Healthy eating may not be as easy as following standard dietary recommendations. Fruits, vegetables, proteins and carbohydrates may affect people differently, although scientists still don’t know exactly why.
Jez Timms/Unsplash
Microbiologist Lora Hooper wishes she had a good answer when her mother asks, “What should I eat?”
Hooper could rely on a familiar refrain. Eat plenty of fruits, vegetables and whole grains, and limit meat and fat intake. Try to eat foods low on the glycemic index, a measure of how high a particular food is likely to send a person’s blood sugar after eating it.
Nutrition recommendations have focused on properties of food, debating whether focusing on calorie counts, carbohydrates, fats or proteins might be more important. But more studies are showing that people’s bodies can react very differently to the same foods, and standardized nutrition advice doesn’t fit everybody. Even identical twins can have varying responses to identical foods, new research finds, suggesting that the variety can’t be explained by genes alone.
With genetics being put on the back burner, researchers are searching for other explanations for why a diet one person swears by may cause another to gain weight. One big player may be the friendly bacteria and other microbes in people’s guts.
“Your microbiota really determines how many calories you take up from your food,” says Hooper, of the University of Texas Southwestern Medical Center in Dallas. Without a better understanding of how gut microbes will react, she says, “I don’t think I can read the number of calories in my food off a box.”
So instead of focusing on the food, people like Hooper’s mother may have to look within to their own gut microbes or other personal qualities to find the diet that works best for them, an approach known as personalized nutrition. But tailoring food regimens to individuals isn’t likely to be a piece of cake, either.
Finding the perfect diet is more important than ever as epidemics of obesity and type 2 diabetes sweep the globe. Worldwide, more than 1.9 billion adults and 380 million children and adolescents — about a quarter of the world’s population — were overweight in 2016, with 650 million of those people obese, according to the World Health Organization. An estimated 422 million people had diabetes in 2014, and rates of the disease have continued to grow.

Follow the guidelines?
Strive as they might to follow healthy diets, people may be thwarted by what they don’t know about their own response to food. Geneticist Tim Spector thought the small sandwich and glass of orange juice he typically bought in the hospital cafeteria was a healthy option. Then he discovered that both bread and orange juice send his blood sugar levels soaring into the diabetic range.
And “I get much worse sugar response to a banana than to an equivalent size of an apple,” says Spector, of King’s College London. He now chooses apples and pears over bananas. “It’s no hardship,” he says, “because I like both.”
Standard advice to eat fruits and vegetables, however, would never clue Spector in to which choice is truly healthier for him. He is not alone. Previous studies have determined that some people’s blood sugar may shoot up more after eating a banana than a cookie, while another person may have the opposite reaction (SN: 11/19/15).
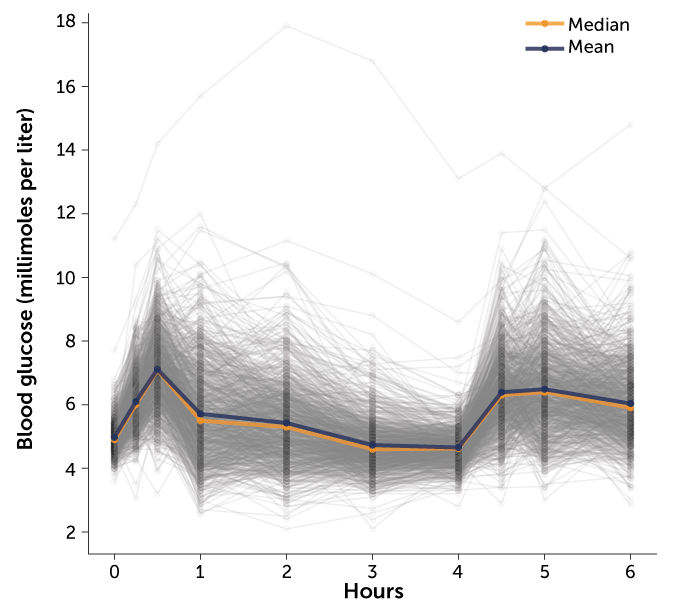
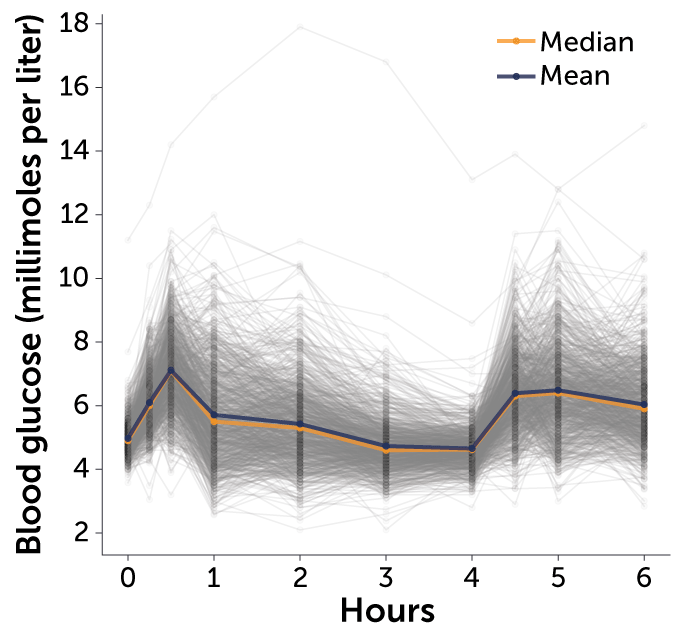
