Medications alone work as well as surgery for some heart disease patients
Patients with stable ischemic heart disease can avoid stents or bypass surgery
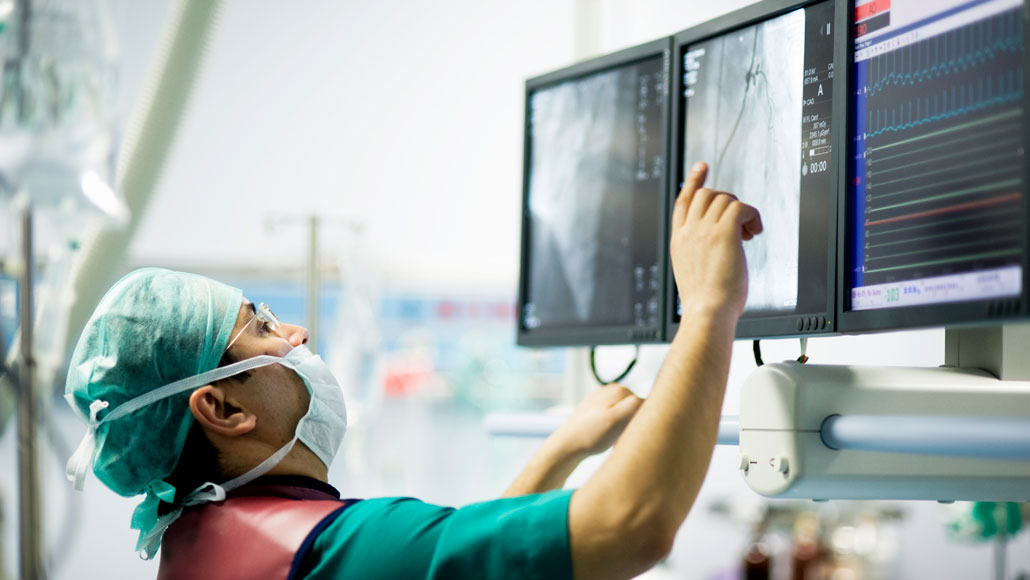
A doctor views an image of the heart during a coronary angioplasty, during which a tube is inserted into the vessels to clear a blocked artery and possibly place a stent. Some patients with heart disease could avoid this procedure and treat their condition with medical therapy alone, researchers say.
U.Ozel.Images/E+/Getty Images Plus