Sick and down
To fight off an infection or illness, the body shifts into a slow-down mode that mirrors some symptoms of depression. In fact, scientists now think the immune response itself may even cause the mood disorder.
When one of psychiatrist Andrew Miller’s patients asked about receiving the best drug available for treating hepatitis C, Miller said: “No way.” The patient — in his early 20s and accompanied by his mom to the appointment — had no job, few friends and a history of depression. While Miller knows that hepatitis C patients often benefit from the new generation of immune-boosting treatments, he’s keenly aware that those same immune therapies have a strong tendency to bring people down — and, in people predisposed to depression, dangerously down.
Certain immune proteins in the body appear to mess with the minds of otherwise healthy, but depressed people as well. Those who suffer from major depression have higher levels of cytokines, immune proteins the body makes to fend off infections and to patrol the body for disease, and which laboratories mimic. Excess cytokines have also been found lurking in the postmortem brains of suicide victims. “It raises the issue, how much of how we feel — how much of who we are as people — is dictated in terms of our immune system?” says Miller, a researcher at Emory University in Atlanta.
Though the connection between the body’s immune response and depression has only gained firm support in the last five years, it’s already catalyzing a revolution in antidepressant drug development. In hindsight, an emotional reaction to surging immune molecules does not seem so surprising. Cytokines are among the first immune proteins to respond to infection. Some direct swelling and fevers. Others order the body to rest, and so the sick take to the bed and decline party invitations, showers and even homemade dinners. The powerful molecules influence wants and needs by altering levels of substances like serotonin in the brain. Essentially, cytokines command the body to conserve energy when it’s sick. “A little depressed behavior is a survival mechanism in that sense,” Miller says. But when inflammation is artificially or erroneously triggered, prolonged sickness behavior may morph into depression and do more harm than good.
Figuring out the biology behind depression should help doctors combat the disorder, which strikes an estimated 14.8 million American adults each year, according to the National Institute of Mental Health. More than one in six individuals will experience major depression in their lifetime. And when depression coincides with chronic diseases like multiple sclerosis, cancer or diabetes, patients’ conditions are less likely to improve.
Psychiatrists and pharmaceutical companies have noted the downpour of evidence linking inflammation to depression. Miller says he and his colleagues have considered creating a new diagnostic category: Major Depressive Disorder with Increased Inflammation. To combat this depression, he says, researchers must find a way to alter the body’s immune response. It is a risky strategy but one that offers hope to the nearly 30 percent of all depressed patients who don’t respond to the antidepressants currently on the market.
Jekyll-and-Hyde changes
Cytokines emerged as the primary suspects for what’s since become known as inflammation-induced depression after Miller and others noticed that cancer patients became inexplicably upset during treatment with synthetic type 1 interferons, cytokines that block viral replication in infected cells. One of these, interferon-alpha, is among the most effective drugs for patients battling cancer and the hepatitis C virus. Yet the treatment has become notorious for causing major depression and other behavioral changes in more than half of these patients, depending on the dose of the immune booster.
Miller describes a “Jekyll-and-Hyde– type change” in one of his patients after interferon therapy. Eight weeks into it, the patient dumped his girlfriend, began dressing in black and grew a goatee. And there was another woman, Miller recalls, who took a drastic downward turn. “One of my most positive patients had been battling cancer for years, yet four weeks into the cytokine therapy she was distraught,” he says. “She told me, ‘I love my husband and my children, but I don’t want to be around them. I want to be left alone, and I don’t know why.’ ”
As observations of sadness, irritability, insomnia, fatigue and loss of appetite — all classic symptoms of depression — mounted in patients treated with immune boosters in the 1990s, papers published nearly a decade earlier in veterinary journals resurfaced. Benjamin Hart had been writing about the behavior of sick animals since the mid-1980s. “Depression was the first sign we had that an animal was sick,” says Hart, an animal behavior researcher at the University of California, Davis. In a seminal 1985 paper in the Journal of the American Veterinary Medical Association, he put forth the argument that animal malaise serves a purpose.
