What consumer DNA data can and can’t tell you about your risk for certain diseases
Consumers face lots of choices and unanswered questions

RISKS AND RIDDLES Now that Lara Diamond has been through a cancer diagnosis, she advises others on how to deal with the personal health information uncovered in genetic testing.
Matthew Rakola
Results from Family Tree DNA, a genetic testing company, helped Lara Diamond find a branch of her family she thought had been lost in the Holocaust. Those 2012 results brought dozens of new people into her life.
Eager to find more relatives, Diamond, now 42, a professional genealogist in Baltimore, decided to try out all the companies that offer geneaological DNA testing to see what else she could learn. Results from one of them, 23andMe, hit her with an entirely different kind of life-changing knowledge: a high risk for breast cancer.
Browsing through the health and trait reports the company provides, Diamond reached the locked reports, which contain information about genetic variants that increase risk for developing breast cancer, Alzheimer’s disease or Parkinson’s. Customers have to choose to “unlock” that information since it can bring upsetting news.
Diamond considered her family history. “Because we have Alzheimer’s and Parkinson’s in my family, I said, ‘OK, I’ll think about those. But we don’t have breast cancer, so I’ll open this BRCA thing,’ ” she says, referring to the family of genes linked to breast cancer.
To her shock, Diamond learned she has a variant in her DNA that alters one amino acid in the BRCA2 protein, putting her at high risk for the disease. “One little stupid mutation. One amino acid. And it changes your whole life.”
The next morning she called her doctor, who sent her to a genetic counselor. The counselor ordered a confirming DNA test from a lab certified to do medical diagnostic testing. Diamond also got a mammogram, an MRI, an ultrasound and blood work to screen for breast, ovarian and pancreatic cancers, because her variant boosts risk for all three. The MRI revealed a tiny spot of cancer deep in her breast, too small for the mammogram to detect. She decided to have a double mastectomy.
Her doctors are urging her to have her ovaries and fallopian tubes removed as well, to head off ovarian cancer. “I’m not ready to do that yet,” Diamond says.
Diamond had been mostly interested in what her genes could reveal about her family history, not the health information they hold. But millions of genetic testing customers want to know their medical future. Even though most consumer genetic testing companies collect data on thousands of gene variants that may have an impact on health, companies such as 23andMe are allowed to give only limited information about genetic health risks. The companies’ reports focus mainly on ancestry or basic physical traits (SN: 5/26/18, p. 20).
So the marketplace has devised a work-around: Consumers who want to know about their risks for diabetes or several other diseases can turn to third-party services to analyze the raw DNA results generated by testing companies. New research suggests, however, that some of the answers people find through these third-party services are wrong and could prevent people from listening to their doctors or genetic counselors. That is, if the person bothers to go see one.
The market responds
Diamond got her health-related results in 2013, just before the U.S. Food and Drug Administration told 23andMe to stop giving consumers health information. The company had to demonstrate to the FDA that the information it provides is accurate and communicated in an easy-to-understand way. In 2017, 23andMe won approval to slowly add back reports for certain health conditions.
Most recently, in March, the FDA granted approval for the company to tell customers if they have one of three genetic variants in the BRCA1 and BRCA2 genes. Those three variants are responsible for about 74 percent of inherited breast cancers among people of Ashkenazi Jewish heritage. Less than 0.1 percent of people of other ethnicities carry these variants.
Offering information on only three variants, when there are thousands in the two genes that increase risk for breast and ovarian cancers — as well as melanoma, prostate and pancreatic cancers — is troublesome, say health care providers, breast cancer advocacy groups and others.
