The Power of D
Sunshine vitamin’s potential health benefits stir up, split scientists
A nutritional supplement that is free of charge, offers a wide range of health benefits and poses little risk sounds like fodder for a late-night TV commercial. But proponents of vitamin D are increasingly convinced that the sunshine vitamin delivers the goods, no strings attached.



It offers a safe route to better health, these advocates say, by promoting proper function of the bones, heart, brain, immune system, you name it. Yet, the proponents claim, most people don’t get enough. Whereas humans’ prehistoric ancestors lived outdoors and made oodles of vitamin D in their sun-exposed skin, people today have become shut-ins by comparison — and scant sun exposure means low vitamin D.
Of course, not everyone sees such a grand reach for the vitamin. While scientists concur that it is essential for bone maintenance, some stop right there. The skeptics note that vitamin D’s other promising qualities have shown up largely in studies that fall short of the gold standard of medicine — the randomized controlled trial, in which groups of people get either a placebo or the real thing. While a handful of randomized trials have shown additional benefits, others have not, leaving a gap in the vitamin’s otherwise sterling reputation.
This debate came to a head last November, when an Institute of Medicine panel of scientists announced new vitamin D recommendations. The old intake levels were barely high enough to prevent rickets, a bone condition associated with the Industrial Revolution. The IOM panel boosted the recommended daily intake of the vitamin from 200 to 600 international units per day for most of the population. The new dose is about 15 micrograms, in the range of vitamin D found in most multivitamins.
But these amounts still fall short of prehistoric people’s intakes by a Stone Age mile. Living outdoors with little clothing, these people manufactured thousands of international units, or IU, every day, perhaps getting three to five times as much as most people get now.
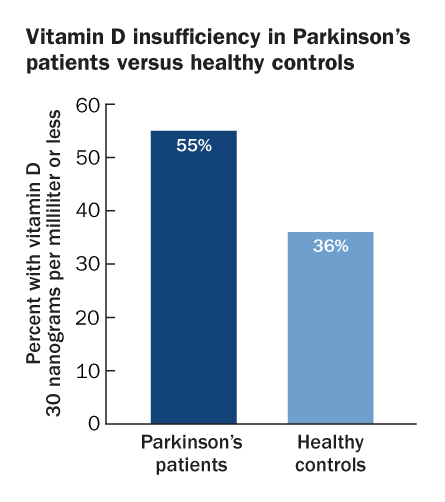
Vitamin D proponents cite a boatload of studies, some randomized and some not, suggesting that a population getting more vitamin D would be healthier overall. A recent Nebraska study links increased vitamin D intake to less cancer risk, for example, while Japanese scientists find that the vitamin helps fight influenza. Other recent work has connected higher levels of vitamin D with lower risks of hypertension, Parkinson’s disease and heart disease.
With these studies in hand, the Endocrine Society put out its own recommendations in the July Journal of Clinical Endocrinology & Metabolism. The society, the world’s oldest and largest group devoted to hormone research, called for vitamin D intake levels two to three times higher than the IOM’s recommendations.
More randomized trials are needed to settle the question, says Patsy Brannon, a molecular nutritionist at Cornell University and a member of the IOM panel. Until then, she says, it would be difficult to justify raising the levels further. It might even be imprudent because soaring levels could be toxic, she says.
That’s almost too much for nutritional biochemist Bruce Hollis to bear. A longtime vitamin D researcher at the Medical University of South Carolina in Charleston, Hollis recently oversaw a randomized controlled trial showing that low blood levels of vitamin D in pregnant women may lead to more preterm births. He has called for much higher doses. “These new IOM levels won’t accomplish anything,” Hollis says. “It’s just insane.”
Cancer connection
Endocrinologist Robert Heaney of Creighton University in Omaha, Neb., has spent a good part of his career compiling evidence that vitamin D has value in bone health and beyond, particularly in the fight against cancer. In a recent study, his team randomly assigned 1,180 healthy postmenopausal women to receive calcium, a placebo or 1,100 IU of vitamin D plus calcium daily.
Over four years, the trial data showed that those on the placebo had higher cancer rates than the other groups, but the findings revealed little difference between those getting calcium alone or calcium with vitamin D. Since cancer starts microscopically and can grow undetected for months or years, the researchers also ran an analysis that skipped the first year — an effort to discount preexisting cancers. During the last three years of the study, 6.8 percent of the placebo group and 3.6 percent of those getting only calcium developed cancer, compared with 2.0 percent of those getting vitamin D plus calcium, Heaney’s team reported in 2007 in the American Journal of Clinical Nutrition.
