Why some children may get strep throat more often than others
Tonsil tissue from kids with recurring infections have smaller key immune structures
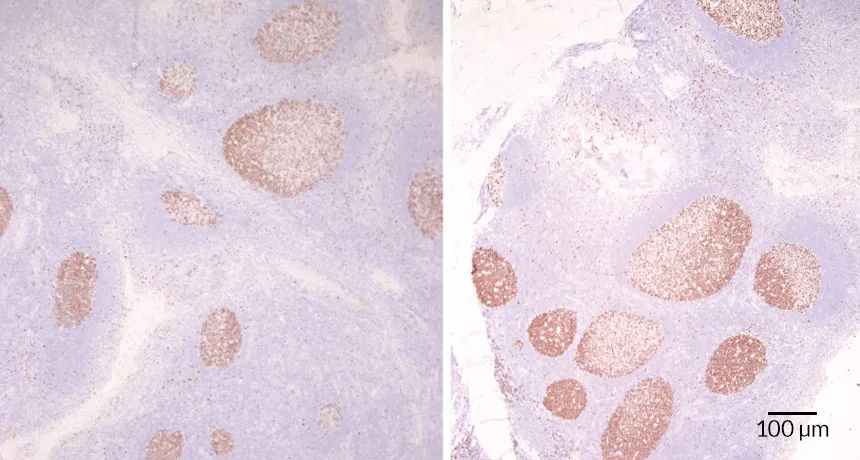
SMALLER CENTERS Certain important immune structures (brown) in the tonsils of children who had recurrent strep throat infections (left in these microscope images) were smaller than those in tonsils from kids who hadn’t had repeat infections (right).
J.M. Dan et al/Science Translational Medicine 2019







