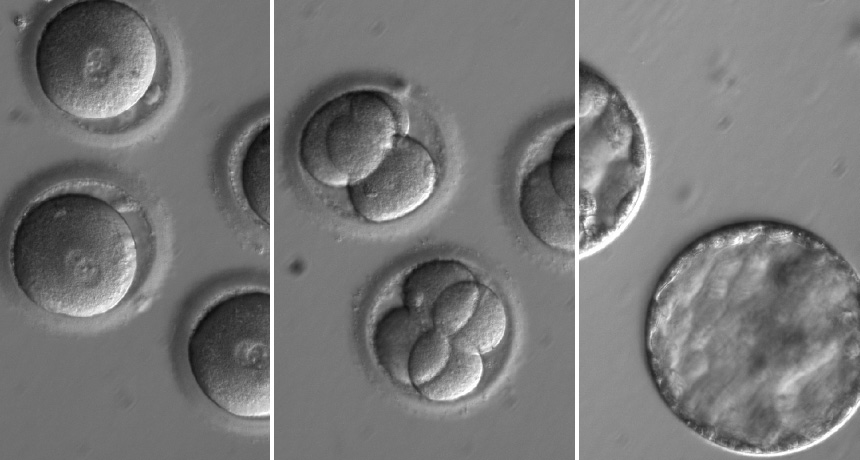
IN GOOD REPAIR CRISPR/Cas9 has corrected a gene defect in fertilized human eggs (left) without hampering embryo development. Four-cell embryos (middle) and blastocyst-stage embryos — about five days old — (right) carrying the CRISPR/Cas9 gene editor appear normal.
OHSU