BACTERIAL HEALERS Researchers are using modified versions of disease-causing bacteria to fight tumor cells.
Nicolle Rager Fuller
Normally, you wouldn’t want to have anything to do with Clostridium novyi.
The rod-shaped bacterium is commonly found in soil, manure or under rotting leaves. When it invades a human body, it releases flesh-eating toxins. The last place you would hope to find it is in a hospital.
But researchers used a modified version of this bacterium to destroy an advanced cancer that had spread to a patient’s shoulder. When injected directly into the shoulder tumor, the altered bacterium killed the cancer cells, sparing nearby healthy ones.
Another bad bacterium, Listeria monocytogenes, is a frequent culprit in serious foodborne illnesses. But the microbe is being tested in patients with several types of cancer. Engineered with special tumor-recognition molecules, Listeria prods the immune system into action, marshaling an attack against tumors that the body might otherwise be unable to combat.
True, these bacteria first had to be genetically re-engineered to change their wicked ways. But this unlikely approach, fighting disease with agents known for causing illness, is gaining ground.
Along with the bad bacteria persuaded to do good, some helpful bacteria are being enhanced to treat disorders such as osteoporosis (see sidebar).
“I think the potential is enormous,” says Martin Blaser, a microbiologist and physician at the New York University School of Medicine. “But there’s a lot of homework that has to be done in order to bring this to the clinical realm.”
Dangers disabled
Efforts to develop bacterial-based treatments date back more than a century. In the 1890s, New York surgeon William B. Coley began using a brew made from infectious microbes to treat cancer patients. Intrigued by reports of patients whose tumors had shrunk after a brief bout with a bacterial infection, Coley mixed two strains of harmful bacteria, heating the solution to kill the bacteria. Over the next few decades, Coley and others treated cancer patients with mixed success: Tumors shrank or quit growing in some patients but not in others. By the 1950s, doctors had abandoned the treatment and began using chemotherapy.
Coley hypothesized that infection with his bacterial brew could somehow shift patients’ immune response into overdrive, so that immune cells that rose up to vanquish the bacteria would also attack the cancer cells. Today, scientists are taking a fresh look at bacterial-based treatments to do just that. Live or disabled versions of harmful bacteria are being used to develop therapeutic vaccines for cancer. Unlike typical vaccines, which prevent certain infections before they can take hold, the bacterial-based vaccines train the body to recognize and destroy cancer cells that have already infiltrated.
Case in point: L. monocytogenes, a microbe that contaminates vegetables, dairy products and meat. Infection with Listeria can trigger days of intestinal distress. Some sufferers — especially children, the elderly and people with weakened immune systems — require hospitalization due to dehydration. An infection that spreads to the bloodstream can be deadly.
Microbiologist Daniel Portnoy of the University of California, Berkeley, an expert on Listeria, says the bacterium’s ability to work its way into cells and trigger an intense immune response makes it an ideal carrier for these types of vaccines. While many disease-causing microbes do their dirty work from the outside — injecting toxins into cells — stealthy Listeria enters the cell and then goes to work. When consumed, say, in contaminated cantaloupe or cheese, Listeria makes itself at home after being gobbled up by an immune system cell called a macrophage.
This activity doesn’t go unnoticed by the immune system — which is the point. Some tumors can tamp down the immune system, or even trick immune cells into aiding tumor growth. Fortunately, these are the very cells that Listeria infects. Once infected with the microbe, macrophages signal to other parts of the immune system to respond. The immune system creates an army of T cells designed to attack Listeria. In addition, the immune system creates a “memory” that makes future responses against that strain more efficient.
By knocking out the gene for the ActA protein, Portnoy and his group created a version of the bacterium that can generate a strong immune response without causing illness. Over the last decade, Portnoy has worked with scientists at two biotech companies, including Berkeley-based Aduro BioTech, to turn the genetically engineered microbes into disease-fighting machines.
Recently, scientists at Aduro successfully inserted proteins that recognize pancreatic cancer cells into disabled Listeria. When given to patients, the microbes work their way into cells and spur the immune system into action, as usual. In addition, Listeria expels the proteins, known as tumor-specific antigens, which flag the cancer cells as a danger to the immune system.