The Nebraska study is one of many looking for a possible link between elevated cancer risk and low vitamin D in the blood. Researchers have found a similar association between vitamin D and colon cancer and the formation of precancerous growths in the colon called polyps. And Michael Holick, a biochemist and endocrinologist at Boston University, can reel off studies demonstrating less prostate and ovarian cancer in populations with high sun exposure (meaning higher vitamin D levels).
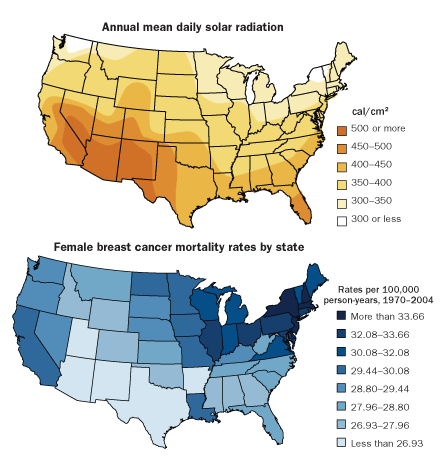
Holick, who chaired the committee that put out the Endocrine Society guidelines, acknowledges a risk of skin cancer from sun exposure in his 2010 book The Vitamin D Solution. But he and others have estimated, based on rates of cancer in the northern and southern United States, that lives saved from greater sun exposure would far exceed those lost to skin cancer.
Evidence for some cancers, he says, is better than others. “If I were to pick one cancer where vitamin D is sure to matter, it would be colon,” he says. “The second would be breast cancer.”
It’s one thing to crunch numbers and notice such associations among populations; it’s quite another to make a biological link. But some of vitamin D’s essential functions are directly anticancer in nature. For example, vitamin D regulates tumor-suppressing proteins called p21 and p27 and triggers other processes that inhibit cell proliferation. Vitamin D has also been shown to limit angiogenesis, the process whereby a tumor builds a web of blood vessels to nourish itself.
Tenacious D
Using an entirely different bag of tricks, vitamin D can stifle infections, a capability that was presaged nearly a century ago when doctors successfully treated tuberculosis with sun exposure. The strategy is now understood to stem from increased vitamin D, which has been shown to trigger cells to produce a handy protein fragment called LL-37 that kills the TB bacterium.
The vitamin appears to defend against viral infections, too. The annual winter flu season comes at a time when people garner little vitamin D from sunshine and blood levels fall. The timing may not be a coincidence, says Reinhold Vieth, a biochemist at the University of Toronto. Low vitamin D levels might offer the virus the edge it needs to gain a foothold in the population and spread from person to person.
Japanese researchers recently bolstered this theory with a study in which they randomly assigned 167 schoolchildren to get 1,200 IU of vitamin D daily and 167 other kids to get a placebo from December 2008 through the following March. Over that time, 31 children not getting the vitamin and 18 receiving it came down with the flu, Mitsuyoshi Urashima of Jikei University School of Medicine in Tokyo and colleagues reported in May 2010 in the American Journal of Clinical Nutrition.
Another study in the United States showed that substantially more people with low vitamin D develop upper respiratory infections than do people with more of the vitamin, and taking up to 2,000 IU a day reduced such infections by two-thirds in one trial. A Dutch research team also reported online in May in Pediatrics that babies with low levels of vitamin D at birth were several times as prone to develop a severe respiratory viral infection in the first year of life as were newborns with ample amounts.
Fighting infection is all well and good, but too much immunity can be a terrible thing. Ask anyone with an autoimmune disease, in which crossed-up immune defenses attack a person’s own tissues. Even milder immune missteps such as asthma and allergy can be difficult to endure.
But taking extra vitamin D doesn’t exacerbate these immune overreactions. If anything it provides an immune gyroscope that moderates them. “Vitamin D makes the immune system smarter, not stronger,” says John Cannell, a forensic psychiatrist at Atascadero State Hospital in California who also studies vitamin D.
