Brain activity in unconscious patients offers new views of awareness
Using EEG and fMRI, researchers try to learn who is conscious but unable to respond
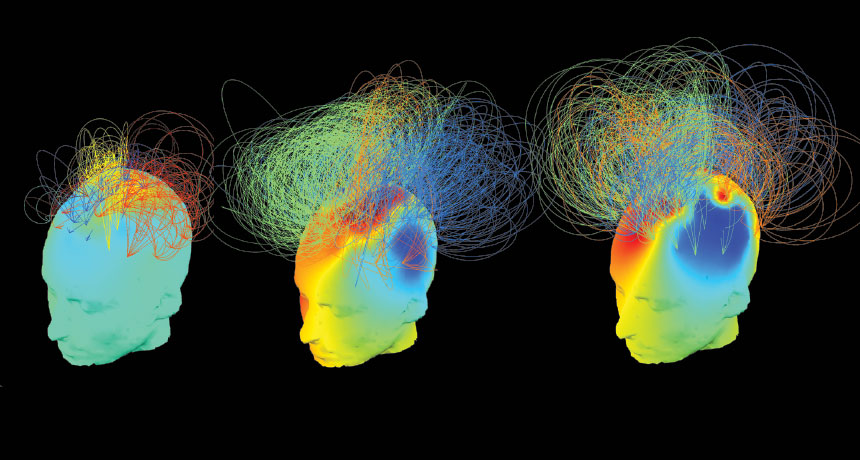
LOCKED IN Patients in the left two images are outwardly in a vegetative state. But the neural connections, measured by electrical activity, are much more active in the middle patient, whose brain network more closely resembles a healthy volunteer’s (right). All three were asked to imagine themselves playing tennis.
S. Chennu/Univ. Of Cambridge
The average brain weighs about 1.3 kilograms and consumes 20 percent of the body’s energy budget. Much of that energy powers the brain’s 86 billion nerve cells, or neurons, which conduct tiny electrical currents that can travel close to 120 meters per second. A typical neuron transmits its signals to about 7,000 neighboring cells and to cells beyond. These neurons assemble into structures responsible for specific tasks. But like individual chords in a symphony, their work blends in seamless harmony. Your visual cortex allows you to see these letters. Your motor cortex controls the movement of your hand to reach for the next page or scroll down the screen. Your prefrontal cortex helps assemble letters into words, words into sentences and sentences into meaning. All you know is that you’re reading.
None of these facts explain one of the greatest mysteries in biology: your conscious existence. The electrical and chemical chitchat among neurons somehow gives rise to awareness, thought, imagination and feeling. Your brain is creating a presence in this moment in a mind that belongs to you alone.
Yet even without consciousness, your body can carry on. Each year, more than 2 million Americans suffer a blow to the head that seriously damages the brain. Another million or so experience cardiac arrest or strokes that deprive the brain of blood, starving nerve cells of oxygen until they no longer function. Some people who survive will be left in a coma, unconscious and unaware of the world around them. Others will live in what’s considered a vegetative state, able to open their eyes and make sounds, but uncoupled from true consciousness. Or so it seems.
“How do I know you’re conscious? If you can say you are, I believe you,” says Srivas Chennu, a neuroscientist at the University of Cambridge. In millions of hospitals, he says, that’s the simple test of consciousness.
It is probably too simple. Recent experiments have revealed a perplexing and profound no-man’s-land of awareness. Outwardly, some patients are in a vegetative state, but brain scans reveal clusters of neurons that appear to form deliberate thought, raising the unsettling possibility of a trapped but cognizant mind.
First verified in 2006 by a brain scan of a woman in a vegetative state, covert consciousness has been sought by researchers among their patients ever since. Scientists are working to develop tests that could reveal silent consciousness and eventually allow those trapped in inert bodies to communicate with the world around them.
Progress has been slow. It’s not possible or practical to obtain scans of the brain as it functions (or doesn’t) for everyone in a vegetative state. But there is hope. Recent studies raise the possibility that the brain’s electrical signals may provide the window doctors need. Brain waves are easy to measure, inexpensive to gather and vary with different states of consciousness. It’s just a matter of figuring out how to read them.
