Morphine may make pain last longer
Rat study suggests further drawback to opioids
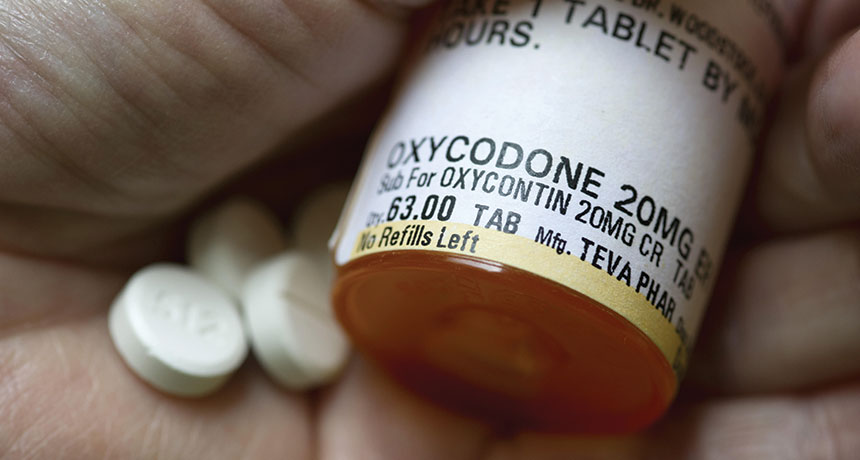
PAIN PILLS Morphine treatment extended the duration of nerve pain in rats, a result that raises questions about the effects of other opioid-based painkillers, such as OxyContin.
ZUMA Press Inc./Alamy
Painkillers in the opium family may actually make pain last longer. Morphine treatment after a nerve injury doubled the duration of pain in rats, scientists report the week of May 30 in the Proceedings of the National Academy of Sciences.
The results raise the troubling prospect that in addition to having unpleasant side effects and addictive potential, opioids such as OxyContin and Vicodin could actually extend some types of pain. If a similar effect is found in people, “it suggests that the treatment is actually contributing to the problem,” says study coauthor Peter Grace, a neuroscientist at the University of Colorado Boulder.
Scientists have known that opioid-based drugs can cause heightened sensitivity to pain for some people, a condition called opioid-induced hyperalgesia. The new study shows that the effects linger weeks after use of the drugs is stopped. Male rats underwent surgery in which their sciatic nerves, which run down the hind legs, were squeezed with a stitch — a constriction that causes pain afterward. Ten days after surgery, rats received a five-day course of either morphine or saline.
Rats that didn’t receive morphine took about four weeks to start recovering, showing less sensitivity to a poke. Rats that got morphine took about eight weeks to show improvements — double the time. “That’s far bigger than we had anticipated,” Grace says. “We were definitely surprised by that.”
These experiments were done with male rats, but unpublished data indicate that morphine extends pain even longer in female rats, Grace says, results that fit with what’s known about differences in how males and females experience pain.
Longer-lasting pain in the rats came courtesy of an inflammatory response in the spinal cord. The immune system sees morphine as a threat, the researchers suspect, and responds by revving up inflammation through specialized cells called microglia. Experiments that shut down this process in microglia shortened the duration of the pain.
Many questions remain. Scientists don’t yet know if a similar immune reaction happens in people. Nor is it known whether all opioid-based painkillers would behave like morphine.
Understanding the details of how the process works has important implications for doctors, many of whom may be unaware of opioids’ complex relationship with pain, says internal medicine physician Jonathan Chen of Stanford University School of Medicine. Clarity on how opioids influence pain could change doctors’ prescribing habits and encourage the search for better pain treatments, he says.
Grace points out that the experiments were done in genetically similar rats, and that people may have more varied responses to opioids. That variability might mean that not everyone would be at risk for such long-lasting pain, he says. “But clearly these data suggest that there may be a subset of people who might be in trouble.”