Allergy, an immune reaction to innocuous substances, offers an example. When researchers led by Michal Melamed of the Albert Einstein College of Medicine in New York City analyzed vitamin D levels of more than 3,000 children, allergies to peanut, oak and ragweed showed up more often in children with less than 15 nanograms of vitamin D per milliliter of blood than in kids with at least 30 ng/ml, a level many scientists consider the minimum for good health.
“Vitamin D is seen as essential in immune function,” says Melamed, an epidemiologist and nephrologist. In theory, she says, lacking it early in life disrupts the immune system “and you start having immune reactions to things you should tolerate.”
Asthma, another immune malfunction that can wreak havoc in the lungs, also shows links to low vitamin D levels. In a study conducted at National Jewish Health respiratory hospital in Denver, researchers found that people with asthma who also had low levels of vitamin D had poorer lung function than asthmatics who had higher levels of the vitamin. The results, reported in 2010 in the American Journal of Respiratory and Critical Care Medicine, show that harboring less than 30 ng/ml of vitamin D was associated with higher concentrations of TNF-alpha, an immune protein known to exacerbate inflammation.
A more destructive immune revolt called autoimmunity has a link to vitamin D as plain as a map of the world. Patients with the autoimmune condition type 1 diabetes, or juvenile-onset diabetes, have to receive insulin injections for life because insulin-making cells in the pancreas are killed off by a self-directed onslaught. Cedric Garland, a public health researcher at the University of California, San Diego, has mapped type 1 diabetes around the globe, noting low rates in Barbados, Brazil, Sudan, Algeria and Cuba but a high rate of the disease in Finland, Scotland, Norway, Sweden and New Zealand. In 2008 in Diabetologia, he and colleagues note that the latitude effect follows sun exposure closely.
There are exceptions. Sunny Sardinia has the highest type 1 diabetes rate in the world, apparently because of the population’s genetic profile, and Latvia ranks low. But the overall trend is unmistakable. Many researchers have also noted a latitude trend in multiple sclerosis, a suspected autoimmune disease that is practically unknown in the tropics and most common in Scandinavia.
Because these observations constitute indirect evidence and not causality, some scientists dismiss the latitude theory. But under a microscope, the evidence becomes more direct.
Multiple sclerosis researcher Jorge Correale of the Raúl Carrea Institute for Neurological Research in Buenos Aires has found that patients in the throes of an MS relapse have vitamin D levels lower than do healthy people or patients in remission. MS is marked by inflammation that damages nerve coatings. Vitamin D enhances the development of an inflammation-fighting protein called interleukin-10 and reduces production of two pro-inflammatory proteins in blood from patients, Correale’s team reported in 2009 in Brain.
Brainwork, babies, blood pressure
Cancer, rogue immunity and infection are just three of the many ailments vitamin D may help ameliorate:
— Bruce Hollis and colleague Carol Wagner, also of the Medical University of South Carolina, randomly assigned 350 pregnant women to get 400, 2,000 or 4,000 IU of vitamin D daily starting in the second trimester. Women getting the highest dose were less prone to have preterm labor or preterm birth than the lowest-dose group, the researchers reported at a scientific meeting in 2010.
— By sifting through medical records, scientists from Kaiser Permanente found hypertension rates of 52 percent among adults with low vitamin D but rates of only 20 percent among those with plenty of vitamin D. The report appeared in the March Journal of Clinical Hypertension.
— In a study reported in 2010 in the Archives of Neurology, Finnish scientists investigating Parkinson’s disease found that nearly three decades after study volunteers submitted blood samples, those with the lowest initial vitamin D levels were most likely to develop the disease.
— Among elderly people in England, those with low vitamin D were at least 40 percent more likely to fail standard cognitive tests than those with high levels of the vitamin, a 2009 report in the Journal of Geriatric Psychiatry and Neurology showed.
— Patients with blood levels of less than 30 ng/ml of vitamin D were slightly more likely to have heart disease and faced a doubled risk of diabetes compared with patients who had higher vitamin D levels, researchers from the University of Kansas Medical Center in Kansas City reported at a meeting in 2010.
D is for discord
The IOM panel members acknowledged all of these findings — and didn’t use any of them in setting vitamin D recommendations. They were very forthcoming about why.
“We looked extensively at those areas,” Brannon says. In non-bone research, she says, “we found very limited randomized controlled trials, and evidence for cause and effect was not present.”
