SARS Control: First nasal vaccine effective in monkeys
Inhaling a new experimental vaccine may offer protection against severe acute respiratory syndrome, or SARS. The vaccine, tested in African green monkeys, is the first to be administered directly to the respiratory tract and is also the first that confers immunity with a single dose.
“This could be used for local outbreak control,” says Peter L. Collins of the National Institute for Allergy and Infectious Diseases in Bethesda, Md. “It would be the most rapid way to vaccinate those at risk for SARS,” especially vulnerable health care workers, he says. SARS became a health crisis in 2003. To date, it has infected more than 8,000 people worldwide, killing 774.
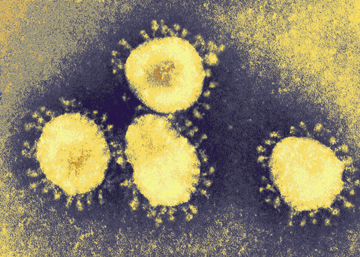
The virus that causes SARS has spiky molecules called S proteins protruding from its surface. These proteins enable the virus to infect mucosal cells in the respiratory system. To make the vaccine, scientists added the viral gene that encodes the S protein to the DNA of a different virus, BHPIV3. This bovine-human hybrid virus provokes an immune response, but no illness, in people and monkeys.
BHPIV3 is also being tested as a vaccine against the human form of the virus, which causes respiratory infections and pneumonia in children.
“A respiratory virus is really the ideal route for a SARS vaccine,” says Collins.
The researchers gave four monkeys respiratory doses of BHPIV3 containing the gene for S protein and provided four other monkeys with BHPIV3 augmented with an irrelevant gene. The BHPIV3 virus replicated in the respiratory tracts of all the animals, but only those monkeys that received the S-protein gene developed antibodies against the SARS virus, the scientists report in the June 26 Lancet.
After a month, Collins exposed the animals to the SARS virus to see whether those antibodies protected the monkeys from the disease. The SARS virus wasn’t detectable in the noses and throats of monkeys that received the
S-protein vaccine but did show up in the others. None of the animals became ill because African green monkeys don’t develop the symptoms of SARS.
Collins says that BHPIV3 is a good choice as the basis for a vaccine because it’s already been shown to be safe in people, a factor that would speed the FDA-approval process. The vaccine, however, may not work in adults. Most have immunity to BHPIV3 through childhood exposure to the human form of the virus. Decorating the viral surface with proteins that the human immune system doesn’t recognize could remedy this problem, Collins suggests.
Other vaccines against SARS are in the pipeline. One is already being tested in people in China. The developer of an injectable experimental vaccine for SARS (SN: 1/10/04, p. 28: Available to subscribers at SARS vaccine triggers immunity in monkeys), Andrea Gambotto of the University of Pittsburgh School of Medicine, says that his vaccine, too, could possibly be administered through the intranasal route.
No clinical trials are now planned for the BHPIV3 vaccine. “If SARS was rampaging through China, we’d probably rush it through testing,” says Collins. But because SARS currently seems to be under control, scientists are exploring multiple avenues to develop the most effective vaccine.
“I think all this research is exciting and interesting,” says Donna Ambrosino of Massachusetts Biologics Laboratories in Worcester, “but which [approach] at the end of day truly benefits us remains to be seen.”