In an early trial in patients with pancreatic cancer, the Listeria vaccine in combination with a cancer vaccine called GVAX (composed of tumor cells genetically altered to stimulate an immune response) improved overall survival, shrinking tumors and halting tumor growth. Patients who received the disabled Listeria plus GVAX survived longer than patients who received GVAX alone (6.1 months vs. 3.9 months).
Tom Dubensky, chief scientific officer for Aduro, says about 10 percent of the patients have been on Listeria therapy for more than a year. In July, the U.S. Food and Drug Administration granted the Listeria treatment “breakthrough therapy” status, allowing it to be fast-tracked for development and review by the agency.
In addition, Aduro is sponsoring early phase clinical trials using the same Listeria strain to treat mesothelioma and brain cancer, and plans are under way to develop a treatment for prostate cancer. For each treatment, a tumor-specific antigen is embedded in the Listeria to target select types of tumors.
Listeria can carry a payload of radiation to tumors as well. Scientists at the Albert Einstein College of Medicine in New York City are developing a radioactive form of Listeria to target tumors that have metastasized, or spread away from the main tumor. A team led by microbiologist Claudia Gravekamp and radiologist Ekaterina Dadachova attaches a radioactive isotope of rhenium — commonly used in conventional radiotherapy — to the bacteria. When injected into the abdomen of mice with pancreatic cancer, the radioactive microbes wiped out 90 percent of the metastasized tumors, the researchers reported last year in the Proceedings of the National Academy of Sciences.
“The Listeria does not necessarily need to be inside the tumor cells to kill them since the radioactivity has a cross-fire effect,” Gravekamp says. “That means they can kill tumor cells at a short distance.” Because radioactive Listeria infects only certain immune cells that are attracted by the tumor to help it grow, healthy cells are not harmed by the treatment.
Delivering the goods
Anthrax toxin, from the bacterium Bacillus anthracis, brings to mind envelopes of scary white powder. The thought is frightening for good reason. “Some of the most toxic materials on Earth are produced by bacteria,” says microbiologist Bradley Pentelute at MIT.
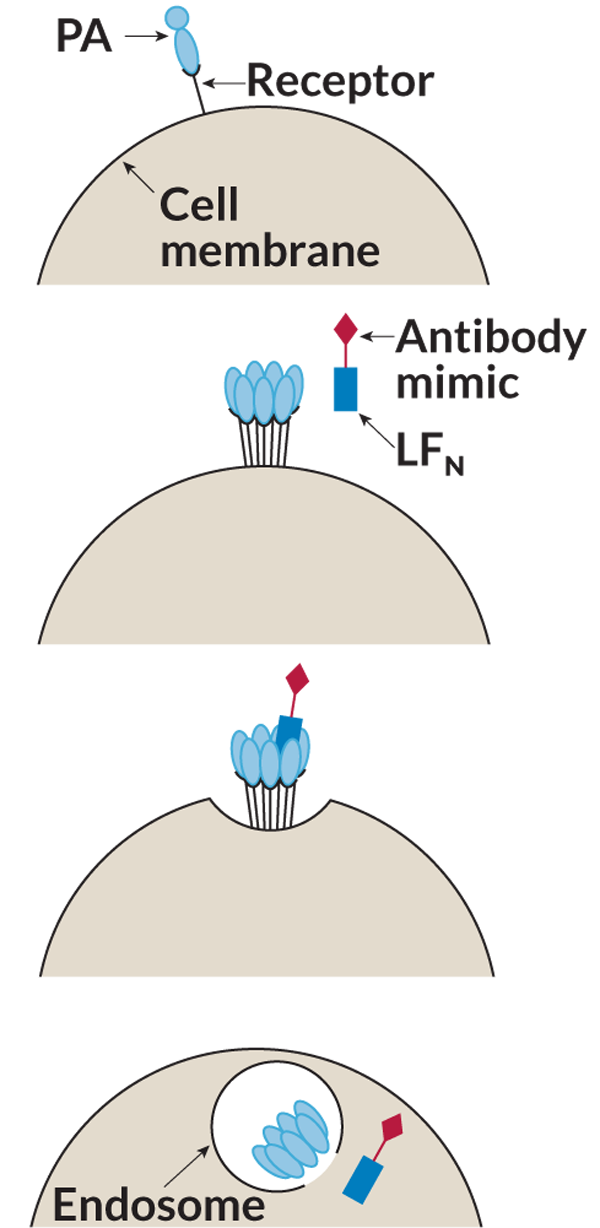
But anthrax may get a chance to improve its reputation as scientists use its destructiveness for good. The toxin works its way into cells, carrying its deadly payload. Pentelute is putting this cargo-carrying feature to work to address a major challenge in biotechnology, delivering therapeutic proteins into cells by getting past the cell’s protective plasma membrane.
