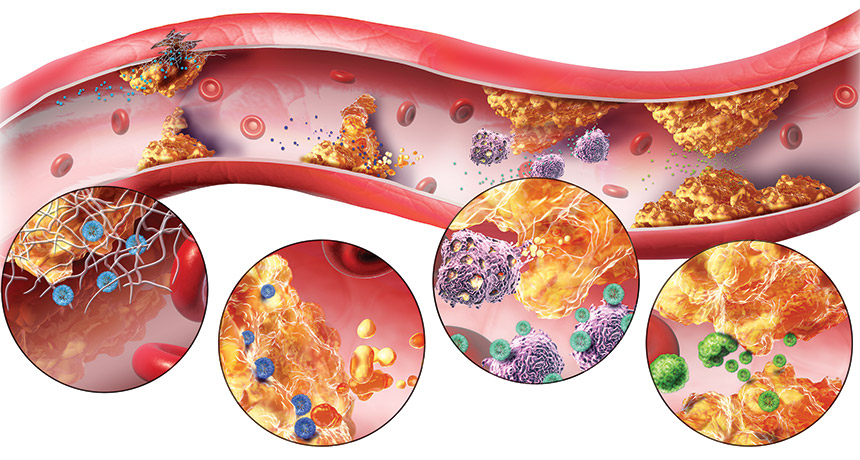
NANO VARIETY Nanoparticles can repair blood vessel damage, break up plaques, stop immune molecules from overreacting and even respond to the pressure of plaque-narrowed vessels in animal studies.
Nicolle Rager Fuller

NANO VARIETY Nanoparticles can repair blood vessel damage, break up plaques, stop immune molecules from overreacting and even respond to the pressure of plaque-narrowed vessels in animal studies.
Nicolle Rager Fuller