‘Forever chemicals’ may pose a bigger risk to our health than scientists thought
Growing evidence of PFAS’ danger prompts new guidance for safe drinking water and health care

Most people in the United States are exposed to PFAS in their drinking water.
STEFANIA PELFINI, LA WAZIYA PHOTOGRAPHY/GETTY IMAGES PLUS
For decades, chemicals that make life easier — your eggs slide out of the frying pan, stains don’t stick to your sofa, rain bounces off your jackets and boots — have been touted as game changers for our busy modern lives. “Better things for better living … through chemistry,” was the optimistic slogan coined by DuPont, the company that invented the widely used chemical coating Teflon.
But this better living has come at a cost that is getting new attention. These chemicals — dubbed forever chemicals for their ability to last in the environment — are proving to have a lasting impact on human health. A growing body of research links the group of chemicals broadly known as PFAS, short for per- and polyfluoroalkyl substances, to conditions from unhealthy blood lipid levels to pregnancy complications to cancer.
Alarm about the health impacts of these chemicals has sparked a recent flurry of action from U.S. public health and regulatory officials. Warning that PFAS pose a greater health risk than previously thought, the U.S. Environmental Protection Agency in June dramatically lowered its recommended safe levels of the chemicals in drinking water.
“The updated advisory levels are based on new science, including more than 400 recent studies which indicate that negative health effects may occur at extremely low levels, much lower than previously understood,” Radhika Fox, assistant administrator of the EPA’s Office of Water, said in June at the Third National PFAS Conference, held in Wilmington, N.C.
Soon after, the National Academies of Sciences, Engineering and Medicine released the first clinical guidelines quantifying blood concentration levels of PFAS that could put someone’s health at risk. The 300-page report urges clinicians to recommend regular blood tests for anyone exposed to high levels of the chemicals and to provide information on how to limit exposure, such as installing special filters known to reduce PFAS in drinking water.
In the United States alone, by one measure, the tally in medical care costs and lost productivity from PFAS exposure linked to five medical conditions adds up to at least $5.5 billion annually, researchers at New York University reported July 26 in Exposure and Health. Those conditions include low birth weight, childhood obesity, hypothyroidism in women, and kidney and testicular cancers.
“We only looked at two of the more than 9,000 chemicals in the PFAS family, so we’re just seeing the tip of an iceberg,” says Leonardo Trasande, a pediatrician and environmental health expert at NYU Langone Health.
PFAS are found in many products, including:
- Firefighting foam
- Paint
- Sunscreen
- Makeup
- Dental floss
- Textiles
- Guitar strings
- Artificial turf
- Microwave popcorn bags
- Fast-food packaging
- Carpeting

Ubiquitous chemicals
Among those most at risk of exposure are firefighters: PFAS make protective gear more water resistant, and the chemicals are found in a widely used fire suppressant foam. But most people have some measurable level of PFAS in their bodies, according to the U.S. Centers for Disease Control and Prevention. Exposure typically comes from ingesting PFAS-contaminated drinking water or food grown in soil treated with fertilizers made from sewage contaminated with the chemicals (SN: 11/24/18, p. 18). An estimated 2,854 locations across the United States have PFAS contamination.
“People and communities have had significant exposure to these chemicals. If they can ID that they are in an area of significant exposure, they should seek testing through their usual source of care,” says Ned Calonge, an epidemiologist at the Colorado School of Public Health in Aurora who chaired the committee that wrote the National Academies report. The committee linked PFAS exposure to a slightly different list of conditions than the NYU team, finding “sufficient evidence” linking PFAS to four conditions: poor antibody response to vaccination, abnormally high cholesterol levels, decreased infant and fetal growth, and kidney cancer. Evidence was “suggestive” for breast and testicular cancers, as well as thyroid problems and ulcerative colitis, an inflammatory bowel disease.
The report calls for more research into the health effects of PFAS, noting gaps in evidence on everything from neurological issues to bone density. These chemicals have a wide range of impacts on multiple systems in the body, Calonge says. And they’re “ubiquitous in the environment.”
How PFAS cycle through the environment
-
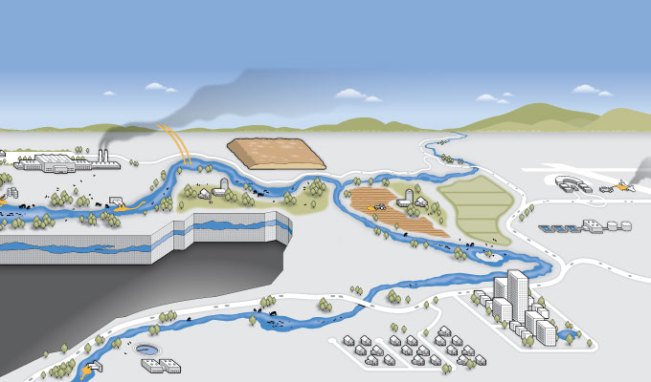
Forever chemicals cycle through the environment in the air, water, soil and sediments — and can eventually accumulate in wildlife and people. David Puckett/National Wildlife Federation -

