Approval of gene therapies for two blood cancers led to an ‘explosion of interest’ in 2017
CAR-T cell therapy treats patients for whom other therapies haven’t worked
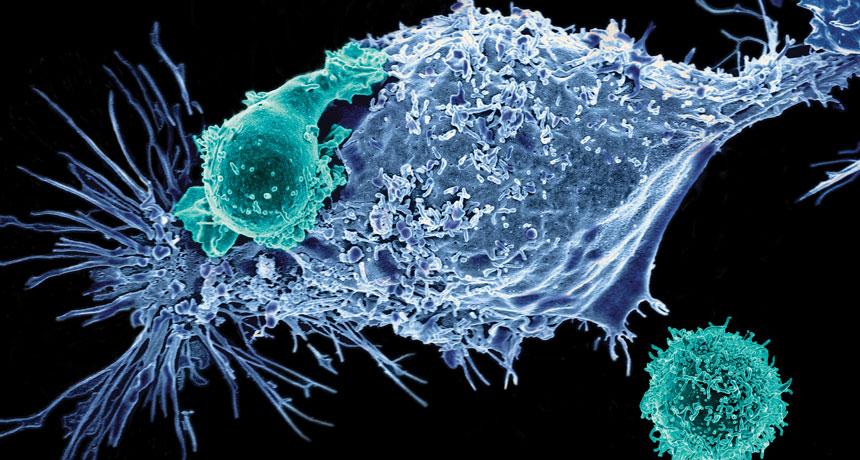
CANCER CRUSH In CAR-T cell therapy, a cancer treatment approved by the FDA this year for certain blood cancers, a patient’s T cells (teal) are genetically modified to hunt down and kill cancer cells (blue).
Prasad Adusumilli, ©2017 Memorial Sloan Kettering Cancer Center