Catching a Cancer
Viral culprits may explain a host of tumors with as-yet unknown triggers
Mentors at the Rockefeller Institute had warned Peyton Rous not to waste his career fooling with “the cancer question.” Then he got the bright idea that tumors might be contagious. Rous extracted part of a sarcoma from a hen, strained out the cells and injected the remnants into another bird. The second hen also developed cancer. Something hidden inside the tumor must be causing the cancer. His culprit: a virus.

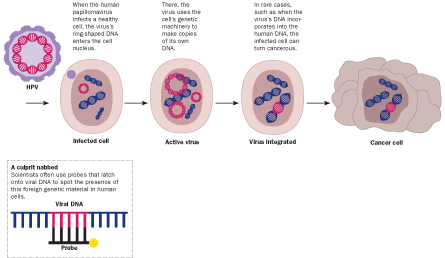
Rous’ finding was met with such resounding disbelief that he soon abandoned the entire line of research. He returned to it 20 years later, still on the unpopular side of scientific opinion. More years passed, until Rous was finally vindicated with a Nobel Prize “for his discovery of tumor-inducing viruses” — 56 years after he began his work, in 1910.
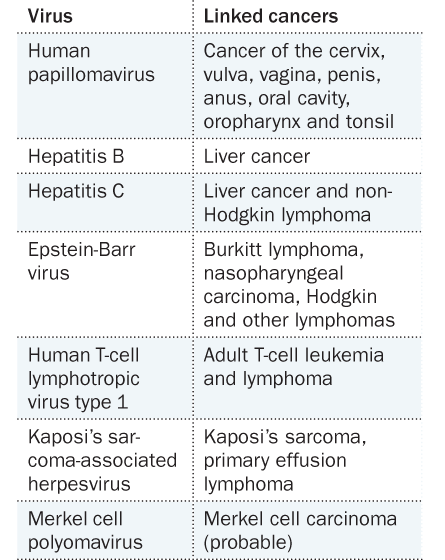
Viruses exist at the border between living and nonliving, working their way into tissues and piggybacking on a cell’s machinery to make copies of themselves. In the century since Rous’ chicken studies, researchers have uncovered about half a dozen viruses that, while going about their sole mission of replicating, happen to trigger cancer. Some cancer viruses bear familiar names like HPV, known to cause cervical cancer, and hepatitis B and C, which lead to tumors in the liver. Others aren’t so famous, including Epstein-Barr virus as a cause of non-Hodgkin lymphoma and two viruses known to cause tumors in people with severely repressed immune systems. Yet scores of researchers are intrigued by the possibility of cancer viruses that haven’t yet been discovered.
As of now, the official figure for the percentage of human cancers caused by viruses is around 20 percent — but most experts concede that number is largely an educated guess, accounting for known viruses behaving in predictable ways. “Thirty years ago, that number would have been 5 percent,” says Robert Garry, a virologist at Tulane University School of Medicine in New Orleans. “It’s a moving target. How high is it going to go? We don’t know.”
Soon, they may. Until recently, virus hunting involved painstaking detective work. But improvements in molecular technologies have made it easier to search for and study the behavior of snippets of nonhuman genes woven around otherwise normal threads of genetic material. In just the last eight years, a human pathogen discovery project housed at Washington University in St. Louis has found 40 new viruses. “We are huge walking bags of viruses,” says Eain Murphy, a virologist at the Cleveland Clinic. “There are so many we don’t even know what they do.”
Not all will have a cancer connection. Yet considering the scope of cancer triggers that remain undiscovered — even in breast cancer, most women have no known risk factors aside from their age and sex — many researchers expect previously unknown viruses will be to blame for some cancers, or at least make otherwise sluggish tumors more aggressive.
Medical science has already compiled a long list of little-noticed viruses suspected of contributing to common malignancies, including cancers of the colon, skin, lungs, breast and brain. Recently, some types of skin cancer, and possibly other malignancies, have been linked to a powerful group of viruses called polyomaviruses, which are little more than free-range cancer genes.
New investigations also stand to finally settle old controversies — such as whether a virus can cause breast cancer — and ignite fresh ones. Already, some scientists are speculating whether lung cancer in nonsmokers may have some viral origin, either through human viruses or infections from animals. “The next decade promises to be an exciting era for the tumor virology field,” researchers wrote last year in Cancer Letters.
