Whooping cough bounces back
Replacement vaccine is not so great at protecting kids
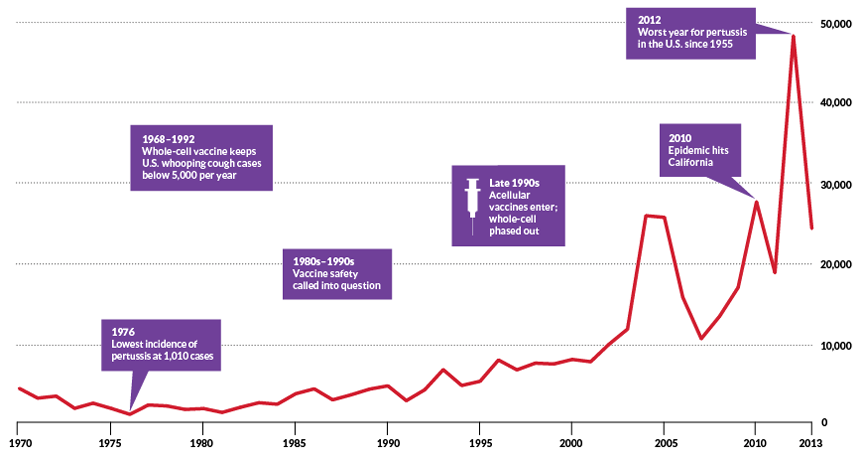
PERTUSSIS REDUX Whooping cough, a disease nearly vanquished in the United States in the 1970s, has made a comeback that coincides with a change in vaccines.
Source: CDC
Whooping cough has turned up in North America after decades of near absence, and we have only ourselves to blame.