One small step for skin cells could mean one big leap for regenerative medicine. For the first time, scientists have converted adult cells directly into neurons.
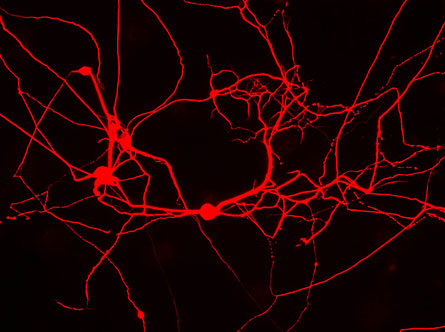
If the technique, performed on mouse cells, works for human cells, the achievement may bypass the need to revert a patient’s cells to an embryonic state before producing the type of cell needed to repair damage due to disease or injury.
Researchers at Stanford University transformed skin fibroblast cells from mice into working neurons by inserting genes that encode transcription factors. Transcription factors are proteins that help regulate gene activity, usually by turning genes on. To convert skin cells into neurons, only three genes for regulatory proteins needed to be added, the team reported online January 27 in Nature. The three transcription factors, called Ascl1, Brn2 and Myt1l, normally appear while new neurons are being born.
Scientists previously thought that this type of flexibility required taking cells several steps backward in development to become pluripotent stem cells, which are capable of adopting nearly any identity. Both embryonic stem cells and other pluripotent stem cells that are created in the lab have these capabilities. The new technique skips the stem cell stage entirely, converting one cell type directly into another.
“It’s quite remarkable that you can jump over so many hills at once with just three transcription factors, and so quickly and so efficiently,” says Marius Wernig, a Stanford stem cell biologist who led the new study. “This really blew me off the chair.”
Perhaps the conversion of skin cells into neurons shouldn’t have come as such a surprise, says Darwin Prockop, a stem cell biologist at Texas A&M Health Science Center College of Medicine at Temple.
“We’ve had fixed ideas about what cells are for a little too long,” he says. “We haven’t thought hard enough about cell plasticity.”
Most of the induced neurons, the team’s name for the transformed skin cells, belonged to a common group of brain cell with many functions. These neurons produce glutamate, an important chemical messenger in the brain that excites other nerve cells. Additional transcription factors may be needed to make other types of neurons, Wernig says.
The induced neurons behaved just like regular neurons, communicating with other neurons in the lab dish and making normal proteins, the team showed. But the scientists don’t yet know whether the cells’ DNA carries normal chemical signatures, known as epigenetic marks, that usually help prevent cells from changing jobs. When altered, these marks can sometimes lead to cancer.
“I believe if you just find the right transcription factors, you can turn anything into anything,” Wernig says. The prospect of making many types of cells in the laboratory is exciting because they could have many applications from transplant to drug testing. Although, he says, “It’s actually a bit scary to think it’s so easy to turn skin cells into neurons because that’s not something you want to happen in your body.”
But other scientists are excited about the prospect of such transformations occurring in the body. “If it’s a naturally occurring repair mechanism, that could be exciting,” says Paul Sanberg, a neuroscientist at the University of South Florida College of Medicine. If such conversions happen naturally, scientists may be able to figure out ways to get the body to heal itself, avoiding the need for transplant.
Because the scientists must genetically engineer the skin cells to make the neuron-inducing transcription factors, the technology probably won’t produce cells for transplant any time soon, Sanberg says. “Once you put in genes, it makes it a little more difficult to use clinically,” he says. Inserting genes might cause cancer-promoting mutations, for example, so scientists may need to develop alternate approaches that would turn on the same transcription factors chemically instead of genetically.
The type of induced cells that Wernig’s group has developed may still be useful as models for diseases and could be used to test new drugs, Sanberg suggests.







