How meningitis-causing bacteria invade the brain
Experiments in mice show the microbes hijack cells in the brain’s protective cover
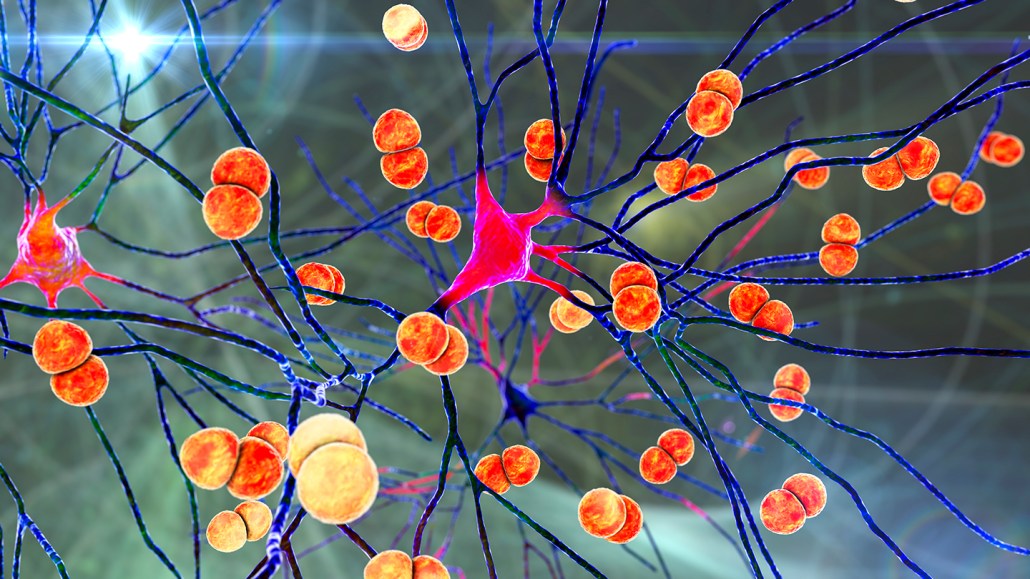
Streptococcus pneumoniae bacteria are one of the main causes of bacterial meningitis. In this illustration, the bacteria (orange) are infecting brain cells.
KATERYNA KON/SCIENCE PHOTO LIBRARY/Getty Images
Bacteria can slip into the brain by commandeering cells in the brain’s protective layers, a new study finds. The results hint at how a deadly infection called bacterial meningitis takes hold.
In mice infected with meningitis-causing bacteria, the microbes exploit previously unknown communication between pain-sensing nerve cells and immune cells to slip by the brain’s defenses, researchers report March 1 in Nature. The results also hint at a new way to possibly delay the invasion — using migraine medicines to interrupt those cell-to-cell conversations.
Bacterial meningitis is an infection of the protective layers, or meninges, of the brain that affects 2.5 million people globally per year. It can cause severe headaches and sometimes lasting neurological injury or death.
“Unexpectedly, pain fibers are actually hijacked by the bacteria as they’re trying to invade the brain,” says Isaac Chiu, an immunologist at Harvard Medical School in Boston. Normally, one might expect pain to be a warning system for us to shut down the bacteria in some way, he says. “We found the opposite…. This [pain] signal is being used by the bacteria for an advantage.”
It’s known that pain-sensing neurons and immune cells coexist in the meninges, particularly in the outermost layer called the dura mater (SN: 11/11/20). So to see what role the pain and immune cells play in bacterial meningitis, Chiu’s team infected mice with two of the bacteria known to cause the infection in humans: Streptococcus pneumoniae and S. agalactiae. The researchers then observed where that bacteria ended up in mice genetically tweaked to lack pain-sensing nerve cells and compared those resting spots to those in mice with the nerve cells intact.
Mice without pain-sensing neurons had fewer bacteria in the meninges and brain than those with the nerve cells, the team found. This contradicts the idea that pain in meningitis serves as a warning signal to the body’s immune system, mobilizing it for action.
Further tests showed that the bacteria triggered a chain of immune-suppressing events, starting with the microbes secreting toxins in the dura mater.
The toxins hitched onto the pain neurons, which in turn released a molecule called CGRP. This molecule is already known to bind to a receptor on immune cells, where it helps control the dura mater’s immune responses. Injecting infected mice with more CGRP lowered the number of dural immune cells and helped the infection along, the researchers found.
The team also looked more closely at the receptor that CGRP binds to. In infected mice bred without the receptor, fewer bacteria made it into the brain. But in ones with the receptor, immune cells that would otherwise engulf bacteria and recruit reinforcements were disabled.
The findings suggest that either preventing the release of CGRP or preventing it from binding to immune cells might help delay infection.
In humans, neuroscientists know that CGRP is a driver of headaches — it’s already a target of migraine medications (SN: 6/5/18). So the researchers gave five mice the migraine medication olcegepant, which blocks CGRP’s effects, and infected them with S. pneumoniae. After infection, the medicated mice had less bacteria in the meninges and brain, took longer to show symptoms, didn’t lose as much weight and survived longer than mice that were not given the medication.
The finding suggests olcegepant slowed the infection. Even though it only bought mice a few extra hours, that’s crucial in meningitis, which can develop just as quickly. Were olcegepant to work the same way in humans, it might give doctors more time to treat meningitis. But the effect is probably not as dramatic in people, cautions Michael Wilson, a neurologist at the University of California, San Francisco who wasn’t involved with the work.
Scientists still need to determine whether pain-sensing nerve cells and immune cells have the same rapport in human dura mater, and whether migraine drugs could help treat bacterial meningitis in people.
Neurologist Avindra Nath has doubts. Clinicians think the immune response and inflammation damage the brain during meningitis, says Nath, who heads the team investigating nervous system infections at the National Institute of Neurological Disorders and Stroke in Bethesda, Md. So treatment involves drugs that suppress the immune response, rather than enhance it as migraine medications might.
Chiu acknowledges this but notes there might be room for both approaches. If dural mater immune cells could head the infection off at the pass, it may keep some bacteria from penetrating the defenses, minimizing brain inflammation.
This study might not ultimately change how clinicians treat patients, Wilson says. But it still reveals something new about one of the first lines of defense for the brain.