Facilities that produce PFAS or use them in industrial processes are a primary source of contamination. The chemicals can leach into surface water and groundwater. Smokestack emissions can also deposit the chemicals into waterways. From left: David Puckett/National Wildlife Federation; sstop/E+/Getty Images Plus -
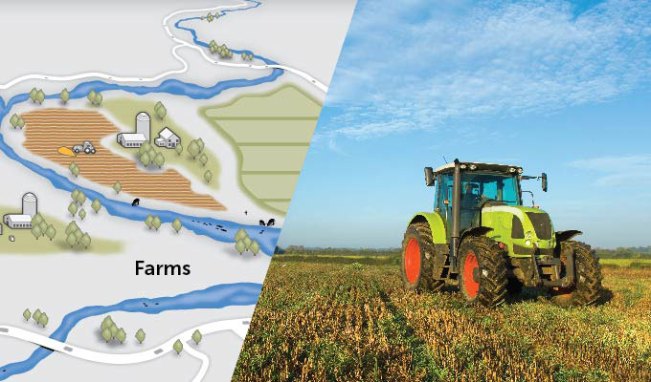
Sludge from wastewater treatment plants, called biosolids, can contain PFAS and is often spread on farms as fertilizer, leading to food, groundwater and surface water contamination. From left: David Puckett/National Wildlife Federation; Mint Images/Mint Images RF/Getty Images Plus -

PFAS in products disposed of in landfills can leach into groundwater or travel via runoff into surface water. From left: David Puckett/National Wildlife Federation; Nora Carol Photography/Moment/Getty Images Plus -

Firefighting foams used at airports, military bases and other facilities can release PFAS to surface and groundwater. From left: David Puckett/National Wildlife Federation; sunara/E+/Getty Images Plus -
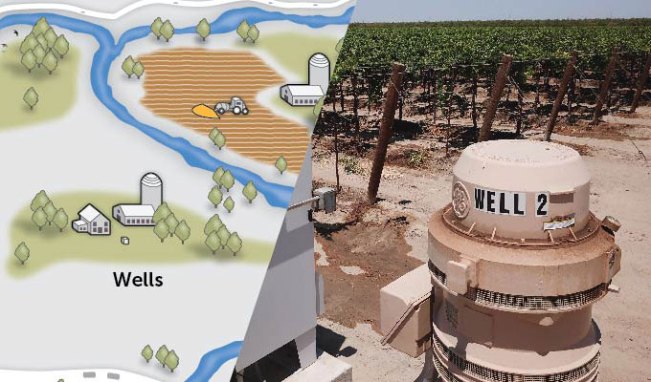
Both public and private water wells can contain PFAS-tainted groundwater. From left: David Puckett/National Wildlife Federation; ROBYN BECK/AFP/Getty Images Plus -

