When preventing HIV, bacteria in the vagina matter
Some microbes appear to break down drug in prophylactic gel, making it less effective
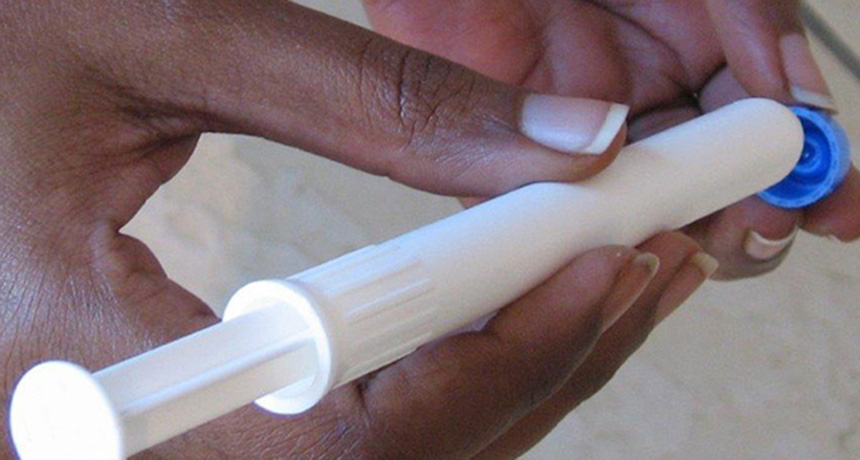
DOSE OF GEL Women use an applicator (shown) to self-administer a vaginal gel containing the HIV-prevention drug tenofovir. Vaginal bacteria affect how well the drug works, a new study suggests.
CAPRISA