BOSTON — For the first time, researchers have snapped pictures of mouse inner ear cells using an approach that doesn’t damage tissue or require elaborate dyes. The approach could offer a way to investigate hearing loss — the most common sensory deficit in the world — and may help guide the placement of cochlear devices or other implants.
Inner ear damage and the deafness that results have long challenged scientists. The small delicate cochlea and associated parts are encased in the densest bone in the body and near crucial anatomical landmarks, including the jugular vein, carotid artery and facial nerve, which make them difficult to access.
With standard anatomical imaging techniques such as MRI, the inner ear just looks like a small grey blob. “We can’t biopsy it, we can’t image it, so it’s very difficult to figure out why people are deaf,” said ear surgeon and neuroscientist Konstantina Stankovic of the Massachusetts Eye and Ear Infirmary in Boston.
Stankovic and her colleagues took a peek at inner ear cells using an existing technique called two-photon microscopy. This approach shoots photons at the target tissue, exciting particular molecules that then emit light. The researchers worked with mice exposed to 106 decibels of sound for two hours — levels comparable to the roaring buzz of a snowmobile or power tools. Then they removed the rodents’ inner ears, which includes the spiraled, snail-shaped cochlea and other organs. Instead of cutting into the cochlea, the researchers peered through the “round window” — a middle ear opening covered by a thin membrane that leads to the cochlea.
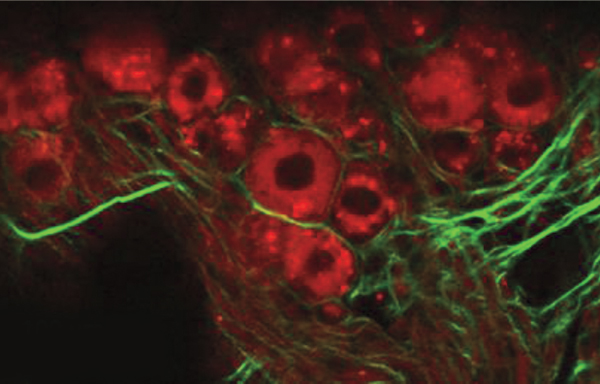
The approach yielded clear images of rows of the inner ear’s hair cells, tiny hairlike structures that detect sound vibrations, enabling hearing. Unlike in control mice, ears of noise-exposed mice had visible damage: Whole sections of ear cells were wiped out, Stankovic reported February 17 at the annual meeting of the American Association for the Advancement of Science.
She hopes the approach will not only shed light on the various kinds of damage that lead to hearing loss, but that it also will help guide the insertion of implants. Placement of a device such as a cochlear implant can scrape ear hair cells and do even more damage, so implants are recommended in only the severest cases of hearing loss.
“Today we do it blindly — we feed it through a hole where it can fold on itself or fracture a membrane,” Stankovic said. “We hope we can make preservation of hearing routine, as opposed to haphazard.”
In the future, the imaging approach might help guide the placement of an experimental device that extracts energy from the inner ear, acting as a tiny battery. The new device, developed by Stankovic and colleagues, doesn’t generate enough power to run a cochlear implant. It could, however, act as a sensor, monitoring for infections or sensing drug levels.
Such devices might prove very useful for monitoring all sorts of physiological responses, says biomedical engineer Philippe Renaud of Swiss Federal Institute of Technology in Lausanne. They could prove especially useful, he says, in patients for whom devices need to be small, delicate and efficient, such as those undergoing deep brain stimulation.





