Record low for human blood oxygen levels
Challenges in thin air of Everest could inform patient care
Avalanches, vicious winds and sub-zero temperatures aren’t the only extremes endured by those who climb Mount Everest. Hypoxia, a lack of oxygen that can lead to cell death, also threatens. But a study of people ascending Mount Everest’s slopes suggests that some humans are especially tolerant of low oxygen levels, perhaps because their bodies use oxygen more efficiently. The findings, reported in the Jan. 8 New England Journal of Medicine, could inform the treatment of critically ill patients struggling to breathe in hospitals.

The new work reports the lowest recorded blood oxygen levels in a nonhibernating mammal. It is also one of the first analyses to come out of a much larger investigation of more than 200 people who made the trek to Everest in an effort to understand how the body adapts to low oxygen levels.
Patients suffering from cystic fibrosis, septic shock and other critical ailments often have severely low levels of blood oxygen. Treatment often involves administering oxygen with a mask, or mechanically ventilating the lungs, a harsh procedure that can do more harm than good, says Michael Grocott of University College London, lead author of the new study. But because the health of such patients is compromised and many variables are involved, studying the effect of low oxygen alone isn’t easy.
“So many things are going on that separating out oxygen is difficult,” says Grocott. Basic questions still loom, he says. “Why do some people adapt well while others seem to struggle?”
Typically studies of how the body responds to low levels of oxygen are conducted in a hypobaric chamber that simulates the effects of high altitudes. But Grocott’s team surmised that the expense and persuasion required to get 200 healthy people to sit in a metal box for three weeks might be skirted if those people could be convinced to climb the 5,300 meters to the Everest base camp. The Caudwell Xtreme Everest expedition was born. In April and May of 2007 more than 200 people, age 18 to 73, made the trek, making themselves available to more than 60 doctors and scientists aiming to get at why some people fare better than others in the thin air at the tallest peak on Earth.
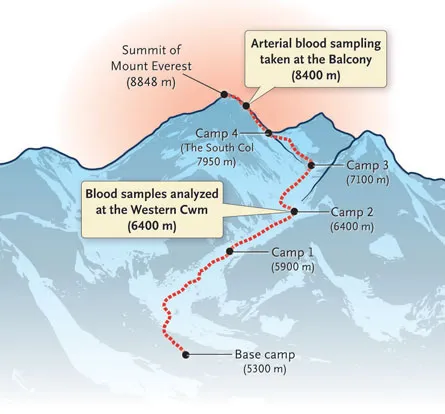
The research team sampled blood, analyzing oxygen and carbon dioxide levels, pH and concentrations of lactate and hemoglobin. Ten subjects were sampled in London (75 meters above sea level). Nine were sampled at the Everest base camp (5,300 m). These individuals, all healthy climbers, then tackled Everest’s southeast ridge. Small shelters were constructed along the route and blood was taken from climbers’ groin arteries. Samples were taken at Camp 2 (6,400 m), from six people at Camp 3 (7,100 m) and finally at what is known as the Balcony (8,400 m) from the four people who made it to the summit and were available for testing (8,848m). Samples taken higher than the base camp were quickly brought to a lab set up at Camp 2 for analysis. Bad weather prohibited taking samples at the summit.
Supplemental oxygen was used only at or above 7,100 m, but samples were only taken after people had been breathing the ambient air for several minutes or hours.
At the highest altitudes, the subjects showed an impressive adaptive response, says Grocott. Most people would pass out after two to three minutes in such altitudes, these climbers were not only conscious, but also clearly communicated by radio and performed complication-free sampling. The blood oxygen levels of the four tested climbers were startlingly low — the lowest a mere 19.1 millimeters mercury, the researchers report. In patients, levels below 60 mm Hg are cause for concern, Grocott says.
The findings suggest that the amount of oxygen alone isn’t the secret to physiological success. Other factors could be how much oxygen a person’s hemoglobin can carry, or the efficiency of the cellular factories known as mitochondria, which use the oxygen.
“There’s a significant possibility that some people may just be more efficient,” Grocott says.
Even among the four climbers tested at 8,400 meters, there was individual variation in measured variables such as blood oxygen levels and pH. This physiological variation among people fits with recent work done by Cynthia Beall of Case Western Reserve University in Cleveland.
“This shows that healthy people have a huge range of variation in being able to respond to stress,” says Beall.
Her investigations of the physiology of Tibetans and other highlanders suggest that a major gene is involved in how much oxygen hemoglobin transport throughout the body. (The Everest team is also looking into the genetics of adaptation to high altitudes.)
Beall tips her hat to the field team. “To have the audacity to think about doing this work — and then to do it! I’m very impressed. The difficulty of taking the measurements alone, and adapting the equipment — they did a beautiful job.”
The results suggest that at high altitudes the problem isn’t the lack of oxygen, but the body’s ability to deliver and use it, comments Paul Firth of Massachusetts General Hospital in Boston. An analysis of mortality rates on Mount Everest by Firth and colleagues appeared in the British Medical Journal in December. “People don’t run out of gas,” he says, “the delivery deteriorates.”







