Better transplants through centrifuging
Removing some antibodies from blood of kidney recipients can improve post-op outlook
Some people languishing on the waiting list for a kidney transplant might see their prospects brighten, thanks to a long-term study that has found a new use for an old technology. By using a centrifuge to spin out troublesome antibodies from the blood of people needing a transplant, researchers have rendered recipients able to tolerate a donated kidney they might have otherwise rejected.
Of the more than 80,000 people on the U.S. kidney transplant waiting list, at least 20,000 are at risk of rejecting a transplant despite standard antirejection drugs, says study coauthor Robert Montgomery, a surgeon at Johns Hopkins University in Baltimore. He estimates that the new procedure could clear the way for 2,000 to 3,000 additional transplants annually. The study appears in the July 28 New England Journal of Medicine.
As many as 30 percent of people in need of a kidney transplant harbor antibodies against specific human proteins found in the donor organ. The antibodies can show up in anyone who has been exposed to foreign tissue via a blood transfusion, a previous transplant or even a pregnancy. These people, whom doctors classify as “sensitized” to other humans’ tissues, require a near-perfect match from a living donor to get a kidney that won’t be rejected — a medical long shot.
In the new study, Montgomery and his colleagues treated 211 sensitized patients with a procedure that patients find similar to kidney dialysis, in which blood is drawn from the body, cleansed and replaced. In this case, the medical team spun and filtered the patients’ blood to remove the offending antibodies. After undergoing this desensitization procedure enough times to clear their rogue antibodies, nearly all of the patients then got a kidney transplant.
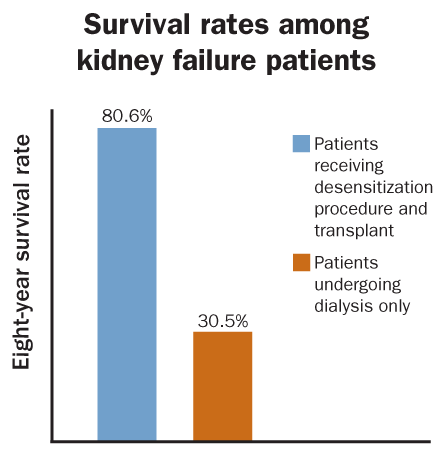
This group had an eight-year survival rate of 81 percent. The rate for 1,050 similar patients who stayed on dialysis over that period without getting a transplant was only 31 percent. A third group of 1,040 patients spent time on dialysis while waiting for a compatible donor, and 14 percent of them did get a transplant during the eight-year study period. Overall, that third group showed eight-year survival of 49 percent.
The desensitization procedure is not unknown to doctors. The Johns Hopkins group surveyed transplant centers and found that about seven in 10 centers had tried it at least once. “This is a very old technique with a new application,” Montgomery says. It has been little-used because clear data on its usefulness had been lacking.
“This validates the approach,” says Dixon Kaufman, a transplant surgeon at the University of Wisconsin–Madison who wasn’t involved in the study. Publication of the new findings will allow more transplant centers to start adding the procedure to their programs, he says. “This is very good evidence that it can provide a benefit.”
It is unclear why some people but not others become sensitized against foreign tissue upon exposure to it, Montgomery says. While these people are easily identified with a standard test, the degree of sensitization varies greatly. This means that while some prospective kidney recipients need to have their blood antibodies depleted only twice, others need to undergo the procedure up to eight times to avoid rejection, he says.







