The thymus withers away after puberty. But it may be important for adults
Removing the thymus is associated with higher rates of death and cancer, a new study finds
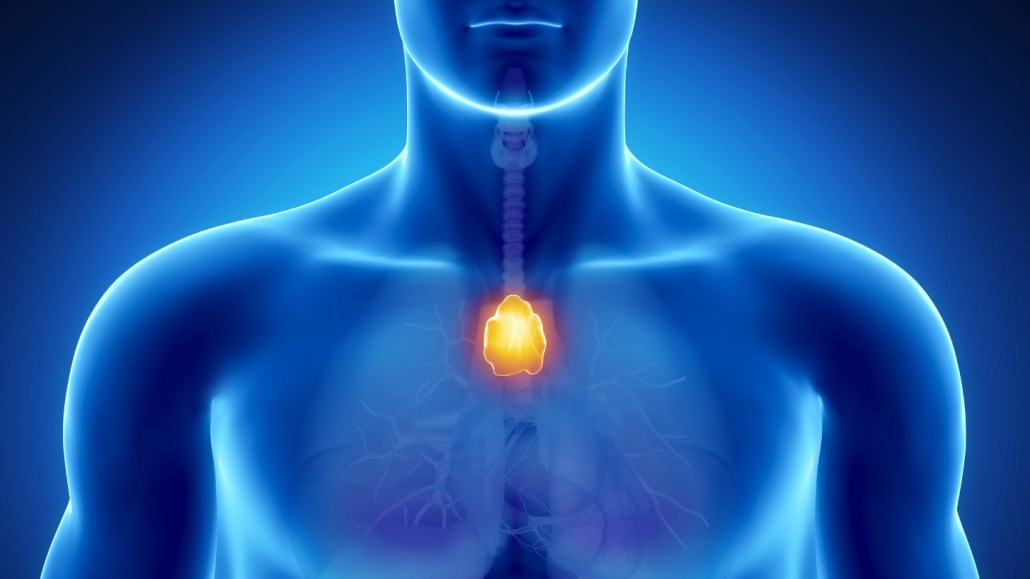
The thymus (orange in this illustration) is an immune system organ that sits between the lungs, right in front of and above the heart. This gland might be more important for adult health than previously thought, a new study suggests.
janulla/iStock/Getty Images Plus
A mysterious organ that’s most active in childhood might play a previously underappreciated role in adults.
In a study of almost 2,300 adults who underwent chest surgery, removing the thymus gland was associated with higher rates of death and of cancer within the next few years, researchers report in the Aug. 3 New England Journal of Medicine. The discovery pushes back on a long-held belief that the immune system organ is somewhat expendable in adulthood.
“This is a really important finding,” says immunologist Dong-Ming Su of the University of North Texas Health Science Center at Fort Worth, who was not involved in the work. Prior to this study, he says, “there was no direct evidence to demonstrate [the thymus’] importance in adults.”
The thymus resides in the chest between the lungs, right in front of and above the heart. In infants, the gland almost completely covers the heart. It pumps out immune cells called T cells, which detect foreign invaders that could cause illness.
But the gland’s activity dwindles after puberty, producing fewer new T cells as we age. Adults mostly rely on memory T cells, long-lived cells that rapidly produce specialized T cells in response to intruders the body has fought before. The thymus gradually wastes away and gets replaced by fat.
“It progressively becomes something that looks like more of a fatty blob,” says hematologist-oncologist David Scadden of Massachusetts General Hospital in Boston. Doctors might excise an adult’s thymus if it contains an abnormal growth, to help alleviate an autoimmune disease or simply because it’s in the way during chest surgery, he says. “It’s often removed because it’s not thought to be very consequential.”
To look at consequences of getting rid of the gland, Scadden and colleagues examined health outcomes in 1,146 patients who had their thymus removed from 1993 to early 2020 at Mass General. The researchers compared those patients’ outcomes with those of an equal number of patients, matched for age, sex and race, who had undergone chest surgery within that time period but kept their thymus.
Within five years after surgery, 8.1 percent of thymectomy patients died compared with 2.8 percent of patients whose thymus remained intact. That means that removing the thymus gland was associated with nearly three times the risk of death from any cause in that timeframe.
Similarly, thymus removal was associated with an increased risk of cancer within five years; thymectomy patients had twice the rate of cancer as patients who kept their thymus. The increased cancer risk, Scadden says, might come from the immune system’s compromised surveillance capabilities.
In a handful of thymus-free patients who developed cancer after surgery and whose blood was analyzed, their T cells seemed unable to identify as many varieties of trespassers compared with T cells from patients who retained their thymus and also developed cancer. Whether the T cells’ reduced repertoire in thymectomy patients led to cancer or was a result of cancer remains unclear, Scadden says.
In patients who didn’t have cancer, infection or an autoimmune disease before surgery, thymus removal was associated with a greater risk of developing an autoimmune disease within five years after surgery, the researchers found. Blood samples from about 20 people in each group hinted that thymectomy might be linked to immune system dysregulation.
“This is pretty striking data,” says immunologist Donna Farber of Columbia University, who was not involved in the study. “You don’t often find these huge survival differences with these kinds of [retrospective] studies.”
But the study can’t explain why or how thymectomy is connected to increased rates of death or other negative outcomes. “We don’t know for sure whether the deleterious effects on health are due to the lack of producing new T cells or some other less well-defined function of the thymus,” Scadden says. And Farber suggests that the thymus removal procedure itself — unrelated to the immune system — could even be the cause.
Still, she says, the new work hints that “maybe even that little bit of active thymic tissue you have [is] playing some role.”







