Iron deficiency goes unnoticed in too many U.S. female adolescents
Nearly 40 percent lack enough of the essential nutrient, and can suffer from dizziness to anemia
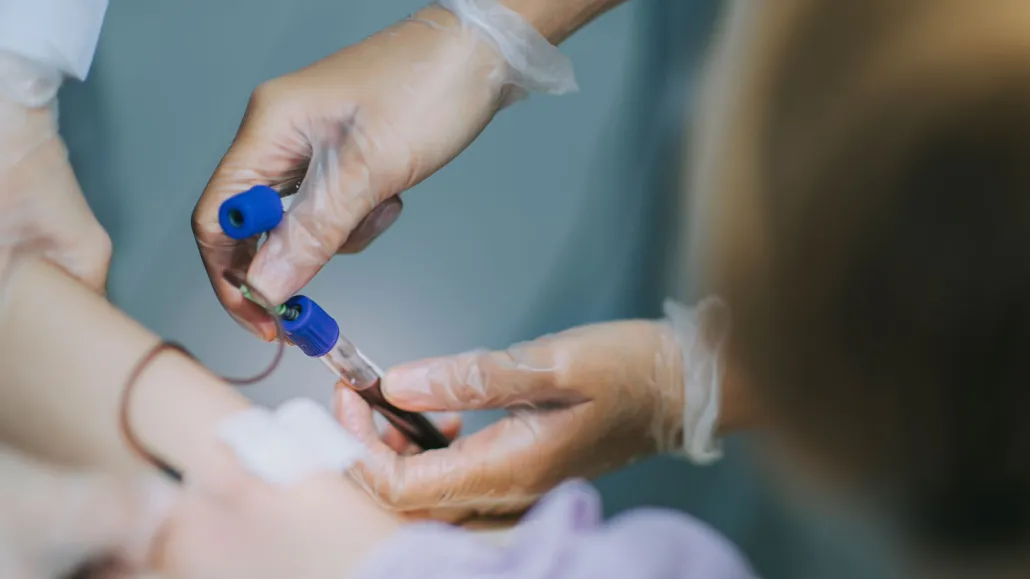
Drawing blood is the most accurate way to screen for iron deficiency and anemia. The U.S. medical establishment should ramp up screenings to help catch more cases in female adolescents, some researchers argue.
Edwin Tan/E+/Getty Images Plus
Many female adolescents in the United States may not have enough iron in their bodies. But most may never know, partly due to a lack of routine screenings as well as disagreement over what constitutes too little iron, pediatric hematologist Angela Weyand argues.
Iron deficiencies are most commonly diagnosed in toddlers, people who menstruate and pregnant people. But Weyand, of the University of Michigan Medical School in Ann Arbor, frequently treats female adolescents for severe cases of the condition. That led her to suspect that its prevalence was being underestimated in that group.
Her analysis of data from thousands of blood samples collected as part of the National Health and Nutrition Examination Survey, which evaluates a nationally representative sample of people each year, suggests the issue is worthy of attention.
Up to 40 percent of U.S. females from the ages of 12 to 21 could be iron deficient, she and colleagues report in the June 27 JAMA. That’s much higher than previous estimates of about 16 percent, which use a lower cutoff point than Weyand’s team did for iron levels.
Iron is an essential component of red blood cells that helps deliver oxygen to organs and tissues. Iron deficiency can cause dizziness, headaches, fatigue, sleep disorders and cold hands and feet. Some of those problems can lead to low work productivity or an inability to multitask (SN: 5/4/04). Severe iron deficiency can also lead to anemia, a condition in which the body doesn’t have enough healthy red blood cells. Anemia can spark more severe issues, such as heart problems or pregnancy complications.
Weyand and colleagues analyzed levels of two iron-containing proteins, hemoglobin and ferritin, in blood samples collected from almost 3,500 female adolescents from 2003 to 2020 as part of the national survey. The researchers diagnosed iron deficiency if the level of ferritin was below 25 micrograms per liter.

Weyand and colleagues used that cutoff based on a previous study on nonpregnant females showing that their hemoglobin levels started to drop when their ferritin levels dipped below 25 μg/L. Hemoglobin is produced in bone marrow and carries oxygen from the lungs to tissues throughout the body. Low hemoglobin is a sign of anemia.
Typically, 15 μg/L is the cutoff used to diagnose iron deficiency, says Laura Murray-Kolb, a nutrition scientist at Purdue University in West Lafayette, Ind., who was not involved in the study. The World Health Organization set that cutoff based on when the body’s iron stores in bone marrow are already depleted. Without enough iron, bone marrow can’t produce more hemoglobin.
But the standard may not be the most effective measure of iron deficiency, Weyand says, because it doesn’t capture “how much iron our [bodies] think we need.” Weyand has treated patients with symptoms of iron deficiency who have ferritin levels above the 15 μg/L cutoff.
In the new study, about 40 percent of participants met the 25 μg/L criteria for iron deficiency. Only 17 percent would qualify based on the 15 μg/L standard set by the WHO, which is roughly in line with previous estimates. Six percent met criteria for anemia, with both ferritin levels below 25 μg/L and hemoglobin levels below the standard cutoff of 12 milligrams per deciliter. Factors such as menstruation, food insecurity or low income increased the risk of iron deficiency or anemia, and Black and Hispanic participants were more likely to meet criteria for iron deficiency than non-Hispanic white participants.
Weyand isn’t surprised that cases of iron deficiency and anemia are so prevalent. Families and medical care providers often brush off symptoms as being a normal part of menstruation, she says, and symptoms can also be attributed to other health issues. “Iron deficiency isn’t necessarily what [primary care providers] are thinking of first,” Weyand says. Taken together, that means cases might go unnoticed and untreated.
The recommendations for iron deficiency screening should be reevaluated, Weyand says. For instance, the U.S. Centers for Disease Control and Prevention recommends that nonpregnant females be screened for anemia every five to 10 years beginning in adolescence but offers no recommendation on screening for iron deficiency.
More research is needed to confirm that the 25 μg/L cutoff is appropriate for widespread adoption in clinical practice, Murray-Kolb cautions. But she agrees that screening recommendations should be reconsidered, especially since screening is so easy to do — requiring a simple blood draw.
The findings underscore just how crucial testing and treatment are for the health of female adolescents even with mild cases, Weyand says. “I’ve seen patients who are really iron deficient and feeling horrible, and we corrected their iron deficiency and their lives really changed.”