Anthrax toxin is composed of three proteins: edema factor, lethal factor and protective antigen, or PA. The PA is nontoxic and carries the dangerous edema factor and lethal factor into a host cell. First, it binds to a receptor on the surface of a cell, latching on “like Velcro,” Pentelute says. Once bound, the PA becomes activated on the cell surface and forms an indentation called an endosome that gets swallowed by the cell. Inside the endosome, the PA rearranges itself, forming a syringelike complex that injects anthrax’s two deadly enzymes into the cell.Pentelute and his team have revised the anthrax toxin to replace one of the toxic proteins with an antibody mimic that targets chronic myeloid leukemia cells. In laboratory studies, the PA protein delivers its cargo of the antibody mimic into the cancer cells, which causes cell death. The researchers published their results online September 22 in ChemBioChem.
Although not yet tested in animals or humans, the system is versatile and can be adjusted to deliver almost any antibody mimic to target any protein, Pentelute says. In his quest to deliver a broader range of therapeutics into cells, Pentelute plans to develop similar systems using the bacteria that cause diphtheria, cholera and botulism, which he hopes will deliver cargo that anthrax can’t.
The bacterium called C. novyi, thrives in places where there is little or no oxygen. Once it finds its way into the body, it can chew through muscle tissue. Molecular biologist Shibin Zhou of Johns Hopkins University and colleagues are exploiting the microbe’s love affair with low-oxygen environs to reach inside clusters of tumor cells, where oxygen is often scarce.
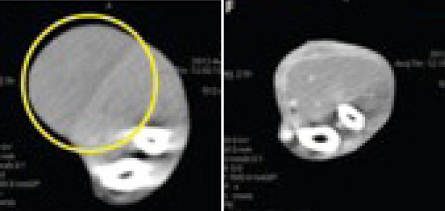
Proving there’s a time and place for everything, the research team, including scientists at BioMed Valley Discoveries in Kansas City, Mo., are genetically altering the microbe, removing the lethal-toxin gene. The new, nonlethal strain, called C. novyi-NT for “nontoxic,” still produces enzymes that eat proteins and lipids in cell membranes. The researchers have injected spores of C. novyi-NT directly into tumors of rodents, dogs and a woman whose advanced cancer had resisted all other treatments.
When injected, two things happened, as the team reported in the Aug. 13 Science Translational Medicine: The bacteria digested the tumor and the infection induced a powerful immune response, bringing the immune cells into the fight.
“This strong immune response, we believe, not only targets the bacteria, but it targets the cancer as well,” Zhou says. After the bacteria was injected into her shoulder, the patient regained use of her arm, which had become immobile. She also developed a fever, severe pain in the injection area and an abscess in the tumor that doctors had to drain. She died six months after treatment due to cancer that had not been treated with the experimental bacteria.
C. novyi-NT is being tested in patients with various solid tumors in a clinical trial conducted in seven U.S. cities. But it will probably work only in tumors with low-oxygen cores, Zhou says.
The early findings are exciting, but some researchers suggest caution. Stanford University biologist David Relman notes that many of the bacterial-based treatments in development need further testing for safety and government approval, especially in cases of genetically engineered strains. And even “good bugs” can have unexpected effects when given in large quantities, he says.