PFAS can pollute drinking water sent to homes and businesses because public utilities are not designed to remove the chemicals. From left: David Puckett/National Wildlife Federation; Brad Vest/Getty Images Plus -
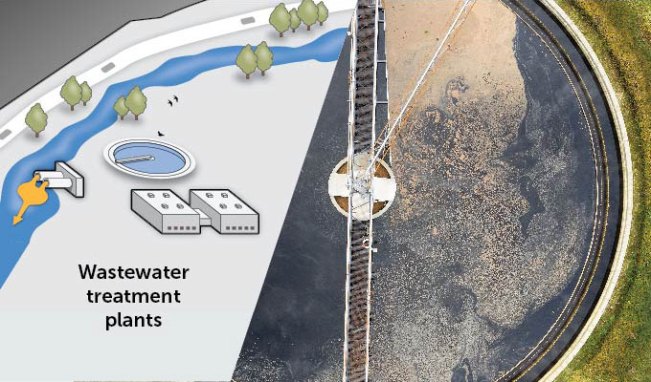
Wastewater treatment plants were not designed to remove PFAS. Treated water that contains PFAS can be discharged downriver to other public drinking water systems. From left: David Puckett/National Wildlife Federation; Bim/E+/Getty Images Plus
Newer, not safer
PFAS have been produced in the United States since the 1940s. Because they are good at repelling oil and water, holding up at high temperatures and reducing friction, the chemicals became useful for a vast array of products, including carpeting, upholstery, food packaging and even dental floss. Yet, relatively few of the 9,000 or so versions of these synthetic chemicals have been studied for their toxicologic effects.
Many PFAS are now recognized as endocrine disruptors, chemical compounds that interfere with the normal functioning of the endocrine, or hormonal, system. But PFAS have other effects that can boost cancer risk, such as weakened immunity, excessive cell growth and altered gene activity. One study found a greater than twofold increase in kidney cancer risk between people with the highest versus lowest blood levels of one common PFAS called perfluorooctanoic acid, or PFOA, researchers reported in 2021 in the Journal of the National Cancer Institute.
A newer generation of PFAS was assumed to be safer because the chemicals are less likely to accumulate in the body. But these newer compounds are structurally similar to the older ones and can be just as harmful to health as their cousins, Trasande says. These newer molecules “are increasingly being associated with diseases like gestational diabetes. We’re just starting to see the bigger problem that might be at play.”
The EPA’s new drinking water advisory aims to tackle both old and new PFAS. It targets two of the earlier and most commonly found kinds of PFAS in the environment: PFOA and perfluorooctane sulfonic acid, or PFOS. The advisory reduces the level of drinking water contamination below which adverse health effects are not expected from 70 parts per trillion to 0.004 and 0.02 ppt, respectively. Those levels are based on routine exposure to them over a lifetime.
The EPA’s health advisory also provided the first-ever recommendations on two of the newer kinds of PFAS: hexafluoropropylene oxide dimer acid and HFPO ammonium salt, collectively known as GenX chemicals, and perfluorobutane sulfonic acid, or PFBS. The agency set the drinking water safety threshold at 10 ppt for GenX chemicals and 2,000 ppt for PFBS. These newer chemicals have similar persistence in the environment, the agency states.
Health impacts
A National Academies panel found sufficient and suggestive evidence that PFAS boost risk for several ailments.
* in adults, † in children
Sufficient evidence
- Poor antibody response to vaccination *†
- Abnormally high cholesterol levels *†
- Decreased infant and fetal growth
- Kidney cancer *
Suggestive evidence
- Breast cancer *
- Liver enzyme alterations *†
- Pregnancy-induced hypertension *
- Testicular cancer *
- Thyroid disorders *
- Ulcerative colitis *
Consumers can ask their municipal water provider for data on PFAS testing in their area. Testing is becoming more common, and providers should be able to list which PFAS they test for. Private wells can be contaminated with PFAS if they are near manufacturers that produce or use the chemicals, as well as airfields where PFAS are used for firefighting, firefighting training areas and some waste disposal sites. People with private wells near one of these facilities can get their water tested. The EPA is giving grants to help underserved small and disadvantaged communities provide household water quality testing and comply with drinking water regulations.
PFAS price tag
Because there are limited available data on the health effects of the newer generation of chemicals, the NYU and National Academies reports focused on the impacts of older PFAS.
First, the NYU team examined PFAS chemicals in blood samples obtained from roughly 5,000 adults and children who participated in the U.S. National Health and Nutrition Examination Survey. Then, based on earlier studies linking PFAS to certain diseases and models that estimate medical costs and lost worker productivity for these illnesses, the team came up with its PFAS price tag.
Childhood obesity, the largest contributor to the overall economic toll of PFAS exposure, costs about $2.7 billion a year, the team estimates, followed by hypothyroidism in women at $1.26 billion. When the researchers considered other PFAS-linked diseases beyond the top five, such as endometriosis, obesity in adults and pneumonia in children, the estimated economic burden rose to as much as $63 billion annually.
Assessing risk
The National Academies report focused in part on how to curb that toll by providing testing guidelines to clinicians to detect high levels of PFAS in the body and try to reduce exposure.
The report provides the first clinical guidelines on how to assess a person’s disease risk. A person with a PFAS blood concentration of less than 2 nanograms per milliliter doesn’t have to worry. But for patients with blood concentrations between 2 and 20 ng/mL, clinicians should screen for conditions like unhealthy levels of fat in the blood, which can lead to heart problems. Such screening is especially important for people more vulnerable to the effects of PFAS exposure, like children, pregnant people and those who are immunocompromised. For anyone who tests above 20 ng/mL, the report encourages routine screenings for some cancers, thyroid problems and ulcerative colitis.
“For almost 20 years, we’ve been able to measure PFAS in people’s blood, but there was no guidance to say what [those measurements] mean,” says National Academies report coauthor Jane Hoppin, who heads the Center for Human Health and the Environment at North Carolina State University in Raleigh. “For the first time, this actually sets some ranges, some guidance for what could be levels of concern, and what kinds of health follow-up might be appropriate.”
She hopes that the recommendations will increase testing availability and make both doctors and patients more aware of these chemicals and their health risks. The report also encourages doctors to work with their patients to figure out where they are being exposed to PFAS and how to mitigate those risks, by cutting down on PFAS-containing products and filtering water.
Activated carbon filters, found in some countertop or pitcher filters, don’t remove PFAS as completely as reverse osmosis filters, researchers at Duke University and North Carolina State reported in 2020. The National Academies report offers a link to NSF, a testing organization that offers technical details on which filters actually filter out PFAS.
Efforts like reducing PFAS in drinking water could help. While EPA’s health advisories are recommendations and not enforceable, Trasande is pleased that the agency acted quickly, particularly on newer chemicals like GenX. But he argues that in light of what we already know and are continuing to learn about the disease burden caused by these chemicals, PFAS should undergo more testing before they are approved. Better yet, they should be regulated by class instead of taking what he calls a whack-a-mole approach.
“Our environmental policy still takes a wait-and-see approach that we should wait 20 to 30 years, which is the time that people take to develop diseases due to chemical exposures,” he says.







