Needling Cells: Stem cells could take their cues from silicon nanowires
The ability to make new heart muscle from a patient’s own stem cells is a dream for many cardiologists. By growing stem cells on a bed of silicon needles, researchers may have found a way to give the cells a push in the right direction.
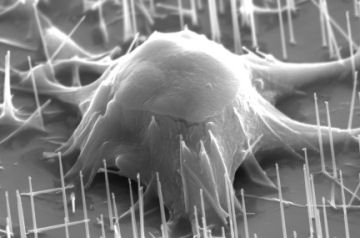
Peidong Yang of the University of California, Berkeley and Bruce Conklin of the Gladstone Institute of Cardiovascular Disease in San Francisco have succeeded in growing mouse and human stem cells that are pierced by silicon nanowires—conducting structures that could give the cells an electrical nudge to spur their development.
Researchers suspect that stem cells require a series of biochemical, mechanical, or electrical signals to form different types of tissue (SN: 3/6/04, p. 155). It’s unclear, however, what mix of cues is necessary to produce any given outcome.
Since heart-muscle cells are electrically active, Yang and Conklin wanted to develop a technique that might enable them to electrically stimulate individual stem cells to become cardiac cells.
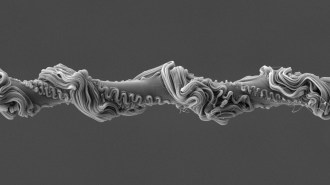
Yang’s group used chemical-vapor deposition to create an array of vertically aligned silicon nanowires, tipped with gold, on a silicon surface. Each wire measured, on average, 90 nanometers wide and 6 microns high.
Next, the team deposited embryonic stem cells from mice onto the bed of nanowires. The wires penetrated the cells without any prompting by the researchers. “Embryonic stem cells are very sensitive to their environment,” says Conklin. “The main purpose of the experiment was to see if the cells would remain alive.”
Indeed they did. When the researchers placed mouse embryonic cells that had already begun to differentiate into heart muscle cells onto the bed of needles, the cells continued to develop normally. In fact, they grew on the surface and continued to beat for up to a month, Yang and Conklin report in the June 13 Journal of the American Chemical Society.
The technology “has exciting potential,” says Timothy McKnight, a bioengineer at Oak Ridge (Tenn.) National Laboratory. Researchers could insert biomolecules—genes and proteins—inside the cells by tethering the molecules to the wires, he adds.
As a proof of concept, Yang and Conklin showed that they could introduce bits of DNA into human embryonic kidney cells. Unfortunately, most of the DNA molecules stayed on the wires. Changing the method of binding DNA to the wires could fix that, the researchers say.
“Nanowire arrays are not . . . representative of anything that really happens in nature,” says Conklin. “But they might allow us to push the cells in new directions.”
The next step will be to use the conducting nanowires to monitor the electrical activity of stem cells and to attempt to control their differentiation into cardiac cells. There are half a dozen different types of heart-muscle cells, each with its own spontaneous beating rate, says Oscar Abilez of Stanford University School of Medicine. He is also growing stem cells on nanowire arrays but has not yet published his findings. Turning stem cells into various types of heart muscle might require using different electrical signals, he suggests.