Alcohol on your breath need not be all bad
Police today can check whether people have been drinking by smelling their breath. In the future, a person might have a good excuse for giving off the aroma of alcohol–a doctor’s prescription.
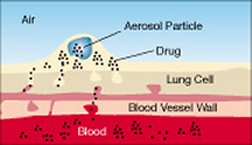
Buoyed by a study in rats, Massachusetts scientists suggest that people with diabetes or other chronic diseases may someday forgo frequent injections of medicine such as insulin and instead inhale a drug-carrying alcohol mist.
“It’s a new concept that merits exploration,” says John Patton of Inhale Therapeutic Systems in San Carlos, Calif.
Since most people hate injections, pharmaceutical firms strive to develop medicines that can be taken as pills. Yet insulin, which controls people’s blood sugar, and many other drugs are large proteins that break apart during a trip through the digestive system.
Alternative forms of drug delivery, such as nasal sprays and skin patches, often don’t get enough medicine into the blood. In contrast, the lungs offer ready access to the bloodstream because they routinely pour oxygen into it.
“The opportunity of delivering drugs through the lungs is just huge,” says Anthony J. Hickey of the University of North Carolina at Chapel Hill.
Most researchers have focused on transforming dry powders or water-based drug solutions into aerosol particles small enough to penetrate deeply into the lungs. Yet each of these drug formulations has several limitations.
Powders tend to clump and require specially designed inhalation devices, for example. “Historically, it’s been difficult to disperse them efficiently and reproducibly,” says Hickey.
On the other hand, water solutions are open to microbial contamination and contain far smaller concentrations of a drug than powders do. Also, proteins may degrade in water over time.
Proteins suspended in ethanol, the form of alcohol in beer and wine, may offer a third option for inhalation therapy, Alexander M. Klibanov of the Massachusetts Institute of Technology and his colleagues report in the Sept. 25 Proceedings of the National Academy of Sciences.
“Ethanol has some advantages,” notes Klibanov. First, the chemical has sterilizing properties that should prevent microbial contamination of an inhalation device. Second, proteins generally remain stable in ethanol.
To test their concept, the investigators added insulin to ethanol and showed that rodents inhaling a mist of the mixture experienced a drop in blood sugar concentration. The rats responded as well as rodents inhaling aerosols from a powder or a water solution did.
A series of tests indicated that the alcohol aerosol hadn’t damaged the rodents’ lungs, says Klibanov, but the long-term safety of alcohol-inhalation therapy needs further study. The strategy wouldn’t deliver enough ethanol to intoxicate anyone, he says.
Neither Klibanov nor the other researchers expect ethanol suspensions to completely replace powders or water solutions in inhalation therapy, but they say it may offer the best option for some drugs.
“Anything that’s new and different can only help the field,” says Hickey.







