Natural Healing: Nanothread mesh could lead to novel bandages
By recasting clot-promoting protein fibers found in blood into a fine meshwork, researchers have devised a wound covering that may speed healing and never need removing.

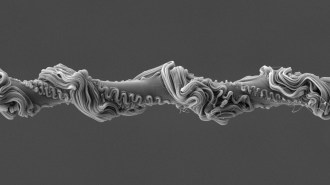
Gary L. Bowlin and his coworkers have produced mats of the protein, called fibrinogen, containing fibers just 80 nanometers thick. That’s comparable in thickness to natural fibrinogen fibers in people’s blood, says Bowlin, a biomedical engineer at Virginia Commonwealth University in Richmond.
Other researchers previously coated gauze bandages with fibrinogen or formed the protein into brittle, sponge-like materials (SN: 6/19/99, p. 396: http://www.sciencenews.org/sn_arc99/6_19_99/bob2.htm). In contrast, the new fibrinogen mats would become integral parts of a wound. Unlike standard gauze bandages, these strong, flexible mats actively promote blood clotting.
Bowlin and his coworkers created their mats from human or cow fibrinogen by modifying a process, called electrospinning, that’s long been used in textile manufacturing.
After dissolving the protein in a solution, the researchers applied an electric field that forced the fluid through a narrow nozzle toward a metal plate. While in the air, the fibrinogen threads dried and twisted, landing on their metal target like a delicate network of spaghetti. Increasing the protein concentration of the initial solution made the mats’ threads thicker; decreasing the concentration made the threads thinner.
Bowlin and his collaborators describe the mat-making process and the mats’ strength, flexibility, and nanoscopic structure in the Feb. 12 Nano Letters. Preliminary tests on rats have shown that the mats initiate clotting within seconds, says Bowlin.
The scientists now aim to determine the mats’ optimal mesh characteristics for specific medical uses, Bowlin says. One type of mesh might be best to prevent soldiers from bleeding to death on the battlefield while awaiting transport. Another might be most useful for stopping minor bleeding during surgery. What’s more, Bowlin suggests, fibrinogen mats might serve as scaffolds for tissue growth to treat damaged organs or replace lost body parts.
One concern with other fibrinogen wound-healing technologies is that one part of the multistep clotting process remains slow and incomplete, says biochemical engineer William Velander of Virginia Tech University in Blacksburg. Bowlin and his colleagues have yet to show they’ve overcome this obstacle, says Velander. However, because scientists suspect that greater surface area would boost the clotting process, the large surface area of the new mats “certainly is an encouraging first step in that direction,” he says.
The fibrinogen mats’ advantages and disadvantages in animals and people are still speculative, says chemist Glenn Prestwich of the University of Utah in Salt Lake City, but he finds the material “intriguing.” If their large surface area can be combined with sufficient elasticity and strength, they could become highly attractive for treating wounds, he says.
****************
If you have a comment on this article that you would like considered for publication in Science News, please send it to editors@sciencenews.org.