Spector and others have confirmed the varied landscape of blood sugar peaks and valleys that people achieve after eating standardized foods full of carbohydrates. In the short term, high blood sugar spikes might produce headaches and fatigue. Over the long haul, high blood sugar — the hallmark of diabetes — can lead to damage of blood vessels, nerves and organs.
It’s not just carbohydrates that produce a variety of responses. People respond differently to dietary fats, too, Spector and colleagues discovered in a new study tracking foods’ effects on more than 1,000 people, including hundreds of identical twins. Spector presented the preliminary, unpublished results June 11 in Baltimore at the American Society of Nutrition’s annual meeting.
Researchers in the PREDICT I study gave volunteers standardized foods and tracked participants’ blood levels of the sugar glucose, insulin and dietary fats called triglycerides. How quickly people cleared the fats from their blood after a meal couldn’t be predicted by knowing what happened to their blood sugar or insulin levels after a meal, the team found.
But perhaps the biggest surprise from the study was that even identical twins process food differently.
Follow the genes?
Identical twins Julie Hodgson and Diane Portlock look like each other. Except Portlock, a firefighter in Worcester, England, weighs about 50 pounds more than her twin. The 46-year-old sisters always put their weight difference down to lifestyle. After all, Hodgson, of Ash Vale, England, is a competitive rower in the British Army who took a gold medal in the United Kingdom Invictus Games trials in July. She exercises more than her sister does and tends to go for salads, while Portlock admits “I like cheese. I like bread. I like a glass of wine.”
But now the sisters have discovered that their bodies handle food differently, too. In an extension of Spector’s study, Hodgson’s blood sugar after a meal would usually rise gradually then taper off “in a nice little rounded arch,” her sister says. But Portlock’s glucose levels spiked and quickly fell and then rose again in what she calls “a double dip.”
“My insulin response is really quite efficient,” Hodgson says. Her body handles carbohydrates well, and eating more carbs fills her up and gives her more energy to train. But not all carbs work for her. Spaghetti Bolognese is Hodgson’s worst food for triggering a glucose spike, even though pasta is considered a low glycemic index food. Now, she avoids pasta and eats other carbs, including mashed potatoes, her twin’s nemesis for causing blood sugar spikes.

“Although our DNA and our genetics are the same, the study has proven that, in fact, we’re very individual as well,” Portlock says.
Genes explain less than half of an individual’s varying responses to food, Spector and colleagues calculate. That’s bad news for people who shell out money for consumer DNA testing companies to tell them what to eat (SN: 5/22/18), Spector says. “Genes are going to be limited when it comes to predicting food responses.”
What’s more, the macronutrient content of the food — the amount of carbs, fat and protein — accounted for only 16 to 32 percent of varying responses, the researchers found. The rest is still a mystery, and could relate to a litany of causes. Medications, the amount and quality of sleep people got, how much they exercised, when people ate and what order they ate foods in, their overall health and biological rhythms as well as the microbes living in the volunteers’ guts might all influence their reactions, Spector says. His team is recruiting volunteers for an even larger study aimed at better understanding the factors that influence metabolism.
