Sunshine vitamin diminishes risk of colds, flu
People with asthma and other preexisting lung diseases face an especially exaggerated year-round risk from a deficiency
Getting plenty of vitamin D — more than diet can offer — appears to provide potent protection against colds, flu and even pneumonia, a new study reports. Although the amount of protection varies by season, the trend is solid: As the amount of vitamin D circulating in blood climbs, risk of upper respiratory tract infections falls.
Though that’s not too surprising (SN: 11/11/06, p. 312), the researchers found one unexpected trend: “In people with preexisting lung disease, such as asthma and chronic obstructive pulmonary disease — or COPD, low levels of vitamin D act like an effect modifier,” says Adit Ginde, an emergency room physician at the University of Colorado Denver School of Medicine in Aurora who led the study. The findings appear in the Feb. 23 Archives of Internal Medicine. In people with lung disease, he says, low levels of the sunshine vitamin “magnify many-fold” the apparent vulnerability to infection seen in people with healthy lungs.
“It’s well-documented that at the turn of the century, kids with rickets [due to vitamin D deficiency] had much higher risk of upper respiratory tract infections,” notes Michael Holick of Boston University. “And treating them with vitamin D lowered that risk. We also know that your immune function is carefully regulated by vitamin D.” For instance, he notes, vitamin D controls the activity of the immune cells that are responsible for destroying infectious germs.
“It’s nice to see that it’s now being documented” with nonanecdotal data, Holick says.
Ginde and his colleagues correlated vitamin D levels of nearly 19,000 adults participating in the National Health and Nutrition Examination Survey with their recent health. NHANES periodically samples a random cross section of the U.S. population; people are selected to be representative of the nation as a whole.
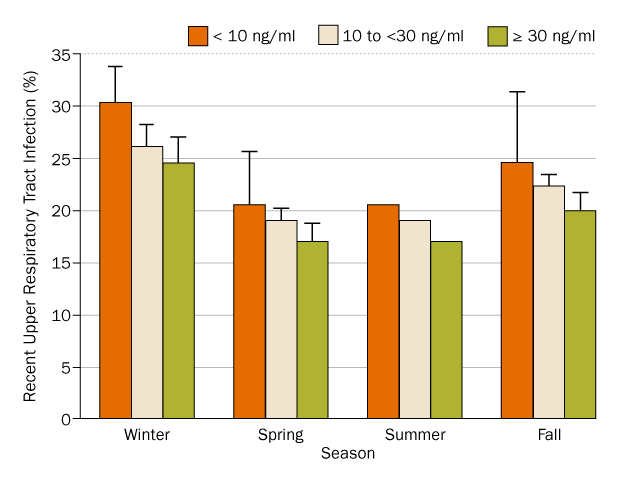
Although no minimum vitamin D level ideal for health has been established, there is a general consensus that people ought to have at least 30 nanograms per milliliter of blood — sometimes described as about 80 nanomoles per liter (SN: 10/16/04, p. 248). In this NHANES data set, only about 45 percent of the population had that minimum. So the researchers separated the NHANES participants into three groups: those with 30 or more ng/ml, those with gross deficiency (less than 10 ng/ml of vitamin D) and those in between.
In every season, people in the lowest vitamin D group were about 36 percent more likely to be suffering a respiratory infection than those in the highest group. Infection risks for people in the middle group fell between those rates.
But low levels of vitamin D more than doubled the risk of respiratory infection for people with COPD — and boosted it almost sixfold in people with asthma — compared with participants who had normal lung function and were in the highest vitamin D group.
Also disturbing, Ginde points out that the NHANES data he analyzed had been collected about 15 years ago, when almost twice as many people as today had vitamin D levels above 30 ng/ml.
Though the body can make plenty of vitamin D as a result of sun exposure, people are spending less time outdoors and covering up when they do go out, so natural vitamin D production has been falling. Ginde and his colleagues plan to supplement high-risk populations during winter months with high doses of vitamin D to see if those people have reduced infection rates compared with untreated people.