Some studies did get special note. Hollis’ trial in pregnant women is interesting but had yet to appear in a peer-reviewed journal, Brannon says, so it wasn’t used in setting the recommendations. The Nebraska cancer study was discounted because the most convincing finding used only three of the four trial years, says panel member JoAnn Manson, an endocrinologist and epidemiologist at Harvard Medical School. She says the full scope of a trial is the only fair measure and that secondary analyses lack credence.
Two large randomized controlled trials are now getting under way and will provide new evidence.
Physician Carlos Camargo of Harvard Medical School and colleagues at the University of Auckland are randomly assigning 5,100 older adults in New Zealand to get a monthly pill containing either a placebo or 100,000 IU of vitamin D — equal to about 3,300 IU a day. The trial will assess heart disease, infections and fractures. “It’s a high enough dose to get most participants up to 35 to 40 nanograms per milliliter, which is where we think we’ll find optimum benefits,” Camargo says.
Manson is leading a U.S. trial in which 20,000 people age 60 and older are being randomly assigned to get 2,000 IU a day or a placebo. Some will also get omega-3 fatty acids. Since they don’t know what they are getting, participants are allowed to take vitamin D supplements up to 800 IU daily on their own. Researchers will measure heart disease, cancer and stroke among the participants.
Manson says she hopes the trial “will provide important information about the balance of benefits and risks” of vitamin D.
Whatever the results, though, these two trials may not settle the question. A randomized trial is only as good as its design, Cannell says. Giving people huge doses of vitamin D once a month creates unnatural swings in the body. “Our ancestors didn’t get one day of sun then 29 days without it,” he says.
And Hollis says that the range between the amounts of vitamin D taken by the two groups in Manson’s trial may not be wide enough to establish an effect. Even if it were, differences between the groups could be blurred by natural sun exposure.
Regardless of the results, which won’t be available for at least four years, Garland says scientists have enough data to justify higher vitamin D recommendations. Waiting for more evidence simply leaves many people at risk of deficiency, he says.
Besides, randomized controlled trials have never been the sole arbiter of medical thinking or policy, Garland says: “If they were, we would all still be smoking cigarettes and no one would be wearing seat belts.” Nobody was randomly assigned to such hazards. Rather, a flood of other evidence established their risk and benefit.
Jack of all trades
Vitamin D differs from other vitamins in one major way: It is nearly impossible to get enough of it in the diet naturally. Instead, the sun provides it.
After the ultraviolet rays of the sun trigger the synthesis of vitamin D in the skin, the body modifies the vitamin into a steroid hormone. Such hormones are heavy hitters in molecular biology, which probably explains the vitamin’s seemingly broad benefits — ranging from maintaining bone strength to sharpening mental acuity.
Vitamin D triggers a huge range of cell activities by binding to the aptly named vitamin D receptor, a protein docking port found on cells throughout the body. This connection — like a password opening up a new computer screen — instructs the cell to activate or silence certain genes. Gene activity in turn influences which proteins are made or not made by the cell. Since the vitamin D receptor is found on a wide array of cell types, such gene tweaking can influence immune reactions, cell growth, muscle maintenance, calcium absorption, metabolism and other processes.
Sreeram Ramagopalan, a geneticist at Oxford University in England, and his colleagues reported in 2010 in Genome Research that more than 200 genes are awakened or silenced by vitamin D binding to its receptor. Other evidence suggests the number of genes indirectly affected by vitamin D could exceed 2,000.
Many details of the vitamin’s activity are still hazy, says Wesley Pike, a biochemist at the University of Wisconsin–Madison. But some are known. “For instance, vitamin D is largely pro-differentiative,” Pike says. Cell differentiation is like specialization, in which an existing cell takes on a new duty. “And cells promote differentiation at the expense of growth,” he says. Genes modulated by vitamin D hamper cell proliferation, meaning the vitamin has anticancer potential.
And while other activities of vitamin D are still being sorted out, one of its best-understood tasks is protection from disease. Cells called macrophages that kill bacteria, for example, don’t always have the chemicals required to do their job on hand, says Robert Heaney of Creighton University in Omaha, Neb. So, in a pinch, the cells consult their gene library — with the help of vitamin D — and use the DNA blueprints stored there to synthesize the needed chemicals.
Vitamin D may not cure anything by itself, Heaney says. “But it’s waiting in the wings, outside of cells,” he says. “It’s an enabling compound.”