Follow the microbes?
Gut microbes are probably the most important factor, says immunologist and microbiome researcher Eran Elinav of the Weizmann Institute of Science in Rehovot, Israel. Past research has shown that microbes determine how much fiber and other complex carbohydrates get digested. Bacteria in the small intestines may influence how much fat people absorb from their food, a study in mice suggests (SN: 7/25/19).
Elinav, Weizmann colleague Eran Segal and other collaborators have found that gut microbes play a big role in controlling how much a person’s blood sugar will spike after eating white or sourdough bread (SN: 6/6/17) or a wide variety of other foods.
The researchers have cataloged hundreds of gut microbiomes — the collection of genes in bacteria, archaea, fungi and other microbes that live in the intestines — responding to thousands of meals. By deeply analyzing, or sequencing, the genes of microbes in a person’s stool samples, and comparing the results with those from people previously studied, Elinav says he can tell what will happen to someone’s blood sugar after eating a specific food. Elinav and Segal are scientific consultants to a company called DayTwo, in Adanim, Israel, that’s based on the researchers’ work.
In February, scientists at DayTwo and the Mayo Clinic reported in JAMA Network Open that they had more accurately predicted volunteers’ glycemic responses to eating a bagel and cream cheese when the team based the prediction on each volunteer’s microbiome and previous response to the meal than when predicting blood sugars based on counting carbohydrates.
But here’s where things get sticky, because what people eat also affects the microbes in the gut in very personal ways.
“What you eat does determine which microorganisms are in your gut. There’s no question about that,” Hooper says. But exactly what about that food influences microbiome changes is a mystery.
It at least seems that microbes don’t count carbs, nutrition scientist Abigail Johnson of the University of Minnesota in Minneapolis and colleagues reported in the June 12 Cell Host & Microbe. Johnson’s colleagues — 34 students enrolled in a citizen science class at the university — were also the study’s research subjects. The students kept detailed food records and collected fecal samples every day for two and half weeks. The team cataloged the abundance of types of bacteria in each person’s stool samples and tried to determine which properties of food determined how the microbe mixes would change.
“We couldn’t look at nutrients and find relationships with nutrients and the microbiome,” Johnson says. But looking at foods eaten over the previous days predicted how the microbiome would change. For instance, knowing that a food was spaghetti with tomato sauce and meat told the researchers more about how the microbiome would change than knowing the carbohydrate, fat and protein content of the food did. Microbes may be more concerned with trace nutrients or chemical components of food that aren’t included on labels, Johnson says.
She thinks that the microbiome, at least the microbes in feces, probably aren’t the major driver of how a person responds to food. “It’s a player certainly,” but not the whole story, Johnson says.
To personalize or not to personalize
Other researchers caution against being too quick to discount the properties of the foods themselves. “The glycemic index is still an important worm in this can of worms,” says Jennie Brand-Miller, a nutrition scientist at the University of Sydney.
That’s in part because people’s variability to different foods is already baked into the glycemic index, Brand-Miller says. She likens the glycemic index to the tides. Although tides may vary from bay to bay, and season to season, “On any given day high tide will be higher than low tide.” Similarly, she says, “on any given day we have a 99 percent chance that high GI food will give a higher response than a low GI food.”
For most people, she argues, following standard nutritional advice will help them get and stay healthy.
But, Elinav says, nutritionists tend to place the blame for the failure of nutritional guidelines to stem the tide of obesity and diabetes on people not following the guidelines. “Rather than blaming the public for not following these recommendations, which often change, maybe the guidelines themselves are not sufficient or not evidence-based enough,” he says.
Personalizing nutrition may do better than the one-size-fits-all guidelines for controlling blood sugar, Elinav says. He and colleagues are pitting the conventional approach and their microbiome approach against each other in a head-to-head trial. The results may be known later this year.
Still, there’s probably no harm in eating within the standard guidelines. “I don’t think we’re going to get 20 years down this line of personalized nutrition research and find out fruits and vegetables are bad,” Johnson says. But in the future, people may be able to optimize those recommendations for themselves by adding or avoiding certain foods.
Until then, when Hooper’s mother asks what to eat, she can only reply, “Mom, I don’t know.”