SWEAT NON-EQUITY Some people may have a greater genetic predisposition to obesity, which means they may have to work harder than others to lose weight or to keep from gaining it. A new study says there’s a way to predict who’s most at risk.
Kzenon/Shutterstock
There’s a new way to predict whether a baby will grow into an obese adult.
Combining the effect of more than 2.1 million genetic variants, researchers have created a genetic predisposition score that they say predicts severe obesity. People with scores in the highest 10 percent weighed, on average, 13 kilograms (about 29 pounds) more than those with the lowest 10 percent of scores, the team reports April 18 in Cell. The finding may better quantify genes’ roles in obesity than previous prediction scores, but still fails to account for lifestyle, which may be more important in determining body weight, other researchers say.
Still, the study shows that “your genetics really start to take hold very early in life,” says coauthor Amit Khera, a cardiologist at Massachusetts General Hospital and the Broad Institute of MIT and Harvard. Weight differences showed up as early as age 3, and by age 18, those with the highest scores weighed 12.3 kilograms more on average than those with the lowest scores, Khera and his colleagues found. Some people with high genetic scores had normal body weights, but those people may have to work harder to maintain a healthy weight than others, he says.
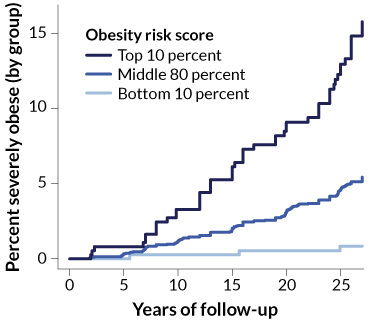
People with the highest scores were 25 times more likely to have severe obesity — a body mass index (BMI) greater than 40 — than those with the lowest scores. BMI is a measurement of body fat based on height and weight. A BMI of 18.5 (calculated as kilograms per meters squared of height) to 24.9 is considered healthy. BMIs 30 and above are considered obese.
The nearly 13-kilogram difference between people dealt a good genetic hand versus those dealt a bad one equals about five BMI points. “Five points is a lot,” Khera says. “That’s what takes you from normal to obese, from obese to severely obese.” High scores were also associated with increased risk of heart disease, diabetes, high blood pressure and stroke.
Other scientists are skeptical that the score is an accurate predictor of obesity risk.
“I’m not convinced at all,” says Ruth Loos, a genetic epidemiologist at the Icahn School of Medicine at Mount Sinai in New York City. Genes are responsible for about half of people’s susceptibility to obesity, but lifestyle factors such as diet and exercise are equally or even more important, she says. “Even if you have a genetic score that perfectly captures that 50 percent of genetics, you still will not be able to predict anyone’s future risk of obesity.” Without figuring in the lifestyle factors, “you will never be accurate.”
Together, the 2.1 million genetic variants used in the study account for less than 10 percent of genes’ contribution to obesity, making the score a blunt tool that could lead to inaccurate predictions, Loos says. For instance, the scores of 3,722 people in the Framingham Offspring study group — one group of people the researchers used to test their genetic score — suggested that 371 of the highest scorers would become severely obese. But only 58 of them did. “The score said bluntly, if you’re in the top decile you’ll become severely obese,” Loos says. “So you basically scared people who were not supposed to be scared.”
On the flip side, the score would have failed to warn 171 of the 229 severely obese people in the Framingham group that they would gain so much weight, she says. “If you simply use the score and don’t account for lifestyle, you’ll be wrong many times.”
Khera and colleagues hope the score will help erase the stigma associated with obesity and shed some light on the biology behind the condition. Although people with high genetic risks may have a harder time avoiding weight gain or losing weight, they also might be the people who benefit most from weight-control drugs or other measures, Khera says.
Endocrinologist and geneticist Mark Goodarzi of Cedars Sinai Medical Center in Los Angeles worries that giving people a prediction of looming obesity could backfire. That’s already happened in at least one study. People who were warned that their genes predisposed them to obesity ate more after learning of the propensity, he says. “I think they figured, ‘I’m doomed. I’m going to be obese anyway. Why fight it?’” Other studies have showed no change in people’s behavior after learning their genetic risks, he says.
It is not clear how doctors might use the score in treating patients, says A. Cecile Janssens, an epidemiologist at Emory University in Atlanta. “You should at least say in the discussion, ‘If we identify the people in the highest 10 percent, we can do X, Y and Z with these people, which we wouldn’t do with everyone else,’” she says. And instead of focusing on severe obesity, it might be more useful to be able to predict whether overweight people might become obese in order to prevent that transition. “You can [more] easily lose a few pounds than 30 or 40 pounds.”