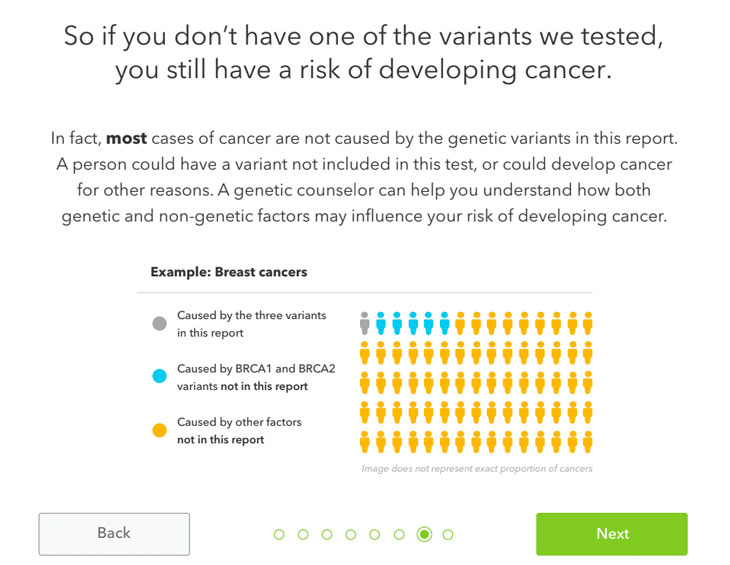
With only a partial list of variants called out, test takers who don’t carry one of those variants may misinterpret the results, worries Lisa Schlager, vice president of community affairs and public policy for FORCE, a hereditary breast cancer information and support group.
People who don’t carry one of the variants may say, “I don’t have a genetic risk that predisposes me to cancer. I’m safe,” Schlager says. “But that is absolutely not correct; you are only negative for three out of thousands of possible mutations. So our concern is that the public is not going to understand the limitations.”
Yet Schlager and others admit that allowing companies like 23andMe to provide FDA-approved information and explain the results — however incomplete — may be the lesser of two evils.
“There’s a sort of underworld that’s been going on since the FDA stopped 23andMe from interpreting these results and giving them out to people,” Schlager says. For a small fee, third-party analysis services stand eager to offer the interpretation that testing companies choose not to provide, or aren’t allowed to provide under FDA rules. These services include Promethease, an early player in the consumer raw data analysis market, along with Genetic Genie, LiveWello and many, many others.
That’s possible because customers of direct-to-consumer DNA testing services such as 23andMe, AncestryDNA and Family Tree DNA can download their raw DNA data to send to third-party analysis sites or apps. Those raw data consist of a list of spots, known as SNPs (pronounced “snips”), where customers’ DNA varies. Some third-party analysis services will also look at a wider swath of information, data on protein-coding regions, called the exome. Genos is one testing company that provides raw data on the exome.
Helix, a testing company that provides “exome plus” data, has partner apps that customers can buy to analyze limited sets of their data. (Or, for $499, you can download all of your raw data). So far, very few of the third-party analysis services are set up to process data from the entire genetic instruction book, or genome.
To write their reports, Promethease and the others find scientific studies that mention the genetic variants a customer carries and make inferences about the health risks of carrying those variants. “That has been an absolute nightmare,” Schlager says. Consumers don’t understand the information and often overreact.
Devil in the data
In Facebook groups for people with BRCA mutations, Diamond, who volunteers with FORCE, often encounters people who got a scary result from a third-party analysis site. “I have to talk a lot of people off the ledge,” she says. “They will upload their data and these services tell them, ‘You’re BRCA2 positive.’ They understandably freak out.” Many of those people would get an entirely different answer from medical diagnostic testing, she says.
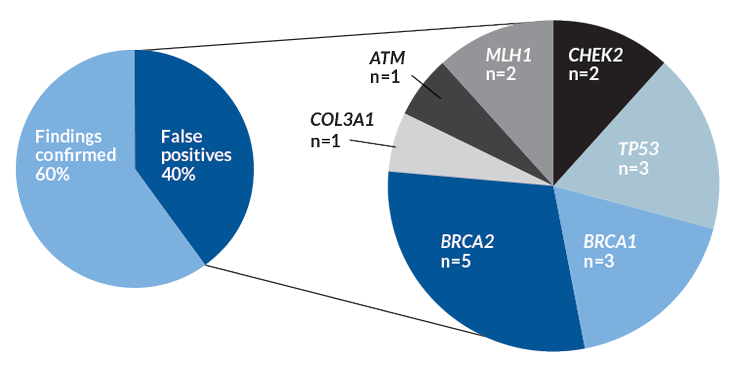
Diamond makes a good point, says Stephany Tandy-Connor, a genetic counselor at Ambry Genetics in Aliso Viejo, Calif., the kind of clinical diagnostic company that doctors use for testing. She and colleagues examined test results of 49 people who received worrisome reports based on raw data generated by direct-to-consumer genetic testing companies between January 2014 and December 2016.
