Imagination Medicine
Brain imaging reveals the substance of placebos. Expectation alone triggers the same neural circuits and chemicals as real drugs
Placebos are supposed to be nothing. They’re sugar pills, shots of saline, fake creams; they’re given to the comparison group in drug trials so doctors can see whether a new treatment is better than no treatment.
But placebos aren’t nothing. Their ingredients may be bogus, but the elicited reactions are real. “The placebo effect is in some way the bane of the pharma industry’s existence because people have this nasty habit of getting better even without a specific drug,” says David Spiegel, a psychiatrist at Stanford University School of Medicine.
It all boils down to expectation. If you expect pain to diminish, the brain releases natural painkillers. If you expect pain to get worse, the brain shuts off the processes that provide pain relief. Somehow, anticipation trips the same neural wires as actual treatment does.
Scientists are using imaging techniques to probe brains on placebos and watch the placebo effect in real time. Such studies show, for example, that the pleasure chemical dopamine and the brain’s natural painkillers, opioids, work oppositely depending on whether people expect pain to get better or worse. Other research shows that placebos can reduce anxiety.
The first brain imaging study to show what happens in the brain during the placebo effect was not necessarily aiming to do so. Its goal was to use brain scans to study what happens when people take apomorphine, which is a drug for Parkinson’s disease, a condition marked by a lack of dopamine. The drug brings quick relief but is infamous for its unpleasant side effects of dizziness and nausea. Led by neurologist Raúl de la Fuente-Fernández of the University of British Columbia in Vancouver, the project used PET scans to monitor the activity of the brains of Parkinson’s patients the same day patients took the drug. PET scans are tools to identify where the brain is activated and which brain chemicals are involved in a task.
But patients in the study experienced so many side effects from the drug that the researchers had to cancel the PET scans. De la Fuente-Fernández wondered whether the combination of undergoing PET scans and worry over side effects made some patients react to the drug more strongly than they should have. So he changed the protocol. On scanning days, investigators gave the drug in several injections rather than a single dose. Participants knew that one dose was placebo, but not which one.
That simple adjustment reduced side effects, kept the trial going and led to a Science paper in 2001 showing that placebos trigger dopamine release through the same circuitry as Parkinson’s drugs. This finding was “serendipity, just serendipity,” says de la Fuente-Fernández.
Seeing expectations in action can help scientists understand how the brain carries out the placebo effect. The hope is that such research can point to when, how and why the effect occurs, leading to better drugs and improved clinical care.
Believing is relieving
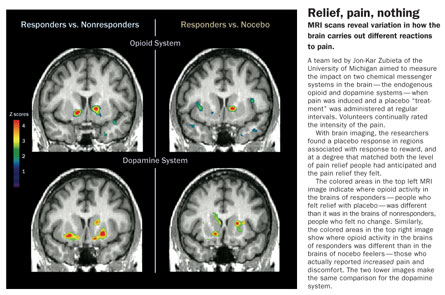
People receiving a placebo in a clinical trial often respond as though they are getting a real drug. At the University of Michigan in Ann Arbor, neuroscientist Jon-Kar Zubieta studies this phenomenon in the laboratory.
Earlier work by Zubieta and colleagues has shown that the anticipation of pain relief discharges opioids from pain control centers in the brain. Opioids are part of the brain’s pain-relief strategy and are activated by stress. Other chemical messengers, such as dopamine, join in too. In the nucleus accumbens, dopamine is released when the brain sees a reward coming, such as food or sex. Dopamine drives the reward response, and Zubieta wondered whether dopamine also participates in the placebo effect.
Modeling the experiments on clinical trials, Zubieta’s team told participants that they would be testing a new medication that would relieve pain by activating the brain’s natural pain-relief centers. Participants were told that they would receive a placebo or the drug. Finally, they were told that they wouldn’t know whether the drug worked or not but that investigators would know because of the brain-scanning equipment.
The scientists then administered the “pain relief” (which did not include, in fact, any actual drugs, only placebo) and exposed participants to pain by injecting low-concentration saltwater into a large jaw muscle for 20 minutes. PET images were taken of the participants’ brains during the exposure. Pain lessened for some and strengthened for others—just what happens in clinical trials, the researchers reported in the February Archives of General Psychiatry.
In participants whose pain symptoms improved, the nucleus accumbens released dopamine and opioids. In those who reported more pain and discomfort, the brain shut down dopamine and opioid release through the same pathways.
But even in such tightly controlled laboratory experiments, not all people respond to placebos, and not all respond the same way. In another experiment, the same volunteers played the monetary incentive delay task, a gambling game. Reward was expected, but not reward in the form of relief from pain. Using fMRI, the researchers monitored neural activity and found that indeed the nucleus accumbens was activated during anticipation of monetary reward. And in each person, that activation was proportional to the person’s capacity for a placebo-generated release of dopamine during the pain experiments, the team reported in 2007 in Neuron.
“Both dopamine release and activity during reward anticipation predicted analgesia,” says Zubieta.
Pain or relief, same network
Pain, Parkinson’s and even anxiety over medicine may seem unconnected, but these conditions share circuits in the cerebral cortex—the part of the brain that evaluates a situation and its consequences—and in the brain stem, a routing area for information going to and from the brain. Think of the brain as a distribution of networks. Each may have a different job but all the regions are connected.
