Mosquito spit can increase dengue severity
Blood vessels weakened by saliva may accelerate spread of virus
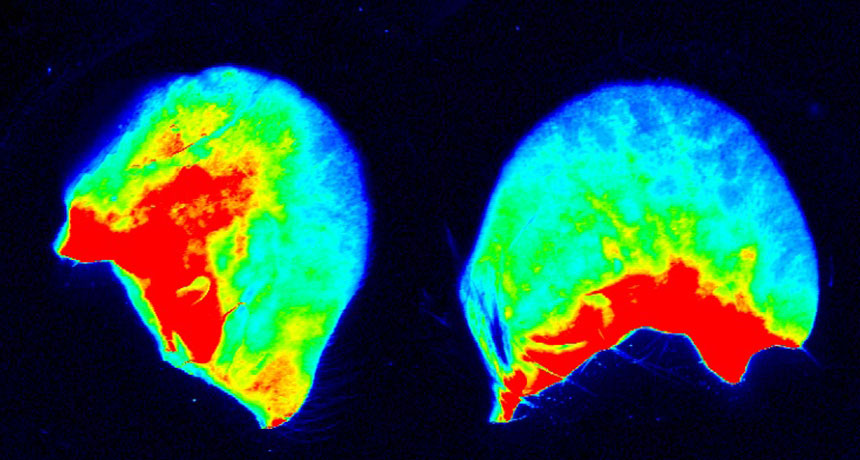
RED SPREAD A red marker molecule, about the size of the dengue virus, spread farther through a mouse ear when treated with an extract of mosquito saliva (left) than when not treated with the extract (right).
M.A. Schmid and D.R. Glasner