The people had gotten a doctor’s order to get retested by Ambry. The company did comprehensive testing of the supposedly faulty genes. More than half of the harmful variants (60 percent) flagged by consumer tests were verified by Ambry’s clinical test. The problem was, 40 percent of the harmful variants were false positives, the researchers reported March 22 in Genetics in Medicine. The results misstated that the people carried the variant when they actually didn’t.
The fault doesn’t lie with the third-party analysis service, Tandy-Connor says. Those companies simply analyze the raw data received from consumer testing companies. The errors were in the raw data. Often the testing companies are aware of the mistakes, but when they don’t use that information themselves, they don’t always bother clearing errors from the raw data, Tandy-Connor says.
Plus, the raw data don’t contain a full draft of a patient’s genome, as some consumers mistakenly think, Tandy-Connor says. Those data report only a few genetic spelling variations. Clinical testing labs, such as Ambry, use several methods to examine and reexamine disease-related genes to uncover all possible harmful variants. If each gene is a chapter in the body’s instruction manual, clinical tests read every letter in that chapter hundreds to thousands of times, Tandy-Connor says.
Clinical labs also check to see if paragraphs or even pages have been ripped out or glued into the chapter. Such missing or added information, known as structural or copy number variants, might affect more than one gene (SN: 4/25/09, p. 16).
Contrast that approach with the genotyping, or SNP testing, provided by 23andMe, AncestryDNA and many other direct-to-consumer companies. “Basically they don’t read the whole chapter,” Tandy-Connor says. “They just spot-check three or four letters and don’t even look at the rest of it.”
Filling a gap
In 2006, even before 23andMe started offering consumer DNA tests, geneticist Greg Lennon and bioinformatician Mike Cariaso wanted to learn more about their own DNA. The two compiled SNPedia, a Wiki-style database of SNPs that are linked to diseases and traits in the scientific literature. Lennon and Cariaso’s app, Promethease, uses SNPedia to compile reports about the genetic variants in a user’s raw data.
The reports consist of long lists of variants with a description of what the scientific literature says about each variant. So even though 23andMe and other companies may not be allowed to give customers that information, Promethease can. Lennon says the difference is that his service doesn’t generate any DNA data. He simply serves up scientific literature pertaining to the data.
“If the science is credible, we’ll tell you about it,” Lennon says. “We are not going to suppress information.” It’s then up to the customers, their doctors and genetic counselors to decide how to proceed. “The flip side is that it’s easy for someone to misinterpret what they see in a Promethease report and panic over it,” he admits.
Consumers shouldn’t just assume that the information contained in their raw data is correct, or that third-party services have interpreted it correctly, Tandy-Connor says. In fact, genetic testing companies say buyers should beware of using raw data as medical information.
“Uninterpreted raw genotype data, including data that are not used in 23andMe reports, has undergone a general quality review. However only a subset of markers have been individually validated for accuracy,” Dave Hinds, a statistical geneticist at 23andMe wrote on April 23 in an “Ask Me Anything” forum on the website Reddit. <
Genetic results should be confirmed in a clinical lab, Tandy-Connor adds. And, importantly, the information needs to be evaluated in the context of a person’s overall health and family history. “Take it to your doctor. Take it to a genetic counselor or some other genetic professional,” she says. “Certainly don’t act on it. Don’t schedule any surgeries or screenings until you can talk it over with a professional.”
Lennon doesn’t quibble with that advice. “We are 100 percent in agreement that anything seen in a consumer test should be confirmed,” he says.
But the message consumers take away from the Ambry study could have the opposite effect, he says: encouraging people to ignore the results of a consumer test.
“To say there are 40 percent false positives may dissuade people — people who are really carrying mutations — from having these things clinically checked out,” Lennon says. These people might think their result is also a false positive. “That kind of blanket message is a huge disservice to people who might otherwise have actually gone in and gotten confirmatory screening.”
Tandy-Connor disagrees. “I can see the angle he’s coming from, but I don’t share the same sentiment. I’m fairly confident most people would follow up. I mean, why else are they even doing this in the first place? If you’re not going to do anything about it, what was the point? Just freak yourself out and walk away?” Not likely.
Matters in their hands
Consumers are using these third-party apps, but, according to a recent study, at least some people are taking their results to doctors and genetic counselors, says Catharine Wang, a behavioral scientist at Boston University School of Public Health. In an online survey on several social media sites, Wang and colleagues found that of 478 people who did a direct-to-consumer genetic test, 321, or more than two-thirds, used third-party analysis services to investigate ancestry or health information or both.
