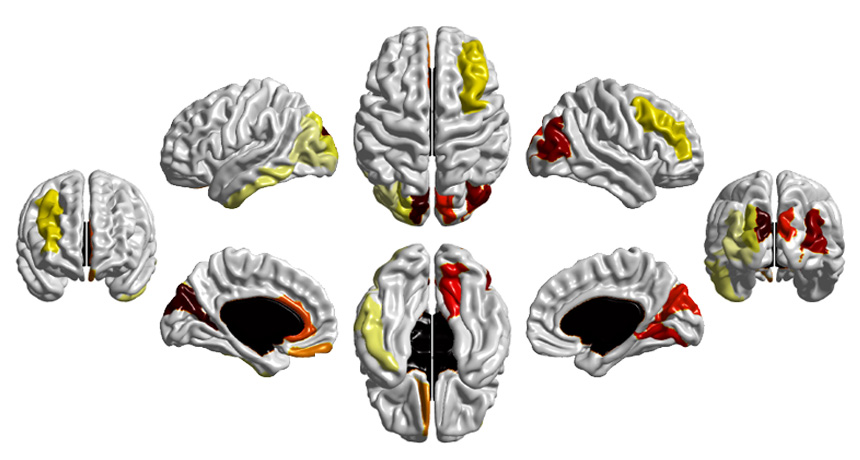
EXPANDING BRAIN High-risk babies — younger siblings of a child with autism — who will be diagnosed with autism themselves had more rapid growth in parts of their brains than low-risk babies who will not later get an autism diagnosis. Darker colors indicate a bigger difference in growth rate.
H.C. Hazlett et al/Nature 2017
Soon after systems biologist Juergen Hahn published a paper describing a way to predict whether a child has autism from a blood sample, the notes from parents began arriving. “I have a bunch of parents writing me now who want to test their kids,” says Hahn, of Rensselaer Polytechnic Institute in Troy, N.Y. “I can’t do that.”
That’s because despite their promise, his group’s results, reported March 16 in PLOS Computational Biology, are preliminary — nowhere close to a debut in a clinical setting. The test will need to be confirmed and repeated in different children before it can be used to help diagnose autism. Still, the work of Hahn and colleagues, along with other recent papers, illustrates how the hunt for a concrete biological signature of autism, a biomarker, is gaining speed.
Currently, pediatricians, child psychologists and therapists rely on behavioral observations and questionnaires, measures with limitations. Barring genetic tests for a handful of rare mutations, there are no blood draws, brain scans or other biological tests that can reveal whether a child has — or will get — autism.
Objective tests would be incredibly useful, helping provide an early diagnosis that could lead to therapy in the first year of life, when the brain is the most malleable. A reliable biomarker might also help distinguish various types of autism, divisions that could reveal who would benefit from certain therapies. And some biomarkers may reveal a deeper understanding of how the brain normally develops.
Scientists are simultaneously sanguine and realistic about the prospect of uncovering solid autism biomarkers. “We have great tools that we’ve never had before,” says psychiatrist Joseph Piven of the University of North Carolina School of Medicine in Chapel Hill. Scientists can assess genes quickly and cheaply, gather sophisticated information about the shape and behavior of the brain, and rely on large organized research collaborations aimed at understanding autism. “That said, I’ve done this long enough to know that people make all kinds of claims: ‘In the next five years or the next 10 years, we’re going to do this,’” Piven says. The reality, he says, is more challenging.
Hahn agrees. “I think it will take quite a bit longer” to find clinically useful biomarkers, he says. “It’s not what parents want to hear. The thing is, this is a very difficult medical disease with many different manifestations.”
Researchers have turned up differences in the brain between people with and without autism, including size and growth patterns, connections between areas and brain cell behavior. But the variability in autism symptoms — and causes — has prompted scientists to look beyond the brain in the search for biomarkers.
“Autism may not be purely a brain disorder,” says neuroscientist Eric Courchesne of the University of California, San Diego. Scientists are looking for important clues to autism in gut microbes, skin cells, the immune system and factors that circulate in the blood.
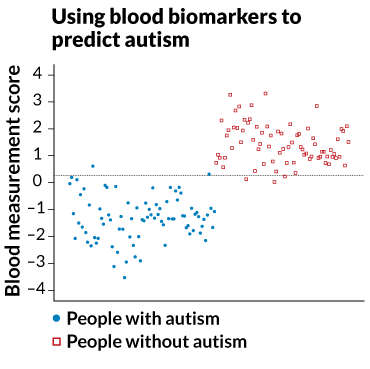
That was the rationale behind Hahn and colleagues’ experiment, which compared compounds in the blood of 83 children with autism to those of 76 children without the disorder. The researchers focused on a group of molecules implicated in autism. These molecules carry out an intricate series of metabolic reactions called folate-dependent one-carbon metabolism and transsulfuration. Earlier work suggested that these processes are altered in people with autism.
