Let there be light
Two separate studies restore vision in humans, mice with retinal degeneration
Seeing the light might now get easier for people with a rare, genetic form of blindness. Some blind mice also offer hope that people who have lost all the light processing cells in their eyes might not have to stay in the dark forever.
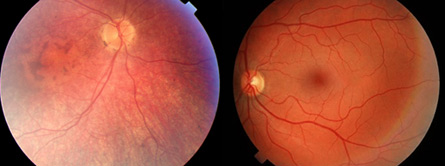
Gene therapy restored sight in three people with an inherited blindness called Leber’s congenital amaurosis, researchers reported online April 27 in the New England Journal of Medicine.
The blinding disease results from mutations in the RPE65 gene, which encodes a protein that helps rod cells in the eye recycle light-gathering pigments. Cone cells work for a while but also start to break down, usually resulting in blindness before age 40. About 2,000 to 3,000 people in the United States have the disease.
Researchers at the University of Pennsylvania and their colleagues injected the right eyes of three people who have the degenerative eye disease with a virus containing a healthy copy of RPE65. The patients’ left eyes were not treated.
All three people had improved vision a few weeks after surgery in their right eye. Two of the people were only able to distinguish hand movements before surgery. After treatment, the patients could read up to three lines on an eye chart.
Eye charts are subjective measures of sight, says Katherine High, director of the Center for Cellular and Molecular Therapeutics at Children’s Hospital of Philadelphia, which sponsored the study. But the patients also showed improvement on objective tests. When light was shone in the patient’s treated eyes, their pupils contracted, indicating that their retinas detected light.
“There’s no teaching of that,” High says. “It’s just a reflex.”
None of the patients regained 20/20 vision, says Jean Bennett, a molecular geneticist at the University of Pennsylvania who led the team. But all of them report better vision in dim light and increased ability to navigate.
“The improvement that we might think is trivial makes a big difference for them in terms of the quality of their lives,” Bennett says.
A second group of researchers from England report in the same issue of the journal that they failed to improve sight in three other patients with Leber’s congenital amaurosis using a similar technique.
A Swedish briard dog named Lancelot got this gene therapy for the eye disease in 2000. He can still see as well now as he did just a few months after treatment, Bennett says. The human patients in the trial can expect similar longevity of vision improvement, she says.
The researchers plan to try the gene therapy in younger patients who have healthier retinas.
Using a different method, an international team of scientists restored vision in mice that had lost all the light-detecting rods and cone cells in their retinas. Those photoreceptor cells detect light. Without them mice and other animals, including humans, can’t see. The results were published online April 27 in Nature Neuroscience.
Once the photoreceptor cells die, as happens in diseases such as retinitis pigmentosa or macular degeneration, there are few options for restoring them. Some researchers have tried stimulating retinas with electricity, a la the visor worn by Geordi La Forge in Star Trek:The Next Generation.
In 2006, scientists at Wayne State University in Detroit reported that they had inserted a gene for a light-gathering protein from a species of green algae, Chlamydomonas reinhardtii, into the retinas of mice with a disease similar to retinitis pigmentosa. Those experiments showed that the protein enabled the mice’s damaged eyes to send messages to the brain when stimulated by light. But it was not clear whether the algae protein or electrical stimulation of the entire retina could actually restore vision.
Now, Botond Roska, a neuroscientist at the Friedrich Miescher Institute for Biomedical Research in Basel, Switzerland, and his colleagues have taken vision restoration a step further. Instead of introducing the light-gathering algae protein — known as channelrhodopsin-2 or ChR2 — into the entire retina, the researchers inserted it only into certain cells in the retina’s second layer. The secondary cells are called ON bipolar cells because they respond to brightening light, as when lights are turned on. Counterpart cells called OFF bipolar cells react to dimming light.
ON and OFF cells normally pass signals from rods and cones to the brain’s visual center, so directly stimulating the cells should restore vision. Roska and his team show that’s just what happens.
The team used electrical current to infuse a piece of DNA carrying the ChR2 gene into ON bipolar cells. The gene is controlled by a piece of DNA that allows it to turn on only in those cells. The technique produces protein only temporarily, so a more permanent method would be needed to successfully treat humans.
Blind mice engineered to make channelrhodopsin-2 in their ON cells scurry to take cover when exposed to bright light just as normal mice do. Blind mice without the treatment don’t respond to the light.
And the protein is “not just acting as a light sensor, it is activating visual systems in the brain,” Roska says. A second test indicated that the vision-restored mice could make out lines on a rotating drum about half as well as mice with normal sight.
Mice are not visual creatures. The animals use their noses and whiskers to navigate more than they use their eyes. Most people generally can’t tell blind mice from sighted mice just by watching them move, says John Flannery, a neurobiologist at the Helen Wills Neuroscience Institute at the University of California, Berkeley. Even with perfect vision, “they’re not going to be reading The New York Times,” he says.
Researchers will probably need to test the technique in animals that rely more on their eyes than mice do, such as dogs and cats, Flannery says.
Algae proteins have a long a way to go before they make it into human eyes, experts agree. Researchers must first design viruses or other delivery mechanisms that can target the light-gathering molecule only to ON cells.
Even with perfect execution, the technique will not restore normal sight, Roska warns. It may restore the ability to see objects, but probably not color vision, for example.
The algae protein is much less sensitive to light and doesn’t respond as well to changing light as rods and cones, so people will probably also need to wear devices that can even out lighting, Roska says.
Even with such limitations, “any improvement for patients is dramatic,” he says.







