Switching off nerve cells eases asthma attacks
Inhaled anesthetic calmed coughing and inflammation in mice
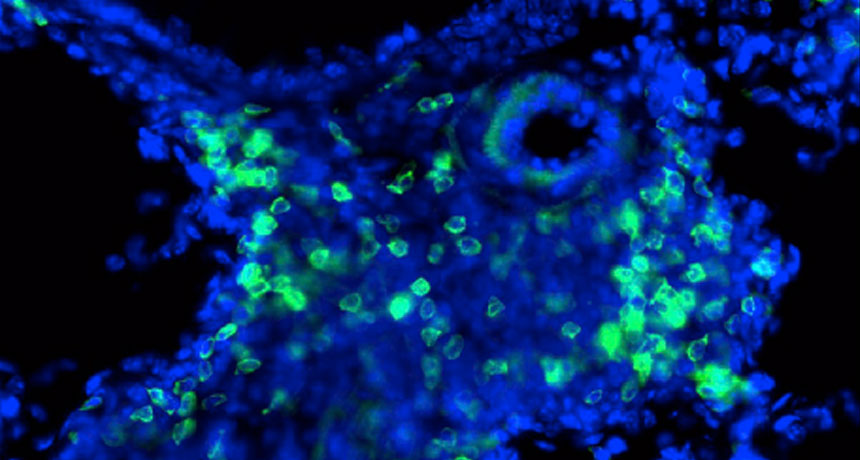
SPICE IT UP Pain-sensing fibers in a mouse’s airways can excite the immune system and crank up inflammation. Here, fibers that catch a whiff of the spicy chemical in hot peppers recruit immune cells (green) to the lungs. Numbing the fibers could ease asthma-related inflammation, a study shows.
S. Talbot et al/Neuron 2015