Chronic pain treatments may get boost from high-tech imaging
Brain scans can track protein changes to show whether therapies work
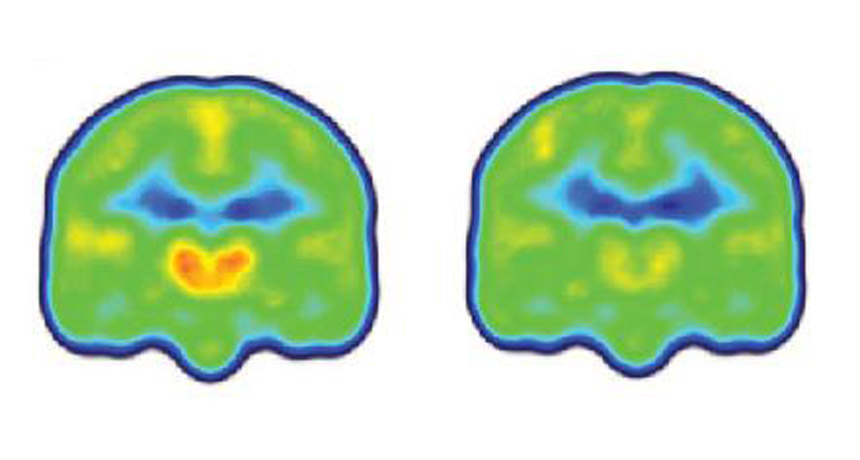
SEEING PAIN People with chronic pain (left) have higher levels of a protein linked with inflammation (orange and red) in their brains than people without chronic pain (right), a finding that could help improve treatments for the condition.
MARCO LOGGIA, MASSACHUSETTS GENERAL HOSPITAL