“People would call in and say that the dog is sleeping more than usual. They give the dog its favorite treat, and it only nibbles at it and then drops it, or they’d say the cat looks scruffy,” Hart explains. “Cats usually groom all the time.” He says that when he ran blood and urine tests on such animals, he usually discovered signs of bacterial or viral infection. Instead of assuming the pet acted sad because it wasn’t feeling well, he suggested that the pet’s behavior was part of its immune response. Fido’s body forced the animal to devote its energy to battling illness, instead of to chasing squirrels.
Furthermore, since all mammals act similarly when sick, Hart suggested that the behavior had been inherited from a common ancestor who survived infection better than other animals who had not evolved the behavioral response.
In the 1990s, researchers in the Netherlands reported that patients with major depression showed signs of inflammation, with elevated levels of cytokines in their blood and cerebrospinal fluid. And in 2001, Robert Dantzer, now at the University of Illinois at Urbana-Champaign, injected rats with cytokines. Sure enough, Dantzer says, the rats lost interest in previous pleasures and activities: They didn’t care for sugary water, they didn’t run on the wheel and, when placed in a pool of water they swam lethargically, barely keeping their heads above water.
Miller compares this sickness behavior to “holing up in a cave.” Although the animal has little drive to do much of anything, it does stay alert to major threats. “While in the cave, the organism rests but keeps one eye open,” he says. That may explain why people with the flu, as well as people with depression, neither leave the couch nor get the deep sleep they crave.
Connecting body to mind
Like army generals, innate immune cytokines order inflammatory molecules to prepare for war when the body is under threat from invasive bacteria or viruses, or under perceived threat in the form of stress or chronic disease. In these situations, cytokine levels rise. “It’s a good thing if you’re running from a tiger,” explained psychiatrist Dominique Musselman in May at a meeting in Washington, D.C., of the American Psychiatric Association. “You’d want to rev up your immune system to prepare for an injury.” Nowadays, however, angry bosses, aggressive creditors and disappointed spouses have replaced vicious predators, she said. And as those stressors are less likely to bite, the subsequent immune response, which had evolved to heal injuries and fight infection, seems a vestige of the distant past.
“The fact that stress can activate the innate immune response has been a major breakthrough,” Miller notes. Add this to one more piece of the puzzle: Stress often leads to depression. The immune system may explain why.
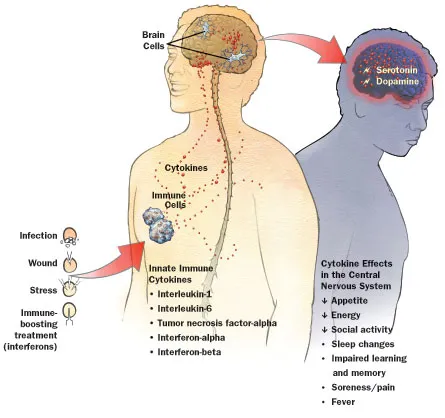
In mapping out the molecular pathway between elevated cytokines in the body and chemical changes in the brain, scientists aim to provide targets for drugs intended to treat depression caused by inflammation. In the last few years, researchers have identified primary suspects. Many cytokine proteins, including tumor necrosis factor-alpha, interleukin-6 and the type 1 interferons (IFN-alpha and IFN-beta), have been accused of being the principal perpetrators in sickness behavior. They respond rapidly to foreign intruders, circulate in the bloodstream and initiate a response in the central nervous system.
Cytokines manufactured in the body can send messages through the central nervous system to induce production of cytokines in the brain. That message may be relayed when cytokines sneak into the brain through leaky regions in the blood-brain barrier, a series of structures that block most substances. In the brain, cytokines activate inflammatory middlemen who tag-team their way to affecting emotion-regulating neurotransmitters. As neurotransmitter levels change, so can mood. “Among other things, we see a drop in levels of serotonin, the feel-good chemical,” Miller says.
