How researchers are working to fill the gaps in long COVID data
To design new studies, researchers are working across specialties and partnering with patients

Researchers studying long COVID are viewing patients’ experiences with the illness as a crucial source of data that can inform future clinical trials.
Gorondenkoff/iStock/Getty Image Plus
It’s been more than two years since the first long COVID patients called attention to their condition. But researchers are still unable to answer basic questions about it, such as how vaccination impacts one’s chances of long-term symptoms or which groups of people are most at-risk, thanks to gaping holes in long COVID data.
Some data gaps originated early in the pandemic. For instance, in spring 2020, people who lacked a travel history to China or didn’t have typical flulike symptoms were unable to get a PCR test to confirm they were infected. So when some of those people later developed long COVID, their initial illness had not been logged in medical records — making it difficult for them to get care and keeping them off most researchers’ radar.
Other data gaps reveal long-standing problems in how the medical system treats complex, chronic diseases. Doctors weren’t looking out for long-term symptoms, despite warnings from experts in other postviral diseases. And some of the most common long COVID symptoms, such as a dramatic worsening of health after exertion, lack a standard code for documentation in medical charts, making them hard to track.
Filling in those gaps is becoming increasingly crucial. Studies suggest that between 10 and 30 percent of people with COVID-19 may experience long-term symptoms, ranging from a simple loss of smell and taste to debilitating cognitive challenges. In the United States alone, that adds up to millions of people who, long after the pandemic ends, may still be dealing with the consequences of the disease.
The urgency of supporting these patients has led to a push for greater collaboration, new technologies and perhaps most important of all, an openness to really listen to long COVID patients, believing in and using their experiences to shape future research.
What is long COVID?
To inform potential treatments, researchers aim to better characterize the causes of and variations in long COVID’s wide range of symptoms. Currently, long COVID tends to be defined broadly (SN: 7/29/22). The U.S. Centers for Disease Control and Prevention characterizes it as a “wide range of ongoing health problems” that can last for months after infection with SARS-CoV-2, the virus responsible for COVID-19.
The electronic health records that researchers use to study long COVID aren’t comprehensive, however, due to gaps in the data. Records often focus disproportionately on people who could get a PCR or antibody test, were hospitalized and had predominantly respiratory symptoms, says Lisa McCorkell, a public policy researcher and cofounder of the Patient-Led Research Collaborative, a group of long COVID patients who also have research experience.
What’s more, records “do not document all of the symptoms the patient experiences,” she says. And for many patients, information about different symptoms can be spread across different healthcare systems, making it difficult for researchers to connect the dots.
“A long COVID diagnosis can mean so many different things in your physiology are going wrong,” says David Putrino, director of rehabilitation innovation at the Mount Sinai healthcare system in New York City and leader of one of the first labs to focus on long COVID. More comprehensive tracking of patients’ symptoms, he says, is crucial to better understand how long COVID presents itself and document how it impacts patients’ lives.
To achieve this goal, experts say, future data collection must be designed collaboratively. Coordination between patients and researchers helps ensure studies are asking the right questions, while coordination between experts with different specialties promotes multidisciplinary, creative approaches to a condition that impacts every organ system in the body. Coordination between research groups in different locations is also important for producing inclusive datasets.
New studies currently in early phases across the United States provide models for how scientists can work with patients and across specialties to investigate long COVID, learning from mistakes made earlier in the pandemic. The results of this work could inform strategies for patients to manage their symptoms and lead to potential treatments.
Asking the right questions
Some of the most influential research on long COVID so far has come from patients themselves, including a 2021 study from the Patient-Led Research Collaborative that documents more than 200 potential symptoms.
“Patients know the right questions to ask to properly document their experience,” McCorkell says. This can include which symptoms are studied, how data are collected from patients and how groups of patients are compared.
For example, one common flaw in research design is that potential long COVID patients might be included in a study’s control group (that is, with the assumption that they do not have the condition) because they lack a positive test result or “do not have the exact symptoms a study defines as being long COVID,” McCorkell explains. Since many long COVID patients — especially those who got sick early in the pandemic — lack positive test results, such a control group can skew study findings because researchers are comparing two groups of people that, potentially, both include patients with long COVID.
To avoid these problems, researchers can solicit feedback from patients during all parts of the scientific process. The Patient-Led Research Collaborative required this type of engagement for applicants to a $5-million research fund run by the collaborative: The winning projects, announced on November 22, were reviewed by a panel of patient experts and will incorporate further patient feedback throughout the research process.
Putrino’s lab is taking a similar approach in setting up a new clinic focused on long COVID and other complex, chronic illnesses. The lab has a “lived experience advisory board” that responds to questions ranging from how the clinic’s waiting room should be set up to how healthcare workers ask patient survey questions, Putrino says.
Surveys have become a particularly valuable tool in long COVID research, filling the gaps left by electronic health records. Health records are “the clunkiest part of this research,” says Arjun Venkatesh, a patient-reported outcomes researcher at Yale University who is investigating COVID-19’s long-term impacts. While new web applications and legislation have made it easier for patients to access their medical records, researchers still face many technical and data security barriers to connecting datasets from different health systems.
