Can humans get chronic wasting disease from deer?
Results from brain organoids suggest it is hard for deer prions to infect human brains

A doe and her young fawn cross a road in Rocky Mountain National Park in May 2022. Chronic wasting disease has spread widely across the United States since it was first discovered in the park’s elk herd in 1981.
Ray Wise/Getty Images
Chronic wasting disease has been spreading among deer in the United States, which has raised concerns that the fatal neurological illness might make the leap to people. But a recent study suggests that the disease has a tough path to take to get into humans.
The culprit behind chronic wasting disease, or CWD, isn’t a virus or bacterium but a misfolded brain protein called a prion. A new study using miniature, lab-grown organs called organoids supports previous work, showing that CWD prions don’t infect human brain tissue.
Brain organoids exposed to high doses of prions from white-tailed deer, mule deer and elk remained infection-free for the duration of the study, or 180 days, researchers report in the June 2024 Emerging Infectious Diseases. However, organoids exposed to human prions that cause a related condition, Creutzfeldt-Jakob disease, quickly became infected. The finding suggests that a substantial species barrier prevents CWD from making the jump from deer to humans.
“This was a model that could really help tell us … whether or not it was a real risk,” says Bradley Groveman, a biologist at the National Institutes of Health’s Rocky Mountain Laboratories in Hamilton, Mont.
But brain organoids aren’t a perfect mimic of the real thing and may lack features that would make them susceptible to infection. And new prion strains can appear, perhaps including some that might help deer prions lock onto healthy brain proteins in humans.
To keep an eye on the risk to people, researchers need to keep amassing evidence and testing new prion strains on organoids or in other experiments, says Cathryn Haigh, a cell biologist also at Rocky Mountain Laboratories. “I don’t think we’ll ever be able to turn around and say [human infection] is impossible.”
A spreading disease
Deer with CWD are doomed. There is no cure.
The prions responsible for the disease — which affects deer, elk, moose and other cervids — spur a healthy brain protein called PrP to twist into an abnormal shape. These warped proteins clump together, killing brain cells and causing symptoms such as listlessness, stumbling, lack of fear of people and drastic weight loss. Animals typically start showing symptoms around 18 to 24 months after getting infected.
Concern about the danger that deer, elk and moose prions pose to people has been rising, in part because of the disease’s persistent spread across North America. On April 5, CWD was reported for the first time in Indiana, and on May 6 officials in California announced the state’s first cases in two wild deer. To date, the disease has been identified in wildlife in 34 U.S. states as well as parts of Canada, South Korea and northern Europe — a considerable increase since the first known case appeared in 1967 in a captive deer from Colorado.
What’s more, a higher proportion of deer are infected with the disease, says Debbie McKenzie, a prion biologist at the University of Alberta in Edmonton, Canada. “For a long time … 1 in 100, 1 in 1,000 deer would be infected…. But we’re now at a time where there’s deer populations where CWD prevalence is greater than 75 percent.”
A spreading disease
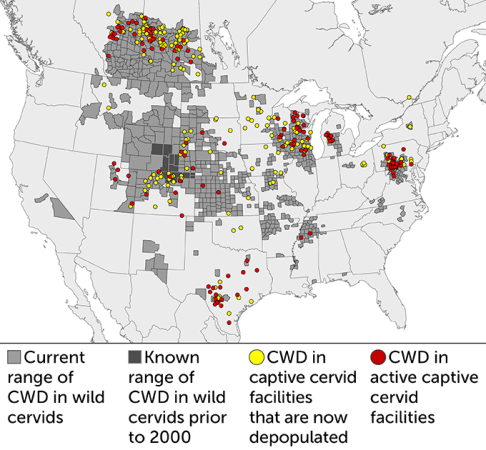
Since chronic wasting disease was first discovered in Colorado in 1967, the disease has spread widely across North America. Prior to 2000, just Colorado and Wyoming had known cases in wild deer and elk (dark gray). Today, the disease is found in 32 other states and 4 Canadian provinces (light gray). Captive animals are also infected; some facilities have current outbreaks (red circles) and others have culled infected populations (yellow circles).
Distribution of chronic wasting disease in North America
If some hunters aren’t testing animals, that increases the chances infected deer meat will make it to someone’s plate. (In the United States, requirements and recommendations for hunters vary by state.) And proteins aren’t affected by cooking the way bacteria or viruses are, so even cooked meat could pose a risk.
Lessons from previous cases
An outbreak of mad cow disease — another prion malady — after people consumed meat from infected cattle in the 1980s and 1990s helped put a spotlight on chronic wasting disease, Haigh says. While the deer disease was discovered before mad cow, back then people largely weren’t worried about the risk to humans.
But the realization that a bovine prion could infect people and cause disease “put into the consciousness that this is a possibility,” Haigh says. “And now we have another disease in an animal that we eat.”
Past research has suggested that prions may have a hard time jumping between certain species (SN: 4/4/14). Work done in mice tweaked to carry the human version of PrP has shown that transmission to people may be a possibility, though less transmissible than prions from cattle. Studies in macaques, a common animal stand-in for people, however hint that deer-to-human transmission of chronic wasting disease is unlikely.
Yet the prospect of transmission of faulty prions from wildlife to humans remains a big question, Groveman says, particularly because venison is on the menu in North America. Vigilance, experts say, is key to catching any potential transmission early, though there have been some jump scares.
News reports in April put the spotlight on a case report presented at the annual American Academy of Neurology meeting in Denver that described a fatal neurological disease in two hunters. The individuals had a history of consuming deer meat from a population known to have chronic wasting disease. But both likely died of a different prion ailment, Creutzfeldt-Jakob disease, which can arise sporadically, according to both the report and the U.S. Centers for Disease Control and Prevention.
“To date, there have been no reported cases of CWD infection in people,” says epidemiologist Ryan Maddox of the CDC in Atlanta.
Barriers to infection
While the mad cow prion sickened hundreds of people starting in 1994 — it can take a decade or more for people to show symptoms — the barrier for its transmission into people is also incredibly high, McKenzie says. Although millions of people are estimated to have been exposed to infected cattle during the outbreak in the 80s and 90s, as of 2022 there have been just 178 cases of Creutzfeldt-Jakob disease caused by infected meat in the United Kingdom, the outbreak’s epicenter, and 55 in the rest of the world.
But the factors that perhaps made some people more susceptible to infection remain unclear. It’s possible that infected individuals were exposed to an incredibly high dose, or the PrP protein in their brains had just the right shape to interact with cattle prions, McKenzie says. “There must have also been other things that contributed to the fact that they were susceptible.”
Prion strains, which twist PrP proteins in different ways, can also come into play. How prions misfold is one factor that can prevent the proteins from infecting a new species, Groveman says. Figuring out the differences in how deer prions bend and curl could help expose which might attach to PrP from people or other animals.
But scientists have a harder time revealing what prions look like compared with normal PrP. That lack of knowledge makes it harder to explore the potential for prion diseases to make the jump from one species to another.
There are at least five prion strains that cause chronic wasting disease, for instance, each of which infects a different range of cervid species. “And we really don’t understand enough about how strains are generated in an animal,” McKenzie says. Lab studies suggest that some may infect other animal species, too, but researchers have never found CWD in animals other than cervids in the wild.
So while the results in brain organoids suggest that at least some current strains don’t pose a high threat to people, it’s possible that new strains riskier to humans could emerge. “I still think that [chronic wasting disease] can jump into humans,” McKenzie says. But in more favorable news, she thinks such cases would be rare. “I don’t think it’s going to be an epidemic.”