While still experimental, results are compelling enough to raise emotional uncertainties for families of seemingly unconscious patients: the distressing possibility that their loved one may be physically dormant but mentally present.
“We’re coming up on 10 years since the first paper,” says Damian Cruse, a cognitive neuroscientist at the University of Western Ontario in Canada. “It’s broadly accepted that there are patients who are misdiagnosed.” They are in an unrecognized state of consciousness.
The effort to reach them is expected to become even more critical as advances in medicine allow people to live with wounds that a generation ago would have been fatal, says Robert Stevens of Johns Hopkins University School of Medicine, who studies brain injury recovery. Over the last decade, as the survival of patients with severe brain injuries has increased, so has the number of patients with disorders of consciousness, he says. How many people are silently trapped?
Ghost in the machine
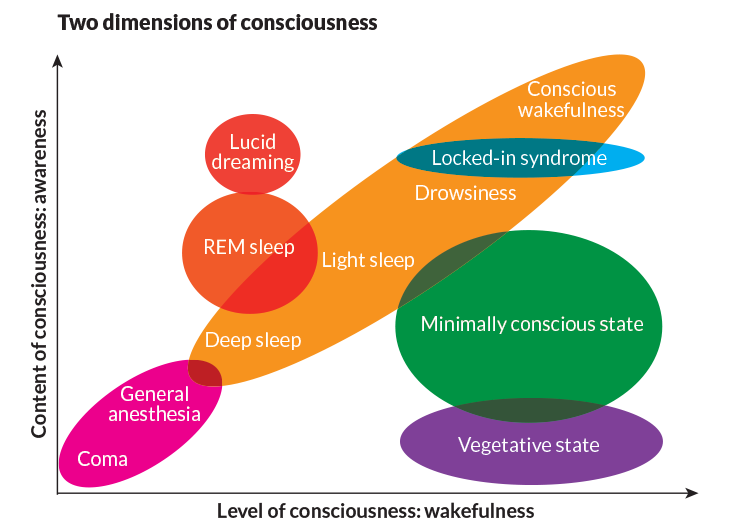
At its extremes, consciousness is easy to discern. A conscious brain is awake and interacting with the environment. An unconscious brain is not awake and not responsive to the outside world (SN: 2/11/12, p. 22). In 1972, neurologists Bryan Jennett and Fred Plum described a condition they named “persistent vegetative state.” In their assessment, a vegetative person wakes for periods of time, but never reaches the capacity for awareness or produces “any adaptive response to the external environment.”
A series of findings over the last decade, though, has people rethinking this definition, to the point that the term itself is falling out of favor. Even as early as the mid-1990s, doctors were finding hints of hidden consciousness in some vegetative patients. In 1996, in BMJ, researchers from the Royal Hospital for Neuro-disability in London suggested that about 40 percent of patients considered vegetative showed some ability to communicate, such as following a simple command to look at an object when their eyes were open.
Still, some saw these flickers of engagement as no more than the brain’s passive, involuntary response to outside stimulation. So a 2006 report in Science was met with great surprise and more than a little skepticism. A team of scientists in England and Belgium used functional MRI to measure blood flow in different parts of the brain, an indicator of neural activity. The experiment involved a 23-year-old woman who had been diagnosed as in a vegetative state following a traffic accident.
Story continues below infographic
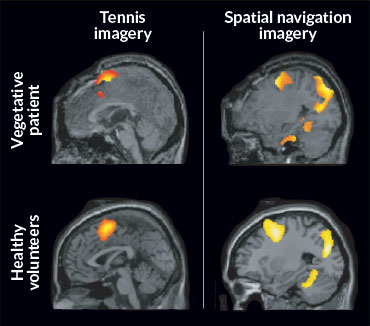
Researchers asked her to perform two tasks while being scanned with fMRI. In one, she was asked to imagine playing tennis. In the second, she was told to mentally walk through all the rooms of her house, starting at the front door.
Asking normal volunteers to play phantom tennis activates the supplementary motor area of the brain, which they would be using if they were on the court. Asking people to imagine going through their houses activates the parahippocampal gyrus (important in memory), the posterior parietal cortex (involved in planning movements) and the lateral pre-motor cortex (which has a role in directing behavior). The brain scans of the supposedly unconscious patient lit up in those same areas. Her scans were nearly indistinguishable from the scans of healthy volunteers.
