This is how norovirus invades the body
The pathogen targets a rare type of gut cell, a study in mice finds
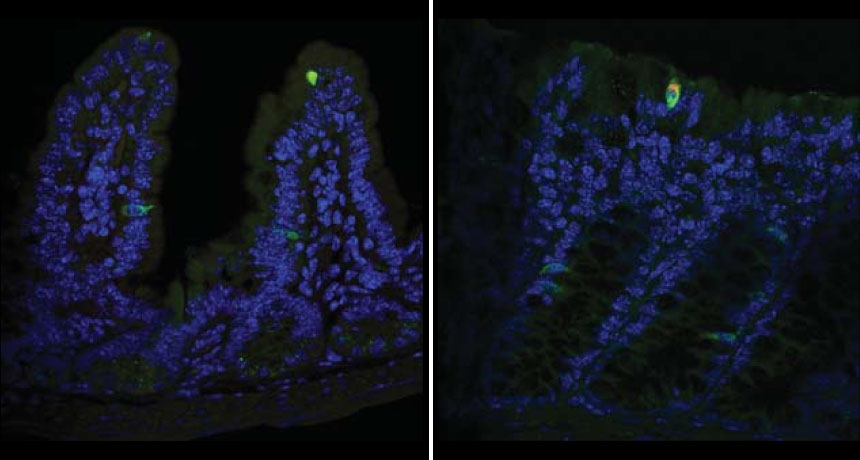
THE WINNER IS… In mice, norovirus invades tuft cells (the two bright green spots) in the lining of the small intestine (left) and the colon (right). Other cells in the intestines that weren’t infected (blue) are also shown.
C. Wilen et al/Science 2018