Hahn and colleagues developed a statistical tool that examined the relationships between 24 of these molecules. Instead of looking at the concentration of each individual player, the team wondered if a more global view would help. “Could you find patterns in these that give you a much more predictive pattern than if you look at them one by one?” he asks. The answer, their results showed, was yes.
The statistical tool correctly called 97.6 percent of the children with autism and 96.1 percent of the children without. Just two of 83 children on the autism spectrum were misclassified as being neurotypical, and three of 76 children without autism were misclassified as being autistic. Compared with other methods described in the scientific literature, “the numbers we got out were very, very good,” Hahn says.
Those results are “quite interesting as an example of a blood test,” says neuroscientist Dwight German of the University of Texas Southwestern Medical Center in Dallas. But as a researcher who also works on blood-based biomarkers of autism, German is familiar with a huge caveat: Blood can be fickle. Medications, age and even time of day can influence factors in the blood, he says. “There’s an awful lot of testing you have to do to show that what you’re measuring is related to the disorder and not what they ate for breakfast,” he says.
If these metabolic differences are present just after birth, the blood test could be an extremely early indicator of autism. But much more work needs to be done to validate the new approach, including tests on children younger than 3, Hahn says.
Other issues need to be resolved, too. When tested on 47 siblings of people with autism, children who presumably share genetics and environment with an autistic sibling but who don’t have the disorder themselves, the statistical tool’s performance worsened a bit. The tool incorrectly classified four of the 47 siblings as having autism.
For tougher distinctions between high-risk kids like these, scientists have had success looking back to the brain. Recently, Piven and colleagues studied babies born to parents who already had an autistic child. These “baby sibs” have about a one in five chance of developing autism themselves, a rate higher than that of a child without an autistic sibling. By studying this high-risk group, Piven and colleagues have found brain features that are associated with even more risk.
Researchers had suspected that at some point early in life, brains grow too much in children who will go on to develop autism. Piven and colleagues scanned the brains of 106 babies with older siblings with autism at 6, 12 and 24 months of age. The researchers also included 42 low-risk infants.
At 6 and 12 months of age, the 15 babies who went on to develop autism had more growth in the outer surface of their brains, the cortex, than both the high-risk babies who didn’t develop autism and the low-risk babies, the researchers reported February 16 in Nature. A computer program that analyzed brain growth predicted whether these high-risk infants would go on to develop autism. On a second set of babies, the classification performed well, successfully calling eight out of 10 babies who would go on to develop autism by 24 months of age.
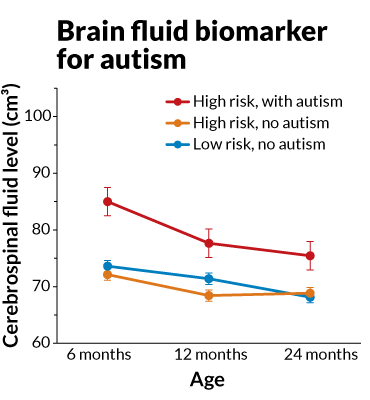
Other work by Piven and colleagues has turned up other brain differences in high-risk babies. Babies who will go on to develop autism have more cerebrospinal fluid on a certain part of the outer layer of their brains than those who don’t develop the disorder. But the results, published online March 6 in Biological Psychiatry, fell short of the predictive power of the brain overgrowth results, Piven says.
Both of these brain scan studies apply only to high-risk babies. It’s not known whether similar tests would work on children without siblings with autism. But it’s possible that these types of detailed findings can help distinguish varieties of autism, and those are distinctions that must be made before scientists can make progress, Piven says. “We call [autism] one thing, but it’s many, many different things. And until we are able to grapple with that in a more meaningful way, it’s sort of an intractable problem.”
Child and adolescent psychiatrist Robert Hendren, of the University of California, San Francisco, envisions a time when this collection of individual disorders collectively called autism are all cataloged in detail, thanks to biomarkers. “We’ll call it autism 23 or autism 14, and we’ll say, ‘We know this is the process that’s going on, and this is how we’re going to personalize our treatments for this person.’”
On the way to that goal, a big breakthrough is unlikely, says Piven. It’s not like the discovery of penicillin for bacterial infections. “You give it, and 10 days later, everything is fine. This isn’t going to be like that.” Even so, the breadth and enthusiasm of the field is promising, he says. “This whole idea of looking at early biomarkers is a new way of thinking, and we have enormous capabilities to make this reality.”