Yet with better virus detection also comes a concern. If people are indeed walking bags of viruses, then every slice of tissue could hold countless false leads. As a case in point, researchers almost universally mention XMRV, a virus discovered in 2006 as a possible cause of prostate cancer. Six years and dozens of studies later, the general conclusion is that XMRV wasn’t inciting human tumor cells, but was instead a case of laboratory contamination with a rodent virus.
“You have to keep in mind the criteria for causality,” says Dana Rollison, a cancer epidemiologist at the Moffitt Cancer Center in Tampa. Finding a virus inside a tumor opens questions that may take years to answer.
From rumor to tumor
Scientists have been interested in polyomaviruses since 1971, when they were found to infect humans. But the landmark report linking a polyomavirus to skin cancer was not published until 2008. In that study, appearing in Science, researchers from the University of Pittsburgh Cancer Institute found that 80 percent of tumors from Merkel cell carcinoma, a rare but deadly form of skin cancer, contained a polyomavirus now named Merkel cell polyomavirus, or MCV for short. In May, those researchers and others reported in Science Translational Medicine that an experimental drug targeting the virus appeared to stop the cancer from growing.
“Of all the viruses that might have a plausible link to cancer, none have a more deadly gene than polyomaviruses,” says Richard Boland of the Baylor Research Institute in Dallas. Healthy tissues can start down the path to cancer if a gene producing something called T antigen turns on, taking mechanisms that naturally suppress cancer growth offline. The “T” stands for transforming. A polyomavirus “is essentially the T antigen gene with a bunch of packing and assembly material,” Boland says.
MCV may even have a role in squamous cell carcinoma, the second most common form of skin cancer in the United States. Squamous cell carcinoma arises from cells making up the upper layers of the skin, and while not as dangerous as melanoma because it is less likely to spread, it can be deadly in some cases.
It’s known that ultraviolet light is a risk factor for skin cancer, but that doesn’t explain why so many people exposed to sunlight don’t get cancer, or why the cancers can sometimes appear on skin that rarely sees the light of day. In recent studies, Rollison has found MCV in 38 percent of squamous cell tumors.
Patients with squamous cell carcinoma who were infected with the Merkel cell virus were about twice as likely to have antibodies for MCV as were people who didn’t have cancer, Rollison and colleagues reported in January in Cancer Epidemiology, Biomarkers & Prevention. That’s a sign that the bodies of the cancer patients had been fighting an active infection. One of the criteria for linking a virus to cancer is that at some point in the life of the cell, the virus has to be actively replicating itself, creating an infection that would prompt the immune system to react.
The support for MCV’s role in squamous cell tumors “is compelling, but it’s not definitive,” says Rollison. “The piece that is really missing is prospective data, showing that the virus was there before the cancer.”
Polyomaviruses are emerging as a possible risk factor in other cancers, not just those of the skin. Boland is investigating whether a polyomavirus called John Cunningham virus, or JCV, might trigger some colon and anal cancers. JCV is common, perhaps infecting as much as 90 percent of the adult population — a factor that can complicate virus-cancer investigations.
Because the virus needs coconspirators, like genetics, environmental conditions and tissue that is hospitable to infection, only a fraction of people who develop an active infection would get cancer. (That’s also the case with other viruses: In June, Rollison and her colleagues reported in the Journal of Infectious Diseases that a practically ubiquitous virus of the skin might work synergistically with sunlight to promote nonmelanoma skin cancers.)
Estimates of how often JCV occurs in colon cancers vary considerably, from studies that find the virus in almost all colon tumors to those unable to find so much as a trace. As for anal cancer, last year Boland and colleagues published a study in Cancer suggesting that JCV is more common in anal cancers than is HPV, the cervical cancer virus, which is considered a risk factor. The analysis of 21 anal tumors found JCV in all of them, including nine that were clear of HPV.
Boland acknowledges that skepticism about JCV remains high, largely because only small numbers of virus particles appear to exist in full-blown tumors. This scarcity could be because the virus doesn’t prompt the polyps to grow. In a hit-and-run kind of approach, it may only knock normal tissue into the early steps of cancer. If JCV is necessary only to make healthy tissue blossom into a polyp, the virus could be long gone by the time the cancer shows itself.
JCV could also be aiding and abetting the tumor process farther down the line, not just at the beginning. Boland and colleagues published experiments in 2009 in PLoS ONE suggesting that infection with JCV increases the likelihood that tumors will spread. Work remains to show that patients with colon cancer have antibodies to the virus, and Boland acknowledges that he could be proved wrong. “I made a decision very early on not to get breathless about this,” he says.
