Yes, statins protect hearts. But critics question their expanding use
For people who haven’t had a heart problem, the benefit-to-risk balance changes

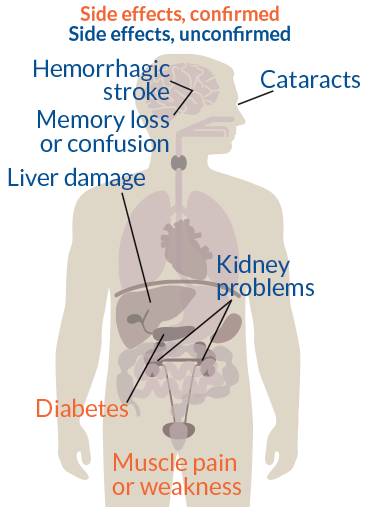
THE STATIN UMBRELLA After decades of study, a big question remains about the safety of statins: What are the risks for people who have a chance of benefit but haven’t yet had a heart attack or stroke?
JAMES PROVOST
Cholesterol is so important to life that practically every human cell makes it. Cells use the compound to keep their membranes porous and springy, and to produce hormones and other vital substances. The body can make all the cholesterol it needs, but Americans tend to have a surplus, thanks in large part to too little exercise and too much meat, cheese and grease. Fifty years ago, researchers began to suspect that all this excess cholesterol was bad for arteries. But the idea remained difficult to prove — until statins came along.
Once the powerful cholesterol-busting drugs appeared, in the 1980s, scientists were able to show that a drop in cholesterol could keep a person who had suffered one heart attack or stroke from having a second. Later studies pointed to protection for even relatively healthy people. Researchers writing in the American Journal of Cardiology in 2010 declared that the drugs were such cardiovascular heroes they could essentially neutralize the health risks from a Quarter Pounder with cheese plus a milkshake.
The news just kept getting better. Studies even floated the idea that statins could protect against cancer and influenza (SN: 5/5/12, p. 30). People joked about dumping statins into the water supply. One pioneering London heart surgeon suggested that the drugs were so good and so safe they should be made available over the counter to everyone over age 40.
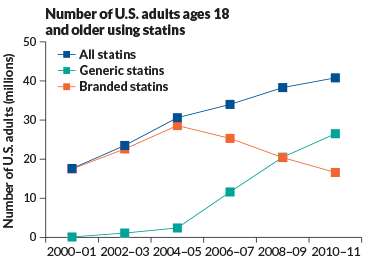
So it may come as a surprise that there are scientists still reluctant to join Team Statin. To them, studies showing benefit for people who haven’t had a heart attack aren’t as clean or overwhelmingly convincing as patients and many doctors probably believe. The statin skeptics worry that too little is understood about unintended consequences, especially for a drug taken for years on end by nearly one-quarter of adults past middle age, according to the Centers for Disease Control and Prevention’s most recent data. After all, only after 30 years of study did researchers discover that statins could raise the risk of type 2 diabetes. Many other sobering but unconfirmed possible side effects appear in the medical literature, including cognitive decline, cataracts and kidney problems.
Muscle damage tops the list of concerns, says James Wright, chairman of the Therapeutics Initiative at the University of British Columbia in Vancouver. “Over time there could be a cumulative effect. I’m predicting we’re going to have an aging population suffering from sarcopenia, where they can’t stand up.” He calls the mass prescribing of statins “the biggest human experiment we’ve ever done.”
In November, a commentary in JAMA carried the headline, “The debate is intense, but the data are weak.” And long-simmering tensions between two major British medical journals recently erupted into an all-out editorial war over the drugs. Rory Collins doesn’t hide his irritation over the enduring controversy. “I can’t think of another circumstance in health care where there is such a lot of nonsense that has been persisting for so long,” says Collins, a medical epidemiologist at the University of Oxford and one of the leaders of the Cholesterol Treatment Trialists’ Collaboration. In his view, statin naysayers are peddling distortions or outright misrepresentations of evidence. Which raises the question: How can respectable scientists see the same data and reach such different conclusions?
At its core, the debate is about how studies are designed, carried out, evaluated and sliced and diced after the fact. No one argues that the vast majority of people prescribed a statin will be taking a drug — probably for the rest of their lives — that they never needed. At issue is whether they stand a good chance of gain, and whether they are putting themselves in unacceptable danger.
“Statins are arguably the most widely studied medicines ever,” says Jeremy Sussman, a primary care provider at the University of Michigan and the Department of Veterans Affairs in Ann Arbor. “They are also among the most widely used. This makes any controversy an important one.”
