A blood test may show which COVID-19 patients steroids will help — or harm
Treatment timing can dramatically lower risk of death or needing a ventilator, or raise it
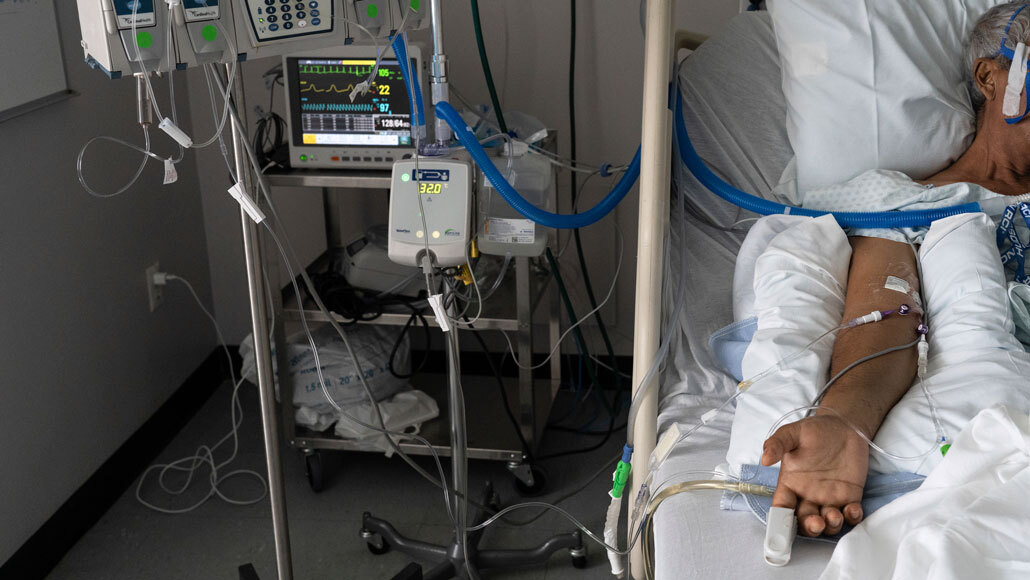
A COVID-19 patient gets treatment in the intensive care unit at United Memorial Medical Center in Houston. A simple blood test may help doctors decide who could benefit from treatment with steroids, lowering the risk of needing a ventilator or dying.
Stringer/Sputnik via AP
A cheap and easy blood test for inflammation may help determine which COVID-19 patients will benefit from getting steroids.
In an observational study of people hospitalized with COVID-19, those with high levels of an inflammation indicator called C-reactive protein in their blood had a reduced chance of dying or being put on a ventilator when treated with steroids. But steroid treatment more than doubled the risk of needing a ventilator or dying for people with low levels of the inflammation-indicating protein, researchers report July 22 in the Journal of Hospital Medicine.
“Steroids are Goldilocks drugs: They need to be given at the just right time,” says Luis Ostrosky, an infectious diseases doctor at the University of Texas Health Science Center at Houston who was not involved with the work. Giving steroids too early may rein in the immune system too much so that it can’t effectively fight the coronavirus, leading to the virus doing more damage. And “if you give steroids too late, the damage is already done.”
Using C-reactive protein as guide “may be the key to starting [steroids] at the right time,” Ostrosky says.
A large clinical trial in the United Kingdom called the RECOVERY trial has shown that the steroid dexamethasone can reduce the risk of death among COVID-19 patients who need extra oxygen or who are on ventilators (SN: 6/16/20). In that study, there was no benefit — and maybe a hint of harm — for patients who don’t need extra oxygen to breathe.
The new results are in line with those from the RECOVERY trial and may help explain why some patients do better on steroids than others, Ostrosky says.
Shitij Arora, a hospital physician at Albert Einstein College of Medicine and Montefiore Medical Center in New York City, noticed in mid-March that some patients coming into the hospital with COVID-19 had intense inflammation in their lungs, while others didn’t. Arora treated a handful of patients who had lung inflammation with steroids and saw some of them dramatically improve.

Trustworthy journalism comes at a price.
Scientists and journalists share a core belief in questioning, observing and verifying to reach the truth. Science News reports on crucial research and discovery across science disciplines. We need your financial support to make it happen – every contribution makes a difference.
“Of course, that’s not a study. They’re anecdotes,” says William Southern, chief of the division of hospital medicine at Einstein and Montefiore. That was before dexamethasone had been shown to be helpful and after a study in China suggested COVID-19 patients might be harmed by steroids.
Some other doctors at the medical center were also prescribing steroids — usually prednisone, but sometimes methylprednisolone or dexamethasone — for some patients. So Southern, Arora and colleagues put together an observational study to see how COVID-19 patients fared when put on steroids.
Arora hypothesized that a test for C-reactive protein might help doctors figure out which patients would benefit most. “It’s a cheap $20 test,” he says. Doctors started measuring the inflammation marker in the hospitals’ COVID-19 patients’ blood.
Among 1,806 patients in the study admitted to Montefiore’s four hospitals from March 11 to April 13, 140 were prescribed steroids. In 198 patients with levels of C-reactive protein of 20 milligrams per deciliter of blood or higher, steroid use reduced the chance of going a ventilator or dying by 77 percent, compared with those not taking the drugs. But in people whose C-reactive protein levels were 10mg/dL or lower, steroids increased the chance of death or ventilation by 2.64 to 3.14 times compared with those not taking the drug.
“Steroids are not appropriate for all. It’s just as important to avoid giving steroids to the people who may be harmed as it is to give steroids that may benefit,” Southern says.
The researchers plan to use data collected in this study to determine whether tracking levels of C-reactive protein can also predict whether patients are recovering.