Of mice and women
Among other researchers with sober expectations are those who have engaged in a controversial, decades-long pursuit of a breast cancer virus. Seven laboratories have found evidence supporting the idea that a virus could trigger human breast cancer, according to a 2009 report in the Journal of the National Cancer Institute.
A mouse version of a breast cancer virus was discovered in the 1930s, and since then the idea of a human counterpart has gone in and out of scientific favor. The mouse version, known as mouse mammary tumor virus, or MMTV, is passed from mother to offspring through breast milk.
Some of the most intriguing hints of an infectious cause in humans come from how the basic geography of the disease syncs with prevalence of MMTV. A woman’s odds of getting breast cancer greatly depend on where she lives. Worldwide, the odds of getting cancer vary, with African and Asian women having a fraction of the risk that European and North American women do. Plus, a woman who moves from a region with a low incidence of breast cancer to a higher one appears to acquire the risk level of her new home.
“In Europe and North America, the mice have a lot of mouse mammary tumor virus. In Asia, where they have the Asian house mice, it’s very, very difficult to find it,” says Garry of Tulane. Women in North America have a risk of breast cancer up to three times as high as women in Asia. The question is whether the mouse version has been able to remodel itself for human tissue.
Garry believes it might have. From laboratory samples at Tulane, he found evidence of a separate human mammary tumor virus. But when Hurricane Katrina struck in 2005, the laboratory’s breast tumor samples were lost, leaving him unable to conduct further studies. “I’m open-minded,” he says. “Some of our studies pointed to the fact that there was a virus there.”
Later work has also been supportive. In 2007, a research team writing in the journal Retrovirology used updated genetic techniques to show, for the first time, evidence that MMTV could replicate inside human cells.
Many other scientists remain unconvinced that MMTV can adapt to people. “In my lab, we’ve not been able to infect human cells with the virus,” says Susan Ross, a microbiologist at Perelman School of Medicine at the University of Pennsylvania in Philadelphia.
To show that a version of MMTV causes human cancer, she says, scientists must consistently demonstrate that the virus is able to enter human cells and use them as a personal Xerox machine. A woman’s immune system must also show signs of fighting an active infection. Earlier studies have suggested such signs. But in 2006, Ross and colleagues from the National Cancer Institute reported in the British Journal of Cancer that, using more modern tests than in previous work, they were unable to detect antibodies to MMTV in a sample of women with breast cancer.
Up in the air
In addition to MMTV, other animal viruses can cause cancer, which makes them objects of scientific curiosity. In February, in Zoonoses and Public Health, epidemiologists from the University of Arkansas for Medical Sciences in Little Rock reviewed 60 studies of lung cancer risk among workers in the meat and poultry industry. That review found a 30 percent increased risk of lung cancer even after taking smoking into account. The researchers called for more careful study “so that the possible role of food animal oncogenic viruses in the occurrence of human lung cancer can be clearly defined.”
There are already candidates. A virus called Jaagsiekte sheep retrovirus infects sheep and goats, and is the only known virus to cause lung cancer in any animal. Among those with a newfound interest in Jaagsiekte is virologist Robert Gallo from the University of Maryland’s Institute of Human Virology, who was drawn to lung cancer after “too many friends died from cancer and they weren’t smokers,” he says.
While the vast majority of people with lung cancer have used tobacco, about 13 percent of cases occur in people who have never smoked. Cancer experts cite radon, secondhand smoke or other pollutants as possible causes, but the culprits have not been identified definitively. In addition to Jaagsiekte retrovirus, there’s a possible association between lung cancer and HPV, researchers from the International Agency for Research on Cancer reported last April at a meeting of the American Association for Cancer Research.
For now, a lung cancer virus is little more than an idea among lots of ideas. But as someone who has been trying to uncover cancer-causing viruses for more than four decades, Gallo notes that locating viral genetic material in “human” DNA has never been easier, and new efforts stand to speed up the pace of tumor virology research.
In some ways, though, the field has never been more problematic, Gallo says. He, too, brings up the case of XMRV and prostate cancer, first found when researchers searched for viral culprits in the genetic instruction book of prostate cancer tissue.
It is great to have the power of genetic tools, Gallo says. “But you also have to have the power of thinking. What does it mean?” he says. “So you found a virus. It’s the beginning of the beginning of a possibility.”
Still, it is from possibility that discovery begins. As the late author Ray Bradbury once said, the best scientists start with the idea that anything is possible.







