Potential pain treatment’s mechanism deciphered
Cells from bone marrow give long-term relief to mice with nerve damage
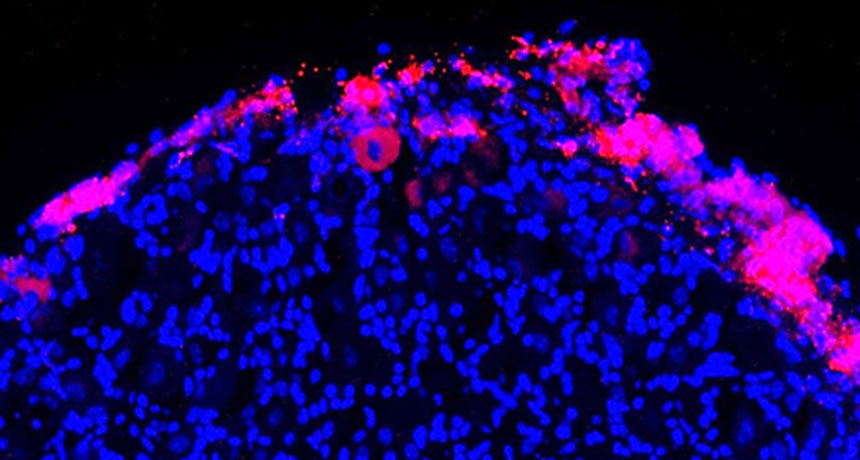
TARGETED TREATMENT Therapeutic cells (pink) extracted from bone marrow can deliver pain-relieving proteins to nerve cells in the spine (blue). The therapeutic cells congregate around injured areas, following chemical signals to damaged cells.
Gang Chen, Duke University