Attempts are underway to treat depression by blocking specific cytokines or the messages they send. A 2006 clinical trial funded in part by the biotech company Amgen found that depressed patients who suffered from psoriasis, an autoimmune skin disease associated with increased levels of cytokines, felt happier after taking the cytokine blocker etanercept (brand name Enbrel), which affects tumor necrosis factor-alpha. Another TNF-alpha blocker, infliximab (Remicade), is being tested for use in depressed patients who don’t respond to antidepressants such as the selective serotonin reuptake inhibitors Prozac and Zoloft. Those results should be ready by 2010, says Charles Raison, a research psychiatrist at EmoryUniversity who heads the project.
Anti-inflammatory drugs like aspirin and ibuprofen haven’t been shown to affect mood. But another anti-inflammatory, celecoxib (Celebrex), that more specifically blocks the inflammatory molecule COX-2, helped heal depression in a small clinical trial in Germany. Norbert Müller, a psychiatrist on that study from Ludwig-Maximilians-University Munich, suggests that a high dose of aspirin would be needed to inhibit COX-2 as strongly as celecoxib. And that, he says, “would provoke a high rate of side effects, mainly gastrointestinal pain and possibly bleeding.”
Developing these types of treatments isn’t easy, warns Dantzer. Compounds that interfere with immune responses have the dangerous potential to compromise the body’s resistance to infection. The goal is to temper inflammatory molecules in the brain, not the body.
Researchers will have to identify safe points to alter along the molecular pathway that runs between bodily cytokines, molecular middlemen and neurotransmitters in the brain. “The further upstream you go towards the cytokines, the more far-reaching the effects on the body. If you move downstream to block cells that are activated by the inflammation, you may have a drug that is less toxic,” Miller says.
Custom-made meds
Another problem is identifying the cases in which the immune system is to blame. “The evidence is clear at this point that inflammation events can lead to a depressed mood,” says neuroscientist Steven Maier of the University of Colorado at Boulder. “The issue is how often this is the case.”
Not all people are sensitive to surges in cytokines. Some recover from the side effects of interferon therapy as gracefully as some lovers rebound from heartbreak. Variations in a couple of genes may help doctors to predict who is most susceptible to immune-related depression. Miller and collaborators found that patients with hepatitis C were more resistant to interferon-induced depression if they possessed a slight variation in the gene encoding the serotonin transporter 5-HTT, which is known to be involved in psychiatric disorders, as well as another small variation in a gene that codes for the cytokine interleukin-6. The fact that the interleukin-6 gene, involved with inflammation, has an emotional impact provides more evidence of how the body and mind interact, the researchers report in the May 6 Molecular Psychiatry.
Identifying these genes is part of a larger effort by doctors to tailor treatment to the individual. “Ideally there could be a drug where one size fits all, but that doesn’t seem to be the case,” Miller says. He thinks that while serotonin reuptake inhibitors like Prozac work for certain people, others might need an immunological approach to combat depression. “We want to bring to people’s attention the interaction between factors,” he says. “This is the idea behind personalized medicine.”
Others agree that depressed patients unaided by standard treatments may be good candidates for an immune approach. “People who don’t respond to those [therapies] seem to have increased levels of inflammatory markers,” Raison says.
As logic, and misfortune, would have it, depression caused by inflammation is most prevalent in patients who have diseases associated with increased inflammation. Rates of depression are five to 10 times higher than average in patients with disorders that involve the immune system, including infectious diseases, cancer and autoimmune disorders, say Miller and Raison in a March report that appeared online in FOCUS. Inflammation is also a risk factor for diabetes and cardiovascular disease. When these diseases coincide with depression, patient outcomes can worsen.
Sickness behavior leads to grumbling under the covers. And grumbling under the covers hinders the hope and drive that patients need to follow doctors’ orders. Depressed patents are more likely to skip appointments and stop taking their medication, Musselman said at the APA meeting. And depressed smokers are more likely to continue smoking after bypass surgery.
By treating those susceptible to depression early on, doctors may increase their patients’ chances of surviving disease. “The idea,” Maier says, “is to cut depression off at the pass.”