Birth of a blockbuster
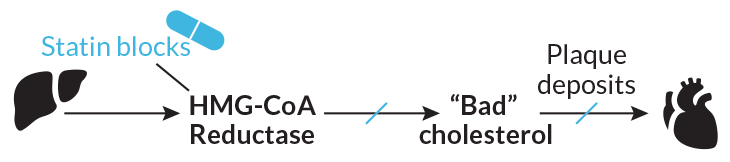
Like many tales of drug discovery, the statin story starts in a petri dish. During the mid-20th century, scientists worked out the chemical steps that cells, most commonly in the liver, use to convert acetyl CoA, a chemical formed during metabolism, into cholesterol. More than 30 different enzymes orchestrate the process, but one central to the assembly line is called 3-hydroxy-3-methylglutaryl-CoA (or HMG-CoA) reductase, an early step in a long line of steps.
In the late 1960s, Japanese microbiologist Akira Endo was inspired to search for an HMG-CoA blocker during a two-year stint in New York, where he was struck by the fatty excesses of the American diet. Returning to Japan, he happened upon a compound in a fermented broth of Penicillium citrinum, a rice mold taken from a shop in Kyoto, that blocked the action of HMG-CoA reductase. In 1978, scientists at Merck & Co. found another microbe-produced chemical that also disabled HMG-CoA reductase. The Japanese discovery fizzled in laboratory trials, but Merck’s compound eventually emerged as the first cholesterol-lowering drug, lovastatin (brand name Mevacor).
Story continues below graphic
Lovastatin targeted low-density lipoprotein, or LDL, cholesterol, often referred to as the “bad” cholesterol because it contributes to plaque buildup inside arteries. The drug didn’t lower another type of cholesterol, high-density lipoprotein, or HDL, which was thought to protect against heart disease because it scavenges cholesterol from arteries and ferries it to the liver for recycling. Today, HDL’s role is less clear (SN: 6/16/12, p. 14). Although statins demonstrated their ability to combat LDL cholesterol, proof that they saved lives was not established until a watershed study appeared in Lancet in 1994.
In that experiment, researchers from a collective of Scandinavian countries, and funded by Merck, followed more than 4,400 patients who had chest pain or had suffered a heart attack. After about five years, 8 percent of patients who took simvastatin (a synthetic version of lovastatin, marketed as Zocor) had died, compared with 12 percent who took a placebo, a 30 percent lower mortality rate. Doctors cheered. A blockbuster was born.
In the years following, a posse of other cholesterol fighters joined simvastatin to create what would become a $20 billion–plus annual market: pravastatin (Pravachol), fluvastatin (Lescol), atorvastatin (Lipitor), cerivastatin (Baycol), rosuvastatin (Crestor) and finally pitavastatin (Livalo). The drugs are now available as lower-priced generics, poised to further drive consumption. Together, statins have been subject to more than two dozen large clinical trials that have collectively included about 175,000 people with and without heart disease. And yet, some doctors worry that even this avalanche of data isn’t enough.
“The reality is there is more we don’t know than we do know,” says Wright. Among the conundrums he cites: The drugs vary widely in their ability to lower cholesterol, yet regardless of their potency, they appear to have the same potential to prevent a second heart attack or stroke. “Fluvastatin is the least potent,” he says. “Yet it appears to reduce cardiovascular events as much as rosuvastatin, which is the most potent. There’s something we’re not getting.”
Primary cares
To be clear, little if any disagreement exists over “secondary prevention,” or using the drug to prevent a second heart attack or stroke in someone with established disease. The contention arises over “primary prevention” — when an otherwise healthy person, whose main concern is simply elevated cholesterol, takes the drug to keep from taking that ambulance ride in the first place. This is a crucial context. If you have already survived one attack, you know you’re at increased risk for another. You’re willing to tolerate a certain level of side effects.
But healthy people, even healthy people whose cholesterol is too high, start with much lower odds of dying from cardiovascular disease than people already afflicted. It’s less certain whether they need the drug at all. A healthy person takes on the same risk of side effects as someone already struck by disease, but for potentially much less gain. That makes it vital to understand the true risk and benefit balance — and that’s precisely where the dispute lies.
The 500-pound gorilla of the statin research world is the Cholesterol Treatment Trialists’ Collaboration, commonly referred to as the CTT. Formed in 1994 and headquartered in the United Kingdom and Australia, the CTT consists of about 150 researchers who compile and interpret clinical trial data on statins. Their funding comes primarily from government sources and foundations. The individual trials the CTT evaluates were largely funded by the pharmaceutical industry.
Since in science no one study is a final answer, CTT gathers data from numerous clinical trials and feeds them into a meta-analysis — a calculation that combines data from different studies to come up with a wide-angle view. Scientists also obtain results by using systematic reviews, which compare the bottom line of different studies to determine where the true impact probably lies. Done well, these methods of blending data can provide a result with strong statistical power, finding an effect that might be missed in a single study.