“This patient retained the ability to understand spoken commands and to respond to them through her brain activity, rather than through speech or movement,” the scientists wrote.
A similar but larger study, published in the New England Journal ofMedicine in 2010, involved 54 patients from England and Belgium with disorders of consciousness. As in the 2006 study, patients were placed in an fMRI scanner and asked to imagine walking around their houses or a familiar city. Five (including the patient from the original tennis study) had brain activity indicating they were experiencing the commands.
The greatest revelation came from patient number 23. The scientists asked patients a series of “yes” or “no” questions (such as, “Is your father’s name Alexander?”). If the answer was yes, the patient was to picture himself playing tennis; if the answer was no, he was to imagine moving around his house. Patients were given the cue “answer” to address a shortcoming of the earlier study — there was a possibility that the word “tennis” or “house” could provoke an involuntary reaction that did not involve deliberate concentration. Patient 23 correctly answered five of six questions.
Evidence of covert consciousness kept building. In 2013, Israeli researchers published a study suggesting that in some vegetative patients asked to imagine their parents’ faces, fMRI showed activity in the brain areas associated with emotion.
Finally, that same year, there was the case of Scott Routley, described in JAMA Neurology. The 39-year-old from Ontario, Canada, had been in a vegetative state for 12 years after a car accident. While in a scanner, Routley was asked yes-or-no questions and told to pay attention to certain words at different times. He was asked yes or no for the question often agonized over: Are you in pain? To the relief of his family, Routley answered “no.” He died a year after the experiment.
The collective conclusion from all of these studies is that some patients are marooned in their own bodies. They can see, hear and contemplate to some degree, but not move or communicate.
Consider the story of Martin Pistorius of Johannesburg, South Africa, author of the 2011 book Ghost Boy. At age 12, he fell into in a coma after an infection. Doctors told his family his brain was permanently compromised and he would never recover. When he was a teen, his brain woke up, but his body did not. No one around him knew he was mentally aware as they fed, bathed and cared for him, and once, in a trying moment, told him they hoped he would die. He lived locked in this way for 12 years before he was finally able to move.
“I couldn’t make a sign or a sound to let anyone know I’d become aware again,” Pistorius wrote in a 2015 Daily Mail article. “I was invisible.” He eventually began to communicate with his eyes, then learned how to use a computerized voice. Today, he is married and working as a freelance web designer.
Making waves
Scientists assume that stories like these, astonishing as they are, represent only a small fraction of patients who are diagnosed as lacking consciousness. Problem is, there’s no reliable way to separate truly conscious minds from those that are fallow or adrift in some state in between. All patients can’t be put into fMRI scanners, which are expensive and difficult to use. The machine requires a person to lie flat, and many patients have bodies that are frozen in rigid contortion. If the brain was injured in an accident, a person may have metal pins and plates for support and so can’t be exposed to the powerful magnets of the scanner. Neither can a patient who has a metal pacemaker.
Even if a person can physically accommodate the scanner, some say a negative result may very well be meaningless. Suppose a patient is conscious, but unable to hear the command? Or “maybe they were just sleeping during the experiment; you don’t know,” says Damien Gabriel, a neuroscientist at the University Hospital of Besançon in France. A negative finding, he says, “just means we weren’t able to measure awareness at that moment.”
As an alternative, or more likely a complement, to fMRI, some researchers are turning to experiments with EEG, or electroencephalography, which measures electrical signals from the brain. Compared with fMRI, EEGs are relatively inexpensive and portable — easy to perform even at a patient’s bedside. Tests can be repeated at different times to help account for undetected sleep. The challenge is figuring out what a “conscious” EEG looks like.
EEG readings come from a series of electrodes placed across the scalp. Each electrode detects the frequency and amplitude of tiny electrical currents generated by the brain. The result is a pattern of wavy lines that reveals something about the state of consciousness. A sleeping brain looks different from an awake brain, and an unconscious brain looks like something else altogether. Computer models can render sophisticated full-color maps of brain waves.