In some cases, Relman adds, scientists don’t fully understand how the microbes work. But he says he’s in favor of pursuing strategies to use them for medicine. After all, certain bacteria have been making people sick since the origin of humans. With the ability to engineer nontoxic strains, these microbes might just change their ways and help conquer disease.
Bone-builders
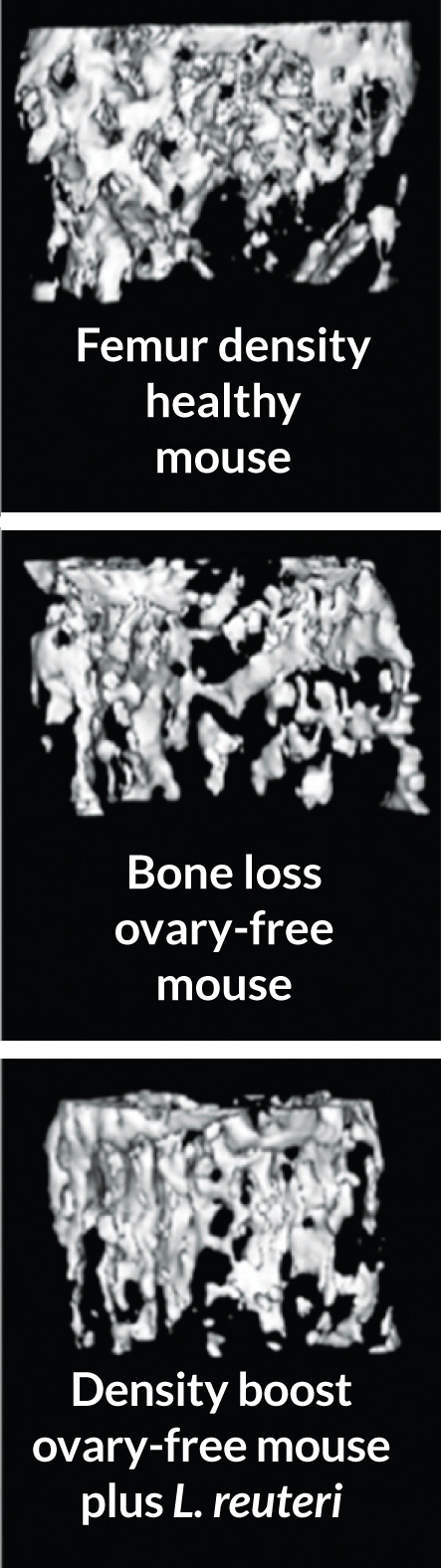
Robert Britton of the Baylor College of Medicine in Houston has found that one strain of the bacterium Lactobacillus reuteri may dial down inflammation, helping to stop the bone loss that occurs after menopause.
L. reuteri is frequently found in the intestines of animals and humans. Different strains of L. reuteri have been shown to promote health by fighting off bad bacteria and producing certain B vitamins. In August 2013, Britton and his group published findings in the Journal of Cellular Physiology showing a probiotic supplement of L. reuteri helps male mice build stronger bones.
L. reuteri also prevents bone loss in certain female mice, the group reported in the November Journal of Cellular Physiology. L. reuteri suppresses the rapid loss of bone that occurs when mice have their ovaries surgically removed to simulate menopause. The bone loss is caused by inflammation within the bone marrow. It occurs at low levels in men and women, but accelerates in women as they age, especially after menopause.
Britton and his colleagues hope to determine how L. reuteri prevents or slows bone turnover. One theory under investigation is that L. reuteri somehow works on an estrogen-receptor pathway. Like menopausal women, the mice with their ovaries removed make less estrogen. Other theories under study: The microbe makes a protein or enzyme that travels to the bone through the bloodstream or perhaps it alters the makeup of the microbiota to tighten what is known as a “leaky gut.”
“As we get older, our guts become more permeable and allow things into our bloodstream that cause inflammation,” Britton says. By calming the gut and suppressing that process, L. reuteri could help stop inflammation and bone loss, he adds. — Susan Gaidos
This article appears in the November 1, 2014, issue with the headline, “Bacterial Healers: Microbes can redeem themselves to fight disease.”