U.S. measles tally for 2015 now at 121 cases
CDC reports patients in 17 states and D.C.
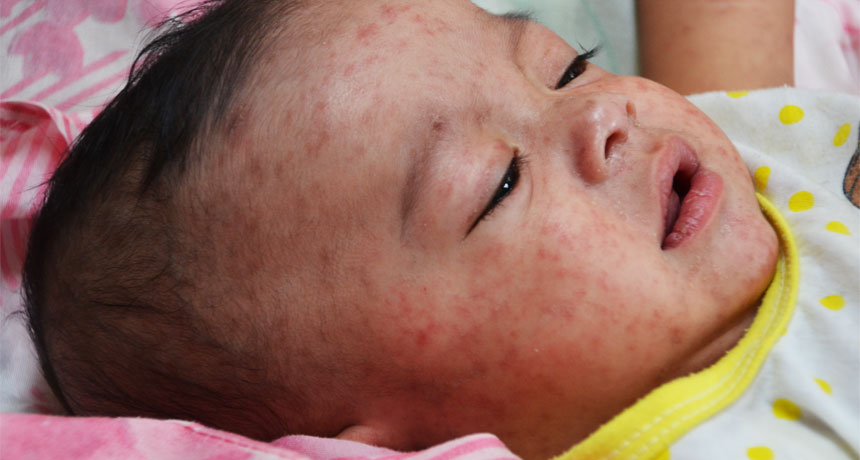
SEEING SPOTS In addition to its trademark rash, measles can cause dangerously high fevers. An outbreak in the U.S. that was jumpstarted in children attending Disneyland continues to generate new cases.
Jim Goodson, M.P.H./CDC