Five reasons to not totally panic about ticks and Lyme disease

BITE ME This summer, a lone star tick bit the author’s baby. The culprit, shown, was a nymph that wasn’t carrying disease-causing bacteria and had only a bit of blood in its belly, according to the lab that tested it.
Courtesy of Meghan Rosen
I thought it was just a scab.
The brown speck clinging to my baby’s cheek had been there for a day or so, resting on a reddish patch of skin. He must have scratched himself, I thought, as I picked lightly at the mark.
My husband was the first to figure out the truth. That little round speck wasn’t a scab at all — it was a tick.
I had recently read a scary article about ticks (complete with scary title: “Be Very Afraid of Ticks”), and I was terrified. We plucked the bug off the baby, stored it in a plastic baggie and popped it into the freezer. But what next? Head to the ER? Get a blood test for Lyme disease? Start him on antibiotics in case he was infected?
None of the above, says pediatric infectious disease specialist Sunil Sood, of Hofstra North Shore-LIJ School of Medicine in Hempstead, N.Y. “It’s all overkill,” he says. A lot of parents panic when they spot a tick on their child because they think first of Lyme disease, a bacterial illness that can hit people with headaches, fevers, arthritis and even paralysis of the face.
After hearing Sood talk about ticks on The Diane Rehm Show, I talked with him and with infectious disease physician Paul Mead about what parents need to know.
1. Not all ticks carry Lyme disease.
A nasty little spiral-shaped bacteria called Borrelia burgdorferi causes Lyme disease. It hitches a ride in the guts of some, but not all, tick species. After an infected tick sinks its mouth parts into a person’s skin and begins to feed, the bacteria mosey up from the gut to the tick’s salivary glands and into the person.
Blacklegged ticks, or deer ticks, are the main carriers of Borrelia bacteria. So if your child has a brown dog tick, a Rocky Mountain wood tick, or a lone star tick (Baby S’s buddy), you don’t have to worry about Lyme disease. But these other types of ticks can carry different kinds of disease-causing bacteria, so it’s good to know which tick you’re dealing with, Sood says.
“Parents should always remember to save the tick,” he says. “That’s the most important thing.”
To figure out which kind of tick bit you or your loved one, you can look at pictures on the CDC’s website, or send the tick to an insect identification lab. (We snapped an iPhone pic of Baby S’s tick and e-mailed it to the USDA, which identifies ticks for free.)
2. There’s no need to get the tick tested for diseases.
Several labs offer tick-testing services. These facilities will grind the tick up and look for DNA from Borrelia or other disease-causing bacteria. Testing sounded logical to me, so I shelled out 50 bucks to a zoology lab* in Massachusetts and sent off Baby S’s tick. I was hugely relieved when the test results came back negative. That meant Baby S was safe, right? Not necessarily.
“Testing for bacteria is a waste of time and money,” Sood says. Blood in the tick’s belly can interfere with the test results, so the tick could test negative even if it’s carrying harmful bacteria. A positive test isn’t all that telling either. A tick that’s positive for Borrelia hasn’t necessarily passed the bacteria on to the bitten child.
What’s more, if the lab destroys the tick without identifying it first, doctors won’t know which disease symptoms to look for, Sood says. “I don’t want to be looking for Lyme disease when it was a lone star tick,” he says.
(*See note below for an update on this point.)
But nearly 90 percent of kids with Lyme disease do develop a rash at the bite site. The rash is a roughly circular red splotch that gradually grows bigger over time. In some kids, more than one splotch shows up. It can take a month to appear, so parents should stay watchful. For kids who don’t get a rash, look for fever and other flulike symptoms in the warm months, from April to November, Sood says.
Since we knew that a lone star tick bit Baby S, we watched for symptoms of ehrlichiosis and Rocky Mountain spotted fever, both potentially fatal diseases. (They can be hard to spot in infants, so if he had become feverish, knowing the type of tick that bit him would have been helpful information for his pediatrician.)
4. Lyme disease is generally easy to treat.
The odds of getting Lyme disease from an individual deer tick bite are pretty low: Even in tick-ridden areas, less than 5 percent of bites result in an infection. But those that do are easy to deal with, Sood says. “Lyme disease is completely treatable. All the symptoms literally melt away with antibiotics.”
“I’m actually more worried about mosquito bites than tick bites,” he says.
Catching the problem early can make treatment easier, says Paul Mead, an infectious disease physician at the Centers for Disease Control in Fort Collins, Colo. But, he says, “the vast majority of patients who have Lyme disease will recover and do just fine.”
Still, about 4 to 5 percent of people who get treated have symptoms, such as fatigue, muscle aches and trouble sleeping, that linger for more than six months. The condition, named post-treatment Lyme disease syndrome, or PTLDS, is commonly known as “chronic Lyme disease,” and on the Internet, it’s a notoriously thorny subject.
