The immune system isn’t just about defense; it works in partnership with other cells to regulate body functions.
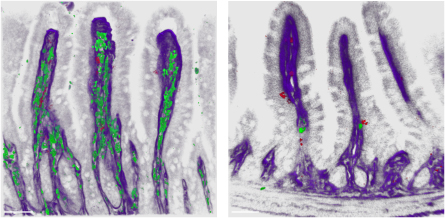
A new study shows that immune cells called B cells carry on a three-way conversation with gut microbes and cells lining the intestines to control fat uptake. The finding, reported online November 20 in Nature Medicine, challenges conventional wisdom that the immune system’s only job is to fight bad guys. The new knowledge also may shed some light on why people with HIV and other chronic infections become malnourished, and it might suggest ways to treat malnutrition.
The study grew out of a comment that systems biologist Andrey Morgun, now a researcher at Oregon State University in Corvallis, once heard at an immunology conference. “A speaker mentioned that the immune system isn’t just a war machine,” Morgun says.
For Morgun and his wife and research partner, Natalia Shulzhenko, also now at Oregon State, the idea was intriguing. Both had training in clinical immunology, where the immune system is thought of as a protective mechanism, not something involved in daily life outside the disease process, Morgun says. While working at the National Institute of Allergy and Infectious Diseases in Bethesda, Md., the couple convinced their research adviser there, immunologist Polly Matzinger, that the idea was worth testing.
Other researchers have noted that mice lacking antibody-producing B cells have abnormal digestive systems. In particular, the mice have difficulty absorbing fat from the diet and become malnourished. In the new study, Morgun and Shulzhenko discovered that B cells’ ability to make a type of antibody called immunoglobulin A, or IgA, is important for fat uptake. IgA is secreted in tears, saliva, milk and mucus, and helps cells lining the intestine maintain a healthy relationship with friendly bacteria.
The researchers reared mice without B cells in a sterile environment so the mice also lacked gut bacteria. The mice didn’t have a problem absorbing fat, despite their lack of immune cells. That told the researchers that intestinal microbes are involved in the process, but exactly what the microbes do to change fat uptake is still unknown.
A closer look at cells lining the intestine, called epithelial cells, showed that those cells have two jobs — self-defense and metabolism, including absorbing fat. Somehow, IgA antibodies produced by B cells trigger gut microbes to send a signal to the epithelial cells. Those cells then determine whether to devote more resources to protecting themselves, by making antimicrobial compounds, or to carry on absorbing fat and other nutrients from food.
Andrew Gewirtz, an immunologist at Georgia State University in Atlanta, draws a comparison between this newly identified role for the immune system and community services such as crowd control performed by the police: “The police don’t just show up when there’s a crime.”
Intestinal epithelial cells taken from people who have immune defects, such as those caused by HIV or a genetic condition called common variable immunodeficiency, behave similarly to those from mice lacking B cells, the researchers found. That raises the possibility that those people might be treated for malnutrition by giving them IgA antibodies.







