Gene behavior distinguishes viral from bacterial infections
New approach could gauge response to flu vaccine
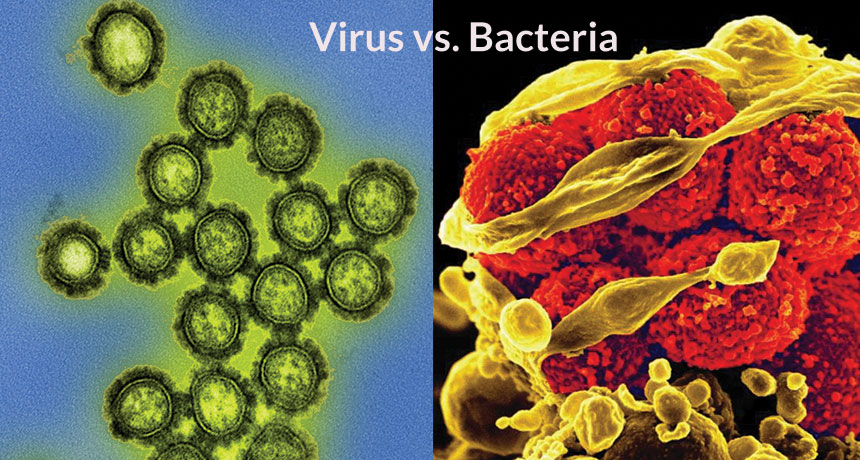
CASING A CULPRIT Certain gene behavior changes in people can reveal whether an infection is caused by a virus, such as the H1N1 influenza virus (left), or bacteria, such as methicillin-resistant Staphylococcus aureus, or MRSA (right).
NIAID/Flickr (CC BY 2.0)