“There’s a lot of misinformation out there,” Mead says. No one really knows what causes the symptoms. People could be having a delayed immune response, or they may have an undiagnosed illness that’s to blame. But scientists do know that lengthy courses of antibiotics don’t seem to help.
“People should be skeptical if providers are telling them that they need to be on months and years of antibiotics,” Mead says. Very few — if any — people actually die from Lyme disease. One 2012 study found that from 1999 to 2003, only 23 death certificates listed Lyme disease as the underlying cause (and perhaps only one of those people actually had the disease). During the same time period, the CDC recorded more than 96,000 cases of the disease.
But not every case gets reported, Mead says. The CDC estimates that the number of Americans diagnosed with Lyme disease each year is actually around 300,000.
5. There are a few good ways to prevent tick bites.
First, if kids play outside, check them daily for ticks, making sure to inspect easy-to-miss nooks and crannies like the armpits, groin and scalp. Bathing with a washcloth is a simple and effective way to sweep ticks from the skin before they’ve latched on.
Bug repellents like DEET and permethrin can help keep ticks away. For kids, the American Academy of Pediatrics recommends formulations with 10 to 30 percent DEET (although Canada’s public health department thinks kids should stick to formulations with 10 percent DEET or less).
If you do find a tick that’s attached, remove it right away. A pair of thin-tipped tweezers and an empty container will do the trick, Sood says. “It’s nothing fancy,” he says. Grasp the tick at the mouth end, and pull straight up. “Gentle, steady pressure, and it will generally pop right out,” Sood says.
I’m much less panicked about ticks now than I was when one was hanging off Baby S’s face. But I do worry that I might not notice one hiding out in some cozy crevice of his skin. And the problem isn’t likely to go away: The number of Lyme cases might go up as the climate changes and ticks have more warm, woodsy places to live.
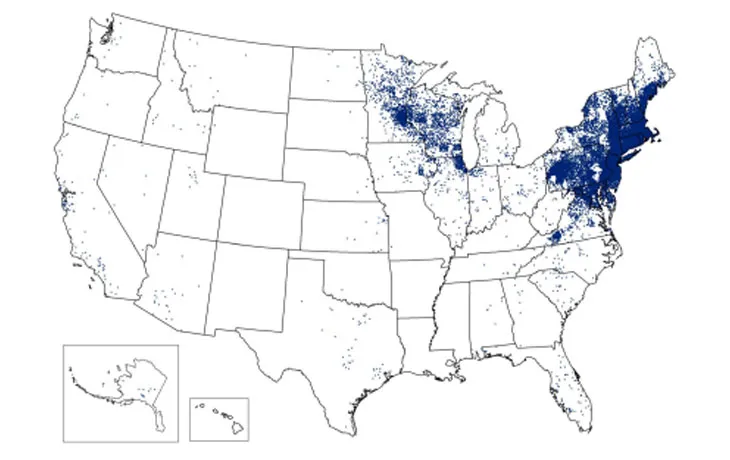
I know our family needs to be especially vigilant: We live in an area that keeps erupting with new cases. Montgomery County, Maryland, ranked 27th out of more than 3,000 U.S. counties in the number of Lyme disease cases tallied up from 2007 to 2011. It’s number one in Maryland. (You can check out the map in this paper to see if you live in a high-risk area, look at this CDC Excel spreadsheet to see how your county fares, or read more about the CDC’s maps here.)
Still, I’m trying to ratchet down my fear level from super-freak-out-panic to something in the neighborhood of responsibly concerned.
“I don’t think being alarmed is helpful,” Mead says. “People should be aware of the problem, and know what to do protect themselves.”
I’m not ready to douse my family’s clothing in bug repellent just yet, but I have vowed to do daily tick checks and wash well after playing outdoors. And next time, if I see a funny-looking scab on my kids’ skin, I’m checking to see if it has legs.
*Update, 4 p.m., August 21, 2015:
Microbiologist Stephen Rich of the Laboratory of Medical Zoology (the lab that tested Baby S’s tick) at the University of Massachusetts took issue with Sunil Sood’s statement that “Testing for bacteria is a waste of time and money.”
Rich explained that the lab tests are not intended to diagnose human disease. Instead, he notes, one of the big benefits is disease surveillance. In addition to identifying deer ticks, dog ticks, lone star ticks and the diseases they may carry, TickReport makes data available to the public.
He makes a good point. Baby S’s tick was one of 272 ticks the lab has tested from Maryland — five of which came from my zip code alone (none of the five tested positive for the bacteria that causes Lyme disease). So people can use the data to glean info about potential risk in their area.
Sood’s point was that testing a tick for bacteria is not a good way to find out if a bitten child was infected. But I agree that there’s certainly value to the information collected from testing ticks and tracking tick bites.