Many brain areas overlap with those involved in pain and stress because pain and mood affect each other. Depression and movement problems are typical symptoms of Parkinson’s disease, and dopamine levels are crucial to both.
Think of these brain areas as networks of reverberating circuits that size up a situation and assign an emotional value, says Tor Wager, a neuroscientist at ColumbiaUniversity in New York City. “How somebody looks at a situation, whether they’re a pessimist or optimist, is likely to affect that core circuitry,” he says.
Wager’s research joins a trio of early studies linking placebos to these brain networks. In 2004, Wager showed that expectations alone bring the prefrontal cortex online even before participants get a painful stimulus.
Earlier, Predrag Petrovic, a psychiatrist at the Karolinska Institute in Stockholm, showed that placebo activates the same brain areas involved in pain relief. Petrovic suspects that the prefrontal cortex sends signals to the anterior cingulate cortex, or ACC, which interprets pain as a threat and activates natural painkillers through a fiber network reaching to the brain stem. “Before, people thought placebos were a passive process,” says Petrovic.
Petrovic and colleagues then wondered whether the placebo response for emotional processing uses the same brain circuits as pain processing. They set up an experiment designed to manipulate anxiety. On day one, scientists gave participants an antianxiety drug and then, during a brain scan, showed photos ranging from scary to neutral. For example, one photo showed a gun pointing at the participants’ faces, another a rolling pin.
The next day, the researchers told participants they would get the same drug and view the same photos. Instead, participants received placebo, and again their brains were scanned while they looked at the pictures. Comparing scans showed that the placebo and the real antianxiety drug activated the same area of the prefrontal cortex and ACC. “We know now that we’re actually activating systems that can either make it better or worse for the patient just by what we tell them and how we tell them,” Petrovic says.
The white, round pill
One reason the placebo response works is because people consciously or unconsciously connect environmental cues and a healing response. The color and shape of aspirin, a doctor’s white coat, the dentist’s chair or a stethoscope form the social context in which the placebo effect occurs.
Fabrizio Benedetti, a neurologist at the University of Turin in Italy, calls these stimuli the psychosocial context, things that “tell the patient that a therapy is being performed.” Aspirin pills are white and round and contain acetylsalicylic acid. Time after time, people take aspirin and headaches disappear, so a link forms between the color and shape of aspirin pills and the effects of acetylsalicylic acid. Before long, people learn to respond to any white and round pill, even one with sugar inside, says Benedetti.
Doctors can bring the placebo effect to the clinic without lying to patients. And doctors can harness the psychosocial context to reduce the intake of dangerous painkillers. Benedetti provides an example: A doctor gives morphine on Monday, Tuesday and Wednesday. On Thursday, the doctor replaces morphine with placebo. Then the doctor repeats the cycle of three days with morphine, one day with placebo. In the long run, doctors can reduce the intake of morphine, which is exactly what Benedetti and colleagues did in a clinical experiment. “We were able to reduce the intake of buprenorphine [a morphinelike drug] by about 34 percent in postoperative pain,” says Benedetti.
The biggest problem with using placebos is ethical because doctors have to convince patients they’re getting a real drug. Benedetti suggests telling patients the truth by saying: “‘I’m going to perform a procedure which is known to activate endogenous analgesic substances in your brain. Thus, your pain will subside in the next few minutes.’ Even though you give a placebo, I believe there is no deception in this sentence.”
Placebos for better drugs
So far, imaging techniques have provided the tools to measure the emotional aspect of medical treatment. Lots of work needs to be done, though, before scientists can fully harness placebo power. Still unknown is why the placebo response sometimes lasts less than an hour and how to make responses last longer.
Almost no system in the brain or body works alone. Imaging research using the placebo effect could help scientists figure out which systems are most important in the human brain, in diseases and in behavior, says Mark Mintun, a radiologist at the Washington University School of Medicine in St. Louis. In Parkinson’s, for example, imaging the effect shows how much the brain depends on the ability to fine-tune the complicated dopamine system. In people with Parkinson’s, disease brings changes to mood and movement. Imaging the effect in this condition could reveal dopamine receptors that influence both reward and muscles, says Mintun.
“We don’t do placebo research just so we can come up with a new therapy,” Mintun says. “Sometimes we have to make sure that we understand what we’re being fooled by. If you find out all you’re doing is activating the placebo network every time you give somebody a drug and tell them how great they’re going to feel, then clearly that drug may not be doing any good.”
Even though imaging has homed in on where in the brain the placebo effect happens, still unknown are the details of what is happening in those regions. Imaging studies have located the placebo effect to areas such as the nucleus accumbens, but this area connects to a number of brain regions. Just locating an area doesn’t explain the role of the connections. The brain usually has multiple ways of achieving things such as movement or pain relief. So the effect may tap into other pathways, says Mintun. Once the pathways are understood, scientists could exploit the effect to help people with conditions that are difficult to treat, such as chronic pain.
“One of the fun steps would be to understand whether the brain mechanisms involved in the placebo effect could give us new insights for how to develop treatments,” Mintun says. “Clearly, if you can make somebody feel better or make them move better by marshaling a new network in their brain, then we could tap into that with drug therapy. We might be able to enhance current therapies or create a brand new therapy.”