About 30 percent of those 321 people shared their results with a medical provider and 21 percent shared results with more than one provider, the researchers reported last year in Molecular Genetics & Genomic Medicine. Wang wasn’t surprised that not everyone brought their results to their doctors. “If you don’t find anything in your results, you’re not going to show it to your doctor,” she says. The study did not determine what percentage of people got a worrying result.
Those people who did tell their doctors about their results weren’t always happy with the responses. Doctors were dismissive, weren’t interested in the results or didn’t know what to do with them, 23 percent of respondents reported. Other times, patients had to educate their physicians about DNA testing. Some consumers went straight to genetic counselors.
In a separate online survey of 85 genetic counselors, about half said that they had been contacted by people who had used a third-party interpretation service, Wang and colleagues reported January 29 in Translational Behavioral Medicine. Counselors reported that patients turned to raw data analysis for several reasons: to get answers about mysterious symptoms, out of curiosity or to find out more about their health risks, including disease risks that the patients might pass on to their children.
According to the counselors, sessions didn’t always go well. “They were encountering resistance from the patient,” Wang says, as the counselors tried to correct misconceptions. Some consumers were overconfident about their knowledge, even when they were wrong. When counselors attempted to explain how DNA testing works and that raw data may contain errors, some people didn’t want to hear it. “Consumers just don’t know these nuances,” Wang says. “Sometimes they’re just not receptive to the information.”
Some third-party interpretation services get into shady territory. LiveWello and Genetic Genie sometimes suggest clients take various vitamin supplements based on variants in certain genes. Some of the supplements are supposed to control DNA methylation, an important part of gene regulation, and reduce levels of a chemical called homocysteine in the blood. DNA methylation is a complex and delicately balanced system. Messing with it could cause problems.
Plus, methylation can’t be gauged by looking at someone’s DNA variants, says Preston Estep III, cofounder and chief scientific officer of Veritas Genetics. “SNPs cannot tell you — no amount of genetic information, actually, can tell you — what the state of your DNA methylation is,” Estep says.
To be fair, the LiveWello website says it is not giving advice and people should talk to their doctors before taking supplements. But the disclaimer is easy to overlook.
The tendency is to think that any change to DNA automatically means disease. But that’s not the case, says Gail Jarvik, a clinical medical geneticist at the University of Washington in Seattle. Some genetic diseases affect a small subset of people who carry the variants. For instance, just 24.4 percent of men and 14 percent of women who have two copies of a variant in the HFE gene will develop hemochromatosis, an organ-damaging iron buildup, Jarvik and colleagues reported in 2015.
Even for DNA changes that are strongly linked to disease, like those in the breast cancer genes, disease is not definite, Jarvik says. About 72 percent of women who carry a cancer-associated variant in the BRCA1 gene and 69 percent of women with a harmful BRCA2 variant will develop breast cancer by age 80, researchers reported last year in JAMA. “But a bunch of these women will never get breast cancer, even if they live a long life,” Jarvik says.
Because of the 23andMe test, Diamond knew her odds of getting breast cancer were high. But until her doctors found the cancer, she didn’t know if she might escape genetic fate.
“During the time between getting the 23andMe results and the cancer results I did a lot of, ‘Do I even want to know this?’ ” Diamond says. Ultimately, she is glad she knew. “They talk about early detection, but this was super early. Nothing on the mammogram. Nothing that you could feel. It’s the best-case scenario for having cancer, I guess.”
Diamond told her extended family that she carries a cancer-causing BRCA2 variant and suggested they get tested, too. Many more people in Diamond’s family turned out to carry the variant than expected for a genetic change that has a 50/50 chance of being passed on to the next generation. “We just lose the coin flip a lot,” she laments.
Diamond says she never would have known she was at risk for breast cancer if not for the consumer test. She’s now grateful she and her family have the information, but says she’s wary of getting similar information from a third party.
“There’s goodness in being able to get your raw data,” Diamond says. Uploading raw data from one ancestry site to another allows people to find more long-lost relatives. “But when you upload it to these other services to get medical information, that’s what’s more dangerous … because people may interpret it for themselves incorrectly.”