Calling gun violence a public health crisis is a ‘first step’ to fight it
Three public health experts weigh in on a new U.S. effort to treat this as a health problem
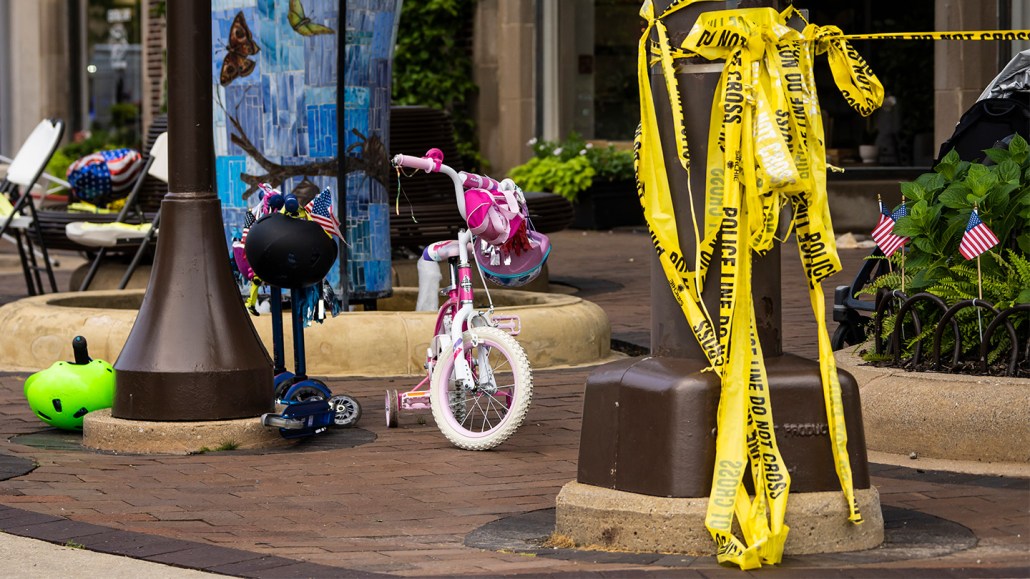
Two years ago, a gunman in Illinois fired a rifle into a crowd celebrating the Fourth of July, killing several people. The incident is part of the larger problem of gun violence in America, which has now been declared a public health crisis.
Ashlee Rezin/Chicago Sun-Times via AP