But they are only as good as the studies that go into them. Depending on which studies are included (or excluded) and how they are analyzed, compilations can distort results or amplify biases and weaknesses in the research.
The CTT published its first meta-analysis of 14 clinical trials for secondary prevention in 2005, concluding that for every 39-point drop in LDL cholesterol (roughly equivalent to 1 millimole per liter of blood) among people who took a statin, the odds of a heart attack or stroke dropped by 21 percent, and mortality from coronary artery disease fell by 19 percent. More CTT-authored publications have appeared in the decade since, including analyses that extend the benefit to stroke prevention. Most recently, Collins and more than two dozen collaborators authored a 30-page review in Lancet last November, bolstered by more than 300 references. That analysis of published large randomized trials calculated that each 77-point drop in LDL cholesterol (a 2 millimole per liter drop) reduced the risk of a major cardiovascular event — heart attack, stroke or the need for a coronary-clearing procedure — by 45 percent. Those kinds of LDL drops are realistic, at least in the short term. A 2015 review of studies of the widely prescribed drug atorvastatin found LDL reductions averaging 64 to 90 points in studies of three to 12 weeks, depending on the dose of drug used.
The degree of benefit depends on whether you’ve already had a heart attack or stroke. The CTT researchers calculated the number of patients who need to be treated to benefit one person. They estimated that if 10,000 people with heart disease lowered their LDL cholesterol by 77 points, 1,000 of them would be spared a second major event over the next five years. If 10,000 seemingly healthy people lowered their LDL by the same amount, an estimated 500 of them would be spared.
Insurance policy
What about those 9,500 healthy people who gained nothing from taking the drug those five years? The reality is, there is no way to sort them out ahead of time. Collins likens it to buying insurance. Everyone pays with the understanding that no one knows who is going to have an accident. If it’s your car, though, that policy can be a lifesaver.
“In insurance, you don’t know which people are benefiting,” he says, you just know that some people will. “The important thing is, there are heart attacks and strokes that are being prevented.” Also, he says, data suggest that the benefits continue to accumulate. If 500 people are spared a heart attack or stroke over five years, “over 10 years the number would double,” Collins says.
So the bottom line, according to the CTT estimates, is that for 5 percent of healthy people taking a statin, the drug means the difference between life and death, health or disability. And in return, the other 95 percent aren’t putting themselves at much risk for dangerous side effects.
Wright, of the University of British Columbia, remains unconvinced. He thinks that the numbers in the Lancet review go far beyond what the data show. The CTT numbers, he says, are based on extrapolations of cholesterol reductions greater than those achieved in reality. In a response to the Lancet review published in March, he and colleagues noted that the average cholesterol reductions actually achieved among lower risk groups in the trials were far below the 77 points that formed the basis for the conclusions.
Wright’s research group has performed its own analysis of primary prevention, published in 2010. In that calculation, the number of people who would avoid a cardiovascular event is not 5 percent, as the review in Lancet estimated, but somewhere between 1 and 2 percent — which means only 100 or at most 200 of every 10,000 healthy people taking a statin would benefit.
Even considering the seriousness of nonfatal heart disease, the ultimate test is not whether statins keep a person from an angioplasty or even heart attack, but whether the drugs save lives. Studies of primary prevention, because they start with healthy populations, have a much higher hurdle to show a reduction in mortality. Over the typical length of a major clinical trial, the overall risk of death is low to begin with.
Still, Collins points to evidence that lives are saved. In 2012 in Lancet, a CTT meta-analysis of 27 randomized trials found that even among people with no previous vascular disease, those who had a 39-point decrease in LDL had a 9 percent lower overall mortality risk over about five years.
But there’s another way to look at those data: a straight-up comparison of low-risk volunteers who take the drug with those taking a placebo. Following the Lancet publication in 2012, Wright and colleagues recalculated the numbers and did not find a mortality benefit among people who had less than a 20 percent chance of having a heart attack in the next five years, based on established prediction measures.
After that analysis appeared in BMJ in 2013, Collins demanded a retraction, but two independent statistical reviews concluded that the paper did not meet any criteria for withdrawal.
Downsides debated
Mortality is not even the most contentious issue in the statin wars. That prize goes to the question of harm: How much might healthy people — the ones who weren’t going to have a heart attack or stroke anyway — be hurt by the drug. To Collins and other CTT leaders, side effects, especially serious ones, are rare and clear up when people stop taking the drug. To others, the story is not that simple.
