Device offers promise of no brain tumor left behind
New technique might allow surgeons to identify edges of cancers
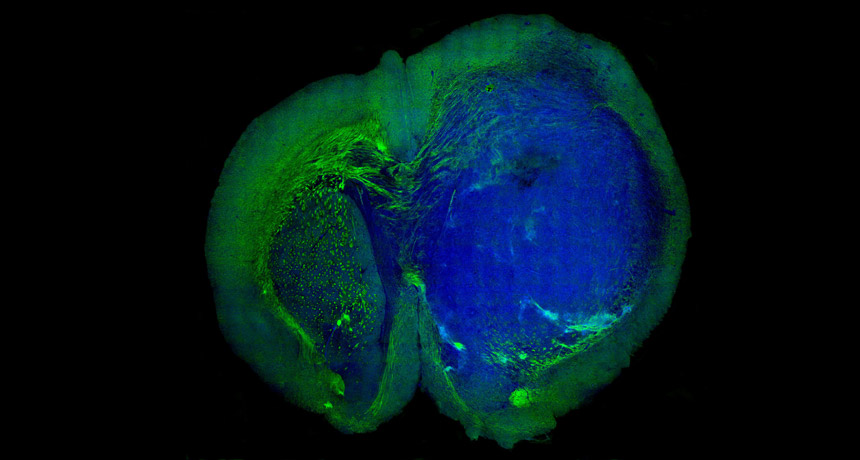
THE CUTTING EDGE A new technique generates colored images that differentiate tumor tissue (blue) in a mouse brain from surrounding healthy tissue (green). The technique may eventually improve brain surgery.
Ji et al/Science Translational Medicine