Protein in Parkinson’s provokes the immune system
Immune cells treat bits of alpha-synuclein as intruders
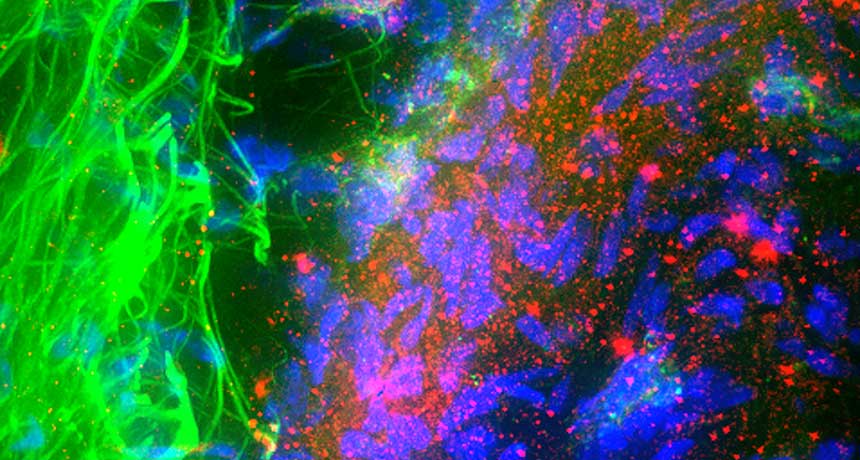
RED ALERT This micrograph shows how the protein alpha-synuclein (red) builds up in nerve cells (blue) in brains affected by Parkinson’s disease. The immune system can react to parts of the protein, a new study finds.
Roger J. Bick & Mya C. Schiess/UT-Houston Medical School/Science Source







