Many pills and injections could become history if a group of drug-delivery researchers has its way. The team has fabricated a polymer microchip that stores multiple drug doses and, when implanted in the body, could automatically release the medications at programmed intervals.
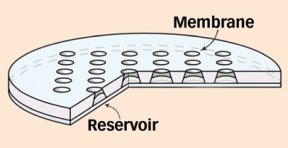
The paper-thin, dime-size chip contains a series of tiny reservoirs. Each reservoir can store a single drug dose and is sealed with a membrane made from a second, tailored polymer. By altering the length of this polymer’s molecular chains, the researchers can program the membranes to burst and release the reservoir’s contents at specific times.
In an upcoming issue of Nature Materials, bioengineer Robert Langer of the Massachusetts Institute of Technology (MIT) and his colleagues unveil their new drug-delivery strategy. In one set of experiments, they loaded the sugar dextran, the anticoagulant heparin, or a growth hormone into reservoirs on separate chips. Each reservoir was sealed with a different polymer membrane.
In water, membranes made of molecules of a particular length burst after a specific amount of time. If made with longer molecules, the membranes took longer to burst. The researchers found that they could make chips that released their chemical loads in four pulses over a period of 35 to 60 days.
The MIT group also loaded individual chips with two chemicals–half of the reservoirs contained dextran and half contained heparin. In a final experiment, the researchers showed the device could function for up to 140 days.
“This is a significant contribution to the field of drug delivery,” says Nicholas Peppas, a biomedical engineer at the University of Texas at Austin. “This device opens up new methods for treating patients.”
Implanted under the skin, the chips could deliver many potent protein-based drugs that are typically delivered via injection because they readily degrade in the gut if taken orally. The chips could also be useful for delivering hormone therapies, which are most effective when released in pulses, rather than in the continuous fashion of slow-release capsules.
And then there’s the issue of patient compliance, says Peppas. “Patients forget to take their pills when they need to.” The drug chips could solve that problem, too.
“You could use these chips for multistage vaccines, such as hepatitis B, that require multiple visits to the doctor,” says Amy Richards Grayson, one of Langer’s coworkers, now at Cornell University. “That could be a really good fit for this technology.”
In previous work, Langer and his colleagues devised a silicon microchip for drug delivery. The device, equipped with a tiny battery and microprocessor, consists of reservoirs capped with gold membranes. When a voltage is applied to a membrane, its gold dissolves.
An advantage of the new polymer chip over the more-complex silicon version is that the polymer one doesn’t have to be surgically removed, says Grayson. When the chip is empty, the biocompatible materials would slowly degrade, she says.
So far, Langer’s team has fabricated chips with 36 reservoirs. However, Langer says, hundreds of reservoirs could easily fit onto a single device. MicroCHIPS of Bedford, Mass., the firm developing the silicon device, also plans to commercialize the polymer version.
****************
If you have a comment on this article that you would like considered for publication in Science News, send it to editors@sciencenews.org. Please include your name and location.