Critics talk mostly about effects on muscles, particularly pain and weakness. One early statin called Baycol was withdrawn from the market in 2001 after it was linked to 52 deaths from a breakdown of muscle tissue. Studies following the scandal suggested that statins might impede protection from oxidative stress or alter other chemical reactions in muscle cells.
It’s important to note that randomized studies haven’t found side effects even remotely as prevalent as critics contend. Back to that theoretical population of 10,000 in the November Lancet review, only five people would experience muscle problems, and just one would have a serious breakdown of muscle tissue.
And even those small numbers might overestimate what occurs in everyday life, says Richard Hobbs, head of the department of primary care health sciences at the University of Oxford, who defended statins last year in BMC Medicine. He points out that clinical trial volunteers are regularly quizzed about possible side effects — and says that asking the question may plant the suggestion in their minds. “The trials, because they are searching for adverse effects, may overstate them,” he says.
The reason for the stark difference in opinion over side effects comes down to how much weight is given to patients who were not included, or not counted, in meta-analyses, says Rita Redberg, a cardiologist at the University of California, San Francisco and a prominent voice of concern over statins. In some trials, she says, people who complained of side effects beforehand were not allowed to participate, dropped out before the studies were completed or were not counted because the criteria for being put in the side effects category were so narrowly defined.
To qualify as having muscle weakness in the CTT studies, a person had to not only feel muscle aches, but also have elevated levels of a certain enzyme (a criterion Collins says is necessary to show the drug caused the effect). Redberg also worries that there are still problems that might be undetected because no one is looking for them, diabetes being a case in point. A link between diabetes and statins wasn’t discovered until a 2008 analysis of almost 18,000 people published in the New England Journal of Medicine, which found that 216 people taking a placebo developed type 2 diabetes while 270 taking a statin did.
Redberg says observational data — which follow real-world patients on statin therapy — report side effect risks much higher than those in the CTT analyses. In one routine-care study, reported in 2013 in Annals of Internal Medicine, 8 percent of patients stopped taking statins because of side effects. One study from an international team of researchers, published in JAMA in 2016, found that among people who previously complained of problems with taking statins, 43 percent developed muscle pain after taking the drug in the study, atorvastatin, compared with 27 percent who took a dummy pill.
“I can tell you side effects are quite common,” Redberg says. “Among my patients, the most common are muscle problems, also malaise, fatigue, feeling in a fog.”
Redberg and others have also criticized the CTT for not releasing the raw data of clinical trials, which would allow other independent researchers to mine the data for adverse reactions. When asked about this, Collins counters: “It’s not our data.” The results that have informed CTT calculations were provided with the understanding that the numbers belonged to the original investigators. And, he says, the CTT doesn’t have data on side effects beyond what has been reported.
In the end, the potential risk that any patient is willing to take may hinge on how much danger they are in to start with. Guidelines released in 2013 by the American Heart Association and the American College of Cardiology say that people between the ages of 40 and 75 should take a statin if their risk of cardiovascular disease is 7.5 percent or higher over the next 10 years. In the United States, that makes an estimated 78 million adults eligible for statin prescriptions. European guidelines set a higher threshold: between 10 and 20 percent risk over the next 10 years. The U.S. Preventive Services Task Force updated its recommendations in November, saying adults should consider statins if they have one or more major risk factors for heart disease.
Sussman, of Michigan, refers to one of several online calculators that can help determine what that risk number is for any particular person. These kinds of tools take into account each person’s unique set of circumstances. In one online tool, a sedentary 60-year-old white male with a weight of 250 pounds, a total cholesterol of 225, no high blood pressure and no personal or family history of heart disease might have a 9 percent risk of having a heart attack in the next 10 years. A 60-year-old African-American woman with diabetes but all other parameters the same would have a 13 percent risk.
The guiding principle Sussman tells his patients is that the lower your risk of disease in the first place, the less you have to gain from statins. Patients also have to factor in their own sense of how much they fear a heart attack or stroke — all the while knowing there are other means of prevention with almost no risk that can get lost in the statin debate, including weight loss, exercise and a better diet. That theoretical 60-year-old man with a 9 percent risk could drop his risk to about 5 percent with 20 minutes of moderate activity each day and better eating habits.
“You say to a patient, ‘Here’s a pill, and the odds of benefit are small, but you’ll have to take it the rest of your life,’” says Sussman. Over the coming decades, the drug may cause you problems you never would have had. But one of the people who hits the jackpot — and dodges a devastating heart attack or stroke — might be you. “That’s a hard choice.”
This article appears in the May 13, 2017, issue of Science News with the headline, “The Statin Umbrella: Yes, the drugs protect hearts. But critics are questioning their expanding use.”