Getting dengue first may make Zika infection much worse
Cell, mice experiments reveal antibodies gone rogue
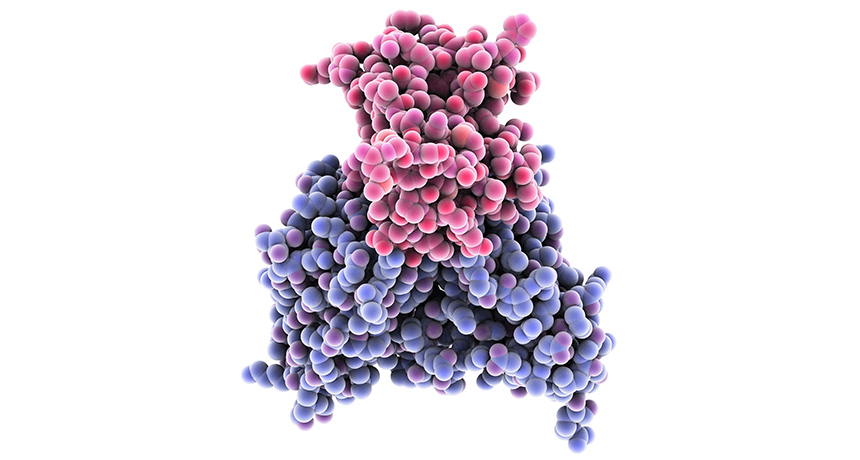
FRIEND OR FOE A dengue antibody (blue, shown bound to a dengue virus protein, red, in this molecular model) can ease Zika’s entry into cells, a new study finds.
Laguna Design/Science Source
Being immune to a virus is a good thing, until it’s not. That’s the lesson from a study that sought to understand the severity of the Zika outbreak in Brazil. Experiments in cells and mice suggest that a previous exposure to dengue or West Nile can make a Zika virus infection worse.
“Antibodies you generate from the first infection … can facilitate entry of the Zika virus into susceptible cells, exacerbating the disease outcome,” says virologist Jean K. Lim. Lim and colleagues report the results online March 30 in Science.
The study is the first to demonstrate this effect in mice, as well as the first to implicate West Nile virus, notes Sharon Isern, a molecular virologist at Florida Gulf Coast University in Fort Myers.
Zika is similar to other members of its viral family, the flaviviruses. It shares about 60 percent of its genetic information with dengue virus and West Nile virus. Dengue outbreaks are common in South and Central America, and dengue as well as West Nile are endemic to the United States.
Exposure to a virus spurs the body to create antibodies, which prevent illness when a subsequent infection with the virus occurs. But a peculiar phenomenon called antibody-dependent enhancement has been described in dengue patients (SN: 6/25/16, p. 22). The dengue virus has four different versions. When a person with immunity to one dengue type becomes sick with another type, the illness is worse the second time. The antibodies from the previous dengue exposure actually help the subsequent dengue virus infect cells, rather than blocking them.
Lim, of the Icahn School of Medicine at Mount Sinai in New York City, and her colleagues began their research with plasma from donors. Some had previously been sick with either dengue or West Nile; others had neither illness. Plasma is the fluid component of blood, which contains antibodies but lacks cells.
In one experiment with cell samples, Zika was able to infect cells more efficiently when the virus was mixed with plasma from dengue- or West Nile‒exposed donors than with plasma from individuals with neither illness. Zika was most aggressive in the presence of dengue.
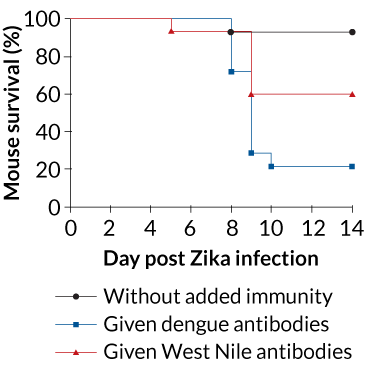
In a follow-up experiment, the researchers gave mice one of the three plasma samples, and two hours later, infected the mice with Zika. More than 93 percent of mice that received the plasma from individuals free of dengue or West Nile survived the infection. But the outcome for mice given plasma with dengue antibodies was stark: By the 10th day of infection, nearly 80 percent had died. The animals also displayed serious neurological symptoms, including paralysis. Of mice given plasma with West Nile antibodies, about 40 percent died from the Zika infection.
“This is important because in places where the Zika virus is causing outbreaks, such as South America, there are currently other circulating viruses, such as dengue, which is highly prevalent,” says Lim. Zika is spreading in the United States, where an estimated 3 million residents harbor antibodies to West Nile. “If you know you’ve been previously infected with West Nile or dengue, this needs to be considered as a risk factor,” she says.
With this work in hand, says Isern, the next step is to conduct clinical studies to “look at individuals who have been infected with Zika, get a good patient history, see if they’ve had previous dengue exposure, or West Nile, and determine whether or not the disease severity is worse.”
Editor’s note: This story was updated April 17, 2017, to correct the survival time frame for mice given plasma containing dengue antibodies and then infected with the Zika virus.