Story continues below infographic
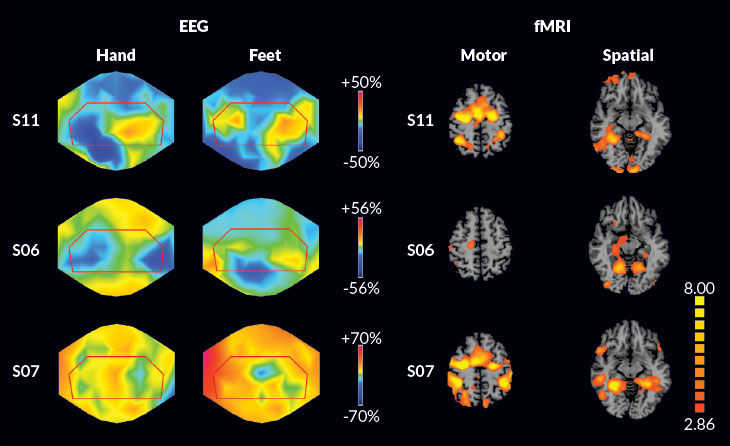
But the electrical approach isn’t without problems. “EEG signals are complicated, and it’s difficult to translate them into a yes or a no,” says Cruse of the University of Western Ontario. In 2011, he and colleagues from Europe reported in the Lancet on an experiment with 16 patients diagnosed as vegetative. The patients were told to imagine themselves doing several things, such as moving their right hand and right toes when they heard a beep. A portable EEG recorded their brains’ electrical activity. The test was repeated on 12 healthy volunteers. In three of the 16 vegetative patients, the brain wave patterns responding to the commands matched the patterns of nine healthy participants, raising the possibility that those three vegetative patients were conscious.
Similar findings with EEG were reported in 2014 in PLOS Computational Biology by Chennu, of Cambridge. Using computer-enhanced images of EEG waves in patients, he and his colleagues found that 32 patients diagnosed as vegetative or minimally conscious showed surprisingly varied levels of active neural connections in the brain; some almost appeared as robust as healthy individuals.
In a testament to the vagaries of EEG interpretation, in 2013 neurologist Nicholas Schiff of Weill Cornell Medical College in New York City and colleagues published a re-examination of the 2011 Lancet data. Their intent was to validate the original findings, not disprove them, Schiff says. But when they took into account factors that could contaminate the original readings, such as involuntary muscle movement, their findings did not support the earlier conclusions.
Last year, however, Schiff and collaborators found that four patients who appeared able to follow commands during an fMRI scan also had EEG patterns that looked normal when they were awake. All four also had one other characteristic on their EEGs: spindles, which are electrical rhythms commonly produced during normal sleep. These healthy sleep patterns could be a signal that brains have some normal function, Schiff and colleagues reported in the Annals of Neurology.
All agree that it’s important for the scientific process to work out the most accurate way to use EEGs for communication with patients, and to explore even tougher questions: What biological mechanisms drive the recovery of consciousness? What are the hallmarks of recovery? Is it possible to revive injured brains? In that regard, Schiff published a study in 2007 in Nature: the case of a 38-year-old man who was minimally conscious following an assault. The man received electrical stimulation to the thalamus, which sits in the center of the brain and connects to many other structures. Most important in this context, the thalamus appears capable of rebooting dormant functions, Schiff says. Following the experiment, the man was able to consistently converse using short phrases until his death six years later. But Schiff has seen little funding for pursuing the work since 2007. “There’s a lot of ambivalence among people who aren’t touched by this problem,” he says.
Those most interested are families, who often carry on with extreme fortitude when their parents, sons and daughters fall into a heartbreaking limbo, Chennu says. “It makes you realize what families have to deal with. You go from having someone with you, to them disappearing, but they are still there,” he says. “We’re hoping these tools will take away some of that uncertainty.” Eventually, he hopes, families will know if their loved ones are truly as vacant as they appear.
The findings also have immediate implications for medical staff and caregivers. “We need to be very, very prudent and cautious about how we behave and what we say in the presence of people we think are unconscious,” says Stevens, of Johns Hopkins. “You can’t walk into a room with a patient and make statements about how they are doing and their prognosis without knowing they aren’t listening in.”
This article appeared in the August 8 issue of Science News with the headline, “Locked inside: As more people survive brain injuries, scientists work to reach patients with hidden consciousness.”