Venkatesh and his colleagues use surveys to collect basic information, such as a patient’s vaccine record, as well as metrics that typically wouldn’t be in an electronic health record, such as their fatigue levels over time. In setting up these surveys, it’s important to solicit input from patients, Venkatesh and others say. Filling out a survey could trigger common long COVID symptoms like brain fog or post-exertion pain and fatigue. Responsible researchers ask a small group of patient volunteers to test surveys before they are widely released.
Input from patients is also crucial in designing clinical trials for long COVID, says Julia Moore Vogel, a program director at the Scripps Research Translational Institute in San Diego. People living with the condition have spent time reading studies, comparing notes and testing out symptom management techniques. “There’s actually a decent amount of anecdotal data we can use to inform trials,” she says.
Anecdotal data inspired a study that Vogel, a long-hauler herself, is starting. She is aiming to enroll 5,000 patients who will test how well a wearable device helps them manage their symptoms, using a technique called pacing. Some Garmin health trackers have a feature called “body battery,” which combines several measurements to determine the user’s capacity for exertion. Vogel and other long-haulers use this feature to monitor their activity, stopping to rest when their “battery” gets low. Her new study aims to test the strategy on a larger scale.
Making connections across specialties and locations
The number of people impacted by long COVID is unprecedented. But the condition shares many characteristics with other complex, chronic diseases that arise after infections and affect multiple organ systems, such as myalgic encephalomyelitis/chronic fatigue syndrome, or ME/CFS. These conditions have historically received limited research funding even though they impact millions of people — a problem attributed in part to the diseases’ inability to fit into a specific medical specialty, says Jaime Seltzer, director of scientific and medical outreach at the ME/CFS advocacy group #MEAction, which is based in Santa Monica, Calif.
Funding from the National Institutes of Health, for example, is allocated to research groups through the agency’s topic-focused institutes and centers. “Every disease is supposed to neatly and nicely fit into these categories,” Seltzer says. “And if it doesn’t, everyone goes, ‘It’s not my problem.’” Conditions like ME/CFS and long COVID also are not taught in medical schools, leading to a general lack of awareness among doctors about how to properly diagnose them, she says, which results in incomplete datasets.
To push back against this fractured system, doctors and researchers need to collaborate across specialties, experts say. Scientists with different types of expertise are starting to work together to design comprehensive studies, share data and educate each other about new techniques. The Long COVID Research Consortium is one such group: Researchers with different specialties are investigating the condition’s underlying biology, with data shared across the participating teams.
“We’re going to be setting up our own data-sharing platform,” says consortium member Richard Scheuermann, director of informatics at the J. Craig Venter Institute in La Jolla, Calif. Data from studies of long COVID patients’ microbiomes, immune systems, lungs and other areas will all be in “the same database,” he says, enabling research that connects the different body systems.
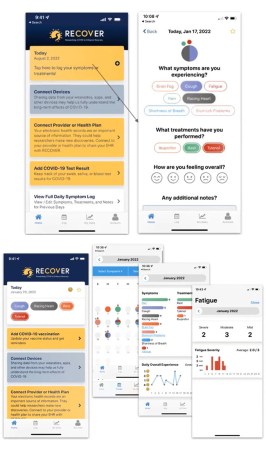
Collaboration between scientists in different places is also crucial to producing research that reflects a diverse patient population. One example is the National Institutes of Health’s RECOVER initiative to learn about the long-term health effects of COVID-19 (SN: 10/24/22).
The initiative’s adult study has recruited about 10,000 people from 53 sites all over the United States and Puerto Rico. But Putrino would like to see the federal government go further by recruiting more patients, collaborating more closely with patient advocacy groups, educating providers and integrating research with efforts to directly help long-haulers, such as aid with disability benefits applications.
Create “a set of common data elements that every site collects, so that every site around the country can contribute to a national registry of people with long COVID,” Putrino says. Such a registry, similar to existing registries for cancer patients, would help researchers better understand the different potential subtypes of long COVID and provide a large population ready to volunteer for clinical trials.
As researchers recruit for large studies of long COVID, they should reach out to communities that are less educated about the condition, says Dona Kim Murphey, a physician, neuroscientist and long-hauler based in Houston. “How do you reach the folks who don’t even know to come to you?” she asks. Public education campaigns about long COVID — combined with easier access to healthcare for people facing long-term symptoms — can contribute to more comprehensive patient datasets (SN: 11/3/22).
Some long COVID researchers are using new technology to better understand the condition, such as wearable devices, survey apps and machine learning for analysis. But models for comprehensive, collaborative research that includes all patients with a complex condition don’t need to be reinvented. As an example, Seltzer points to a 2014 CDC initiative to study autism, in which 11 sites across the country worked together to diagnose children while simultaneously educating clinicians about autism.
“They basically had diagnostic experts in autism train other people to become diagnostic experts in autism,” she says. The study is a model in creating an inclusive dataset, while simultaneously enabling a new group of researchers to better study a condition in the future. Seltzer hopes to see federal agencies enable similar large-scale studies for long COVID and related conditions.
As some long COVID patients enter their fourth year with the condition and more people continue to get infected, moving toward impactful clinical trials is a top priority for scientists. “Design research in a way that’s going to be most effective to the end users, who are the patients,” says Vogel, the Scripps researcher. Going forward, this research model could be valuable for other